Diabetes, a chronic condition affecting over 100 million people, can significantly impact vein health. In fact, a study from Oxford University found that about 30 percent of people with varicose veins also have diabetes.
While diabetes can contribute to varicose veins, it’s not the sole cause. Many factors, including genetics, age, pregnancy, and prolonged standing or sitting, can contribute to the development of visible veins and other signs of vein disease.
Let’s review the link between varicose veins and diabetes, why there’s an increased risk of varicose veins in diabetics, and how to protect vein health if you have the condition.
Test Your Knowledge on Varicose Veins
An In-Depth Look at Varicose Veins and Diabetes
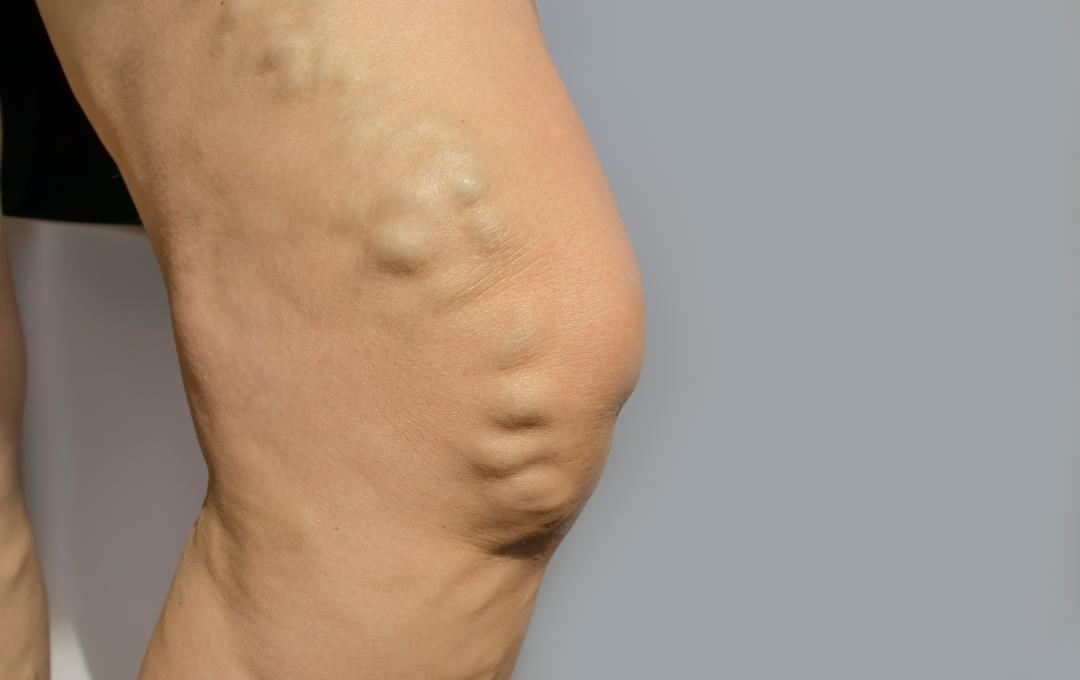
Varicose veins are swollen veins that become stretched over time due to damaged vein valves.
Vein valves usually act as one-way doors, moving blood from the lower parts of the body back to the heart. Valves that don’t work correctly will lead to blood pooling in the legs, resulting in enlarged veins and symptoms like leg pain and swelling. Other symptoms include:
- Leg fatigue
- Aching in the calves
- Burning or itching sensations around the vein
- Restless legs, especially at night
These symptoms often indicate an underlying condition known as chronic venous insufficiency, or vein disease. If untreated, symptoms can worsen and increase the risk of or . If you’re unsure your symptoms are related to vein disease, take our vein health assessment.
Why People with Diabetes Are at an Increased Risk for Varicose Veins
Varicose veins and type 2 diabetes share similar risk factors; however, each risk factor affects the body in different ways. These risk factors include:
- Obesity—Excess weight can add pressure on your veins and affect how the body uses insulin.
- Genetics—A family history of either condition increases the risk.
- Sedentary lifestyle—Being inactive can lead to weight gain, which can affect blood flow and blood sugar levels.
- Smoking—Cigarettes and vapes restrict blood circulation while also affecting blood sugar levels.
Addressing these risk factors can help reduce your risk or manage symptoms.
How Diabetes Affects Veins
Diabetes can significantly harm vein health. While this condition does not directly cause varicose veins, high blood sugar levels can damage blood vessels. This makes it harder for the veins in the legs to return blood to the heart.
Chronic inflammation, often associated with diabetes, further contributes to the damage. Neuropathy, a complication of diabetes, can mask symptoms of vein disease, delaying diagnosis and treatment.
When diabetes and varicose veins are left untreated, they can increase the risk of complications that can impact mobility and overall health. Addressing these conditions with the help of trusted health care providers can lower those risks and reduce symptoms.
How to Protect Your Veins if You Have Diabetes
If you have diabetes, here are some ways you can maintain healthy blood flow:
- Maintain an active lifestyle, especially if you have a job that involves sitting or standing for long periods.
- Wear compression socks, which apply gentle pressure to help bring blood from the legs to the heart.
- Adopt a diet rich in vitamins and nutrients, such as leafy green vegetables, ginger, and berries, for example.
- Continue monitoring blood sugar levels.
- Find time to exercise for at least 30 minutes a day, which can include low impact activities, such as walking or cycling.
- Quit smoking if you do.
These methods can help prevent varicose veins and vein disease. However, these lifestyle habits will not reverse the damage caused by these conditions. If you are diabetic and have varicose veins, consult a vein specialist to discuss any symptoms you have, and explore treatment options to reduce the appearance of veins and improve blood flow.
Varicose Vein Treatment at USA Vein Clinics
USA Vein Clinics is equipped with experienced vein specialists who perform various, minimally invasive procedures that effectively target damage caused by vein disease. These treatments include:
- Endovenous laser vein treatment (EVLT)
- Varithena vein treatment
- Ultrasound-guided sclerotherapy
- ClariVein®
- VenaSeal™
- Radiofrequency ablation (RFA)
The nonsurgical nature of these procedures means there’s no need for incisions or an extended hospital stay. In fact, patients can go home shortly after their procedure and expect a faster recovery than surgery.
In addition to shorter procedure and recovery times, many research studies report that these procedures are effective in reducing symptoms and the appearance of varicose veins. For example, a study from the National Institutes of Health found that EVLT was over 95 percent effective against varicose veins.
Addressing varicose veins if you have diabetes can help reduce your risk of complications. If you’re concerned about your risk, appointments can be made easily online or by calling 888.768.3467. With over 168 locations nationwide, advanced vein care is closer than you think.
Frequently Asked Questions
Are varicose veins a sign of diabetes?
Varicose veins are not a sign of diabetes; however, both conditions share similar risk factors. High blood sugar from diabetes can damage veins, making blood flow in the legs stagnant and causing the veins to bulge.
Can diabetes cause varicose veins?
Diabetes doesn’t directly cause varicose veins, but the effects of diabetes can lead to various conditions, including varicose veins and heart disease.
Can diabetes cause deep vein thrombosis (DVT)?
Diabetes can increase the chance of deep vein thrombosis because of how the condition affects the body. Diabetes can impair the immune system and hinder blood flow, triggering the body to respond by clotting the blood.
Is vein treatment safe for people with diabetes?
Vein treatments are safe for people with diabetes when they’re performed by an experienced vein specialist. If you are considering vein treatment, a vein specialist can review your medical history and determine which treatment works best for your condition.