Are you dealing with tired, achy legs? It might be more than just getting older — it could be venous reflux disease, also known as vein disease. While the veins in the legs typically help return blood toward the heart, venous reflux disease impairs this function, causing blood to flow backward instead.
Leaving the condition untreated can lead to worsening symptoms and an increased risk of complications, such as non-healing sores and a blood clot called (DVT). If you are concerned that you have venous reflux disease, understanding the symptoms and risk factors can help you take proactive steps to protect your vein health.
What is Venous Reflux Disease?
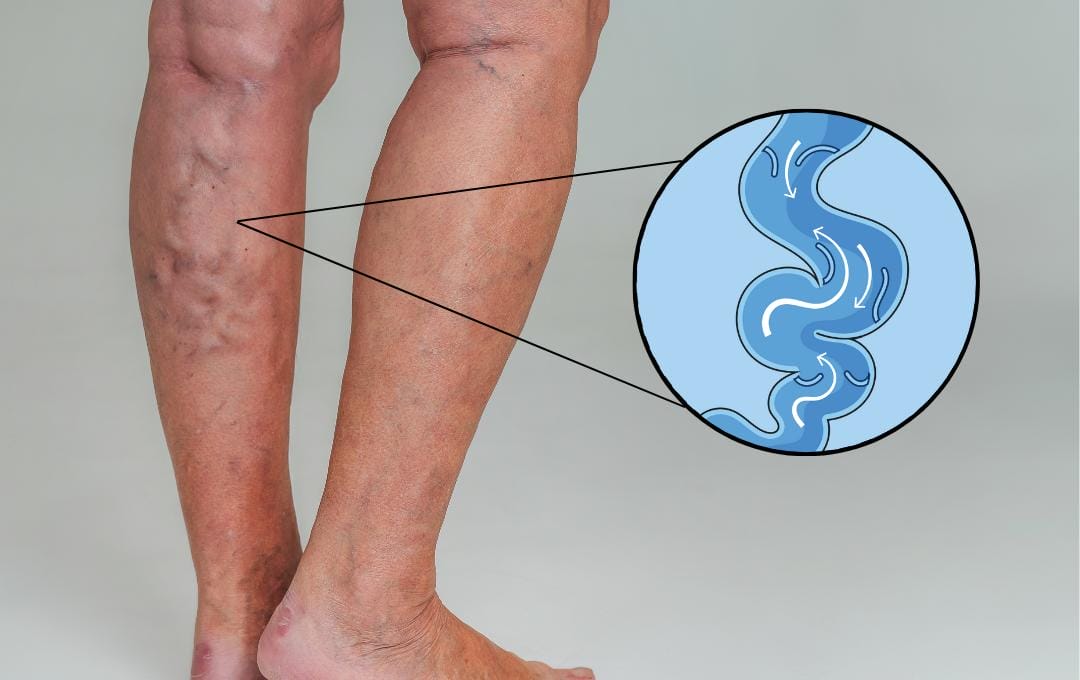
Venous reflux disease, or chronic venous insufficiency (CVI), is the underlying cause of varicose veins. While these bulging veins are the most visible symptom, they result from blood pooling in the legs. While venous reflux is the primary reason, the symptoms can also be triggered by past injuries or blood clots.
Venous reflux occurs when tiny, delicate valves inside the veins of the legs become weak or damaged, making it difficult for blood to return to the heart. As a result, blood flows backwards and pools in the legs. This increased pressure causes veins to stretch, distort and bulge through the skin.
Venous reflux disease is an ongoing condition. Once the damage to the veins starts, the refluxing veins worsen over time, which is why proper treatment is important for maintaining your vein health.
Deep Venous Reflux vs. Superficial Venous Reflux
Although patients with venous reflux may experience similar symptoms to superficial venous reflux, such as leg pain, swelling, and varicose veins, the location of the affected veins is a key difference. Reflux may occur in superficial veins, deep veins, or both. Each type of reflux will require a personalized evaluation to determine the best treatment.
What Is Superficial Venous Reflux?
Superficial venous reflux affects veins closer to the skin’s surface (superficial veins). These smaller veins act as a pathway to the deeper veins inside the body. When valves inside superficial veins weaken, the reflux causes the veins to bulge and twist, leading to the appearance of varicose veins.
Superficial venous reflux is commonly diagnosed with an ultrasound and is often treated with minimally invasive procedures that redirect blood flow through healthier veins.
What Is Deep Venous Reflux?
Deep venous reflux impacts larger veins inside the leg that carry most of the blood back to the heart. Because deep veins are vital to circulation, they cannot simply be closed.
Treatment for deep venous reflux typically focuses on improving blood flow, reducing venous pressure, and managing symptoms. When venous reflux affects both superficial and deep veins, treating superficial venous reflux helps reduce the strain on deeper veins and relieve symptoms.
What Causes Venous Reflux in the Legs?
While the main cause of venous reflux is weakened or damaged veins, various factors can contribute to the disease, including:
| Risk Factors | Link to Venous Reflux Disease |
| Family History | Vein disease can be hereditary. |
| Inactivity | Long periods of standing or sitting slow blood flow and strains veins. |
| Excess Weight | Being overweight adds pressure to the leg veins, worsening symptoms and reflux.1 |
| Smoking | Smoking damages blood vessels and raises blood pressure inside the veins. |
| Gender | Women are more likely to develop venous reflux |
| Pregnancy | Expectant mothers have an increased blood volume to support the developing fetus, which enlarges the veins in the legs. |
| Age | Veins lose elasticity over time, making vein dysfunction more likely. |
Venous Reflux Disease Symptoms
Common symptoms of venous reflux disease include:
- Swelling of the ankles or legs (edema)
- Cramping, aching, itching, or heavy sensations
- Throbbing pain that eases when you elevate your legs
- Weak or tired legs
If you are concerned you may have symptoms related to venous reflux disease, take our symptom quiz below for additional insights.
Duplex Ultrasound for Venous Reflux Mapping
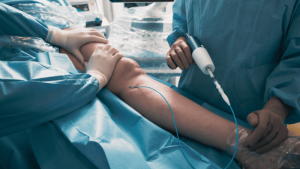
A duplex ultrasound is one of the most important diagnostic tools used to evaluate venous reflux disease. This noninvasive imaging test allows a vein specialist to see how blood is flowing through the veins in real time and identify where faulty valves may be allowing blood to move backward.
During venous reflux mapping, ultrasound is used to examine the superficial and deep veins in the legs. The test helps determine which veins are affected, how severe the reflux is, and whether there are other concerns, such as obstruction or a history of clotting. This detailed “map” of the vein system gives the specialist the information needed to recommend the most appropriate treatment plan.
At USA Vein Clinics, duplex ultrasound plays an important role in confirming the underlying cause of symptoms such as varicose veins, leg swelling, heaviness, aching, cramping, itching, and skin changes. Because venous reflux can occur below the surface, symptoms are not always visible from the outside. Ultrasound helps identify the source of the problem so treatment can target the unhealthy vein rather than only addressing surface-level symptoms.
This test is typically performed in-office and does not require incisions, anesthesia, or downtime. Once the results are reviewed, your vein specialist can explain whether venous reflux is present and discuss minimally invasive treatment options that may help improve circulation and relieve symptoms.
How Venous Reflux Disease is Treated
Treatments for venous reflux disease use advanced technology to target affected veins. A Doppler ultrasound evaluates blood flow to identify reflux, after which a vein specialist seals the faulty veins using specialized catheters or injections. As a result, blood reroutes through healthier veins, alleviating symptoms and supporting a faster recovery.
Most venous reflux treatments are minimally invasive and can be personalized to treat each patient’s condition. Because these procedures are performed in outpatient settings, patients can return home the same day with minimal side effects. Patients can also resume light activities shortly after treatment.
Learn More About Venous Reflux Treatments
When to See a Specialist for Refluxing Veins
If you notice common venous reflux signs such as enlarged leg veins, leg pain, or swelling, consult a vein doctor. The sooner a vein specialist treats the condition, the lower the risk of complications, such as skin discoloration, non-healing sores, and deep vein thrombosis (DVT).
Reasons you might want to consult a vein doctor include:
- Personal Assessment: A healthcare professional can evaluate your specific symptoms and risk factors. They can determine if your symptoms indicate venous reflux disease and recommend appropriate treatment options based on your condition.
- Diagnosis Confirmation: Identifying venous reflux can help rule out other causes of leg pain and swelling while ensuring appropriate treatment.
- Treatment Recommendations: Tailored treatment plans can be made based on the severity of your condition. These plans may include lifestyle changes, compression stockings, or medical procedures.
- Prevention of Complications: Early diagnosis and treatment can help prevent the progression of venous reflux disease and reduce the risk of complications like DVT.
- Pain Management: If you’re experiencing pain or discomfort associated with venous reflux, a vein doctor can provide effective pain management strategies.
Find Relief from Venous Reflux at USA Vein Clinics
Leg pain, swelling, fatigue, and heaviness are common signs of venous reflux—and because the condition is progressive, these symptoms often worsen without proper treatment. Addressing vein disease early can help relieve discomfort, improve circulation, and prevent symptoms from interfering with daily life.
At USA Vein Clinics, patients receive focused medical care designed to treat the underlying cause of venous reflux. From a diagnostic ultrasound to a personalized, minimally invasive treatment plan and follow-up care, our vein specialists guide patients through every step with clarity and compassion.
For many patients like Linda A., that patient experience makes a meaningful difference.
“Doctor Horng provided me with the best treatment she could offer,” said Linda A. “She took extra time to help me understand the decisions necessary for my specific issue. I have never met a doctor who seemed genuinely concerned about me as she did.”
Venous reflux disease does not have to take over your life. If you’re experiencing symptoms, a consultation with a vein specialist can provide answers—and a clear path toward relief. With over 160 locations located nationwide, USA Vein Clinics makes it easier to find expert care close to home.
Online scheduling is available to help you find a clinic near you, or you can speak with a Care Team Member by calling (888) 768-3467 for assistance with scheduling and next steps.
Frequently Asked Questions
Is venous reflux dangerous?
Venous reflux, while not a medical emergency, can be dangerous if left untreated. As the disease progresses, the risk of developing deep vein thrombosis, a dangerous blood clot, increases.
Does venous reflux go away?
Venous reflux cannot go away on its own. This condition permanently damages veins, and symptoms will worsen the longer it’s left untreated.
Can venous reflux lead to other problems?
While untreated venous reflex does not directly cause other serious issues like heart disease, it can significantly strain the cardiovascular system. If untreated, venous reflux symptoms can worsen and increase the risk of non-healing wounds and dangerous blood clots known as deep vein thrombosis (DVT) and pulmonary embolism.
Sources
- Huw O Davies, et al., “Obesity and lower limb venous disease – The epidemic of phlebesity,” Phlebology, https://pubmed.ncbi.nlm.nih.gov/27178403/