So, you are experiencing pain or discomfort in your legs and think it may have something to do with your circulatory system. You’ve googled your symptoms and have seen terms such as arterial insufficiency, venous insufficiency, arterial ulcers, venous ulcers, and you are now dealing with information overload.
In this blog we will discuss the difference between the arterial and venous systems, their role in peripheral vascular disease (PVD) and what you can look for to determine if you or a loved one may suffer from peripheral arterial disease (PAD) or chronic venous insufficiency (CVI).
What is the difference between veins and arteries?
Before we dive into the different types of vascular disease that may affect you or your loved ones, let’s quickly review the circulatory system. The purpose of the arterial system is to carry clean, oxygenated, nutrient rich blood away from the heart to the body’s organs and limbs. The venous system’s job, on the other hand, is to pick up the carbon dioxide and waste products from the cells and return the blood to the heart and lungs to be cleaned and begin the cycle again.
Peripheral vascular disease
Peripheral vascular disease (PVD) describes a disease process or disorder with the veins and/or arteries in the body, excluding those involved with the heart and brain. The most common types of PVD include peripheral arterial disease (PAD) and chronic venous insufficiency (CVI).
Let’s take a deeper dive into each.
Arterial insufficiency, also known as peripheral arterial disease
Arterial insufficiency, more commonly known as peripheral arterial disease or PAD, occurs when the arteries bringing oxygen and nutrients to the limbs become blocked by plaque or fatty deposits, preventing the necessary amount of oxygen and nutrients from reaching the skin and tissue in the legs.
Common risk factors leading to peripheral artery disease include:
- Family history
- High blood pressure
- History of heart disease or stroke
- Sedentary lifestyle
- Age of 50+
- Obesity
- Diabetes
- History of smoking
- High cholesterol
Venous insufficiency, also known as chronic venous insufficiency or varicose vein disease
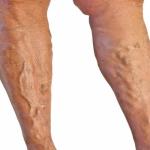
Venous blood picks up the carbon dioxide and waste products and then travels back toward the heart and lungs to be cleaned. In the legs, venous flow travels against gravity using one-way valves in conjunction with the contraction of the leg muscles to move flow up and out of the legs. When those valves fail, however, blood pools in the veins, causing them to stretch and eventually, become varicose veins. What is commonly referred to as varicose vein disease is actually called chronic venous insufficiency (CVI).
Common risk factors leading to varicose vein disease include:
- Obesity
- Pregnancy
- Menopause
- Family history
- Injury such as accidents, surgeries, prior blood clots (involving the leg)
- Age
- Smoking
- Sitting or standing for extended periods of time
While there are many things that can contribute to venous insufficiency, the most common risk factor is a family history.
Signs and symptoms of chronic venous disease vs. peripheral artery disease
Now that we understand what CVI and PAD are, as well as the risk factors, let’s look at their signs (what you see) and symptoms (what you feel), to determine what may be impacting you or your loved ones.
Signs and symptoms of chronic venous disease (CVI)
- Aching, throbbing
- Heaviness
- Itching
- Burning sensation in the calf or thigh
- Restless Legs
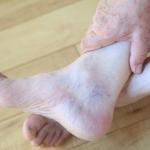
- Swelling in in the legs, ankles, or feet
- Numbness/tingling in the legs
- Difficulty standing for long periods of time
- Ulcer(s)
- Brown colored skin (often near ankles)
- Cramping, usually at night or in the evening
- Bulging varicose veins or spider veins
Signs and symptoms of peripheral artery disease (PD)
- Loss of hair on the leg
- Erectile dysfunction
- Ulcers on the toes, feet, or legs
- Poor toenail growth
- Leg, foot or toes cool/cold to the touch
- Skin changes such as: brittle, thin, shiny, or reddish-blue discoloration on the legs and feet.
- Pain or cramping in the calf, thigh or buttocks during activity that disappears when at rest
Many people are more familiar with arterial issues and often miss the signs and symptoms of vein disease that are negatively impacting their lives. In fact, vein disease is so common it affects 1 in 10 men in the United States and 1 in 3 women.
Often, we get so used to the symptoms that progress slowly over time, that we attribute our veins disease symptoms to age, hydration, activity, and other factors rather than recognize the true culprit.
Remember: No one knows your body as well as you do – you are an expert in what feels normal and abnormal. Also, while most people experience signs and symptoms of vein disease, it is not uncommon for some to experience signs but no symptoms, or symptoms but no signs. Listen to your legs.
Know the difference between arterial ulcers vs. venous ulcers
You may have noticed that one sign of both PAD and CVI is a slow or non-healing wound known as an ulcer. While both of these disease processes can cause ulcers, you can usually tell if it is caused by arterial or venous issues based on its location and appearance.
How to Identify Venous Ulcers & Arterial Ulcers
| Venous Ulcers | Arterial Ulcers | |
| TYPICAL LOCATION | Below knee, near inner ankle area | Outer side of the ankle, feet, heels or toes |
| TYPICAL PRESENTATION | Shallow but large, Irregular margins (edges) | Punched-out look, Round in shape, Well-defined edges, Even wound margins, and Deep |
| TYPICAL SIGNS | Browning or black stained skin, Bleeding, Hardening of Skin, Scabbing or flaking, Swelling, Inflammation, Discharge | Red, yellow, or black sores, No bleeding, Tight, hairless skin, Affected area cool to the touch, Legs turn red when dangling, and become pale when elevated |
| TYPICAL SYMPTOMS | Not painful, unless infected, Aching and itching | Painful, Leg pain at night |
Ulcers are an advanced sign of PVD. If you or a loved one has an ulcer, don’t wait another minute! Get in touch with your primary care physician or vascular specialist immediately.
So, what’s the fix?
So you have peripheral vascular disease, what’s the next step? The good news is, for both venous and arterial insufficiency, they are easily diagnosed and most treatments are covered by most major medical insurance companies.
Diagnosis of arterial and venous insufficiency
For both arterial and venous insufficiency, diagnosis begins with a trip to the doctor, a thorough medical history and physical exam. If CVI or PAD are suspected, an ultrasound will be required for diagnosis.
Treatment options for arterial and venous insufficiency
While surgical options are available, there are things that can be done from home to help in the maintenance of your veins and arteries through beneficial lifestyle changes.
At Home Maintenance for Chronic Venous Insufficiency
- Quit Smoking
- Maintain a healthy weight
- Stay active
- Avoid sitting or standing for long periods of time
- Wear compression socks/stockings
At Home Maintenance for Peripheral Vascular Disease
- Quit Smoking
- Maintain a healthy weight
- Stay active
- Eat foods low in cholesterol and fat
- Take medications as prescribed to help maintain blood pressure, cholesterol, blood sugar, and platelet coagulation levels
Surgical options vary greatly between arterial and venous insufficiency. While both can be very routine, surgical options for PAD will sometimes not be recommended if they are not severe enough. When surgical options are recommended, the type of procedure, post procedure physical limitations, instructions, and expectations vary greatly depending on the location and severity of the obstruction. Visit our FAQs page to more about what to expect before, during and after vein treatment.
Common procedures for peripheral vascular disease include:
- Atherectomy: A tiny cutting blade is inserted into the artery to cut away the plaque.
Angioplasty: A technique where a tiny inflatable (medical grade) balloon is inserted into an artery, then inflated to enlarge the narrowed area. - Stenting: A technique used for severely blocked arteries in which a small metal mesh sleeve is fixed inside the affected area of the artery to allow flow through. This will sometimes be used in instances of a failed angioplasty.
- Bypass: In more severe cases, a blocked artery may not be able to be reopened. In this type of case, a healthy vein or artery is used to redirect blood around the blocked section to restore blood flow.
- Amputation: In very severe cases, when arteries are too damaged and are causing tissue death, it can become dangerous to keep a piece of a limb due to the risk of infection causing death. In these severe instances, the removal of a digit, limb or piece of a limb may be required to prevent death due to infection, or a continued gradual death of the surrounding area that is currently still functioning.
With CVI, once the vein is not functioning properly, it does not improve, and over time this creates additional varicose veins so it is usually recommended that CVI be treated as signs and symptoms appear. Additionally, treatments for vein disease are considered minimally invasive with little to no pain and you can go back to your typical daily activities immediately following the procedure. You will not be sedated as only local numbing medication is used. You can drive yourself to and from your appointment.
Common procedures for chronic venous insufficiency include:
- Ablation of the Saphenous Veins: These are sterile procedures in which the saphenous veins are targeted for treatment due to their failure. This method shuts down the targeted veins using either heat or glue to collapse the vein, diverting the blood to healthy veins. There are three types of devices your physician may choose from for this process: LASER (using heat), Radiofrequency (using heat) and Venaseal (using medical grade glue).
- Ultrasound Guided Sclerotherapy: Once the saphenous veins are closed, the next step is to treat the varicose vein branches coming off the saphenous veins. These clean procedures utilize medication (sclerosant) injected into the veins, irritating the vein walls, causing them to spasm and shut down, diverting the blood into normal, healthy veins. Most patients require 1-3 sessions per leg, depending on the severity and progression of vein disease as a limited volume of medication can be used per session.
- Visually Guided Sclerotherapy: This also involves injection of a medication (sclerosant) into a diseased vein which causes the vein to spasm, shut down, and the blood diverts to normal, healthy veins. These injections target the spider and reticular veins seen on the surface of the skin. Most patients require 1-3 sessions per leg, depending on the severity and progression of vein disease as a limited volume of medication can be used per session.
What are you waiting for?
We discussed the differences between arteries and took a deeper dive into the difference between PAD, CVI as well how arterial and venous ulcers can appear on the body. Remember that you are the expert when it comes to how your body looks and feels so listen to your legs. If you think you may be suffering from peripheral vascular disease make an appointment with your physician to discuss your diagnosis and treatment options.
Make yourself and your health a priority today. Don’t wait! At USA Vein Clinics, we specialize in the diagnosis and treatment of vein disease – it’s all we do! Our dedicated team of specialists will be able to identify or rule out CVI and create a personalized treatment plan based on your needs.
Medically Reviewed By:
Dr. Yan Katsnelson is a philanthropist, business owner, and highly skilled cardiac surgeon. He is the Founder and CEO of USA Vein Clinics, which is part of USA Clinics Group, the parent company of USA Fibroid Centers, USA Vascular Centers, and USA Oncology Centers, with more than 100 facilities nationwide. Dr. Yan has established himself as a strong advocate for accessibility and affordability of the most advanced medical care close to home. His mission is to create a positive experience for each patient with compassionate, personalized, and expert care.