It’s common for spider, varicose, and other vein health conditions to run in families. Genetic factors like specific gene mutations are linked to vein health. These factors mean that someone is more likely to develop varicose or spider veins if one or both of their parents had the condition.
A vein screening can help detect and treat vein issues early and prevent complications, even if you don’t have obvious symptoms like bulging varicose veins. Many vein conditions can present with subtle signs, such as leg heaviness, ankle swelling, or even a feeling of restlessness. If you know that vein disease runs in your family and are concerned about your risk, recognizing the signs and symptoms can be the first step toward better health outcomes.
What Is Vein Disease?
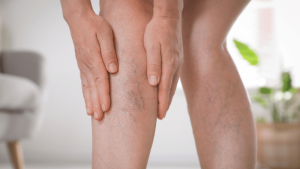
Varicose veins and spider veins are signs of underlying vein disease or venous insufficiency. Vein disease develops when tiny, one-way vein valves that pump blood back to your heart are placed under strain.
When this occurs, your valves can malfunction and cause blood to flow backward. This leads to blood pooling in the veins, which can result in the formation of varicose veins and spider veins. Most often, the legs, ankles, and feet are affected.
Vein disease causes painful and uncomfortable symptoms. Symptoms of venous insufficiency include:
- Swelling in the legs and ankles
- Leg pain that feels better when you walk or raise your legs
- Numbness or tingling sensation
- Non-healing wounds on your legs
- Difficulty standing for long periods
When caring for your veins, it is important to understand your risk factors for spider and varicose veins. Hereditary may be one of them. With this information, you can make lifestyle modifications to manage your risks.
What Causes Vein Disease?
Many contributing factors can lead to the development of vein disease. Some of these may be within your control, others, such as heredity, are not. Risk factors for vein disease include:
- Age: You have a greater risk of developing vein disease as you age.
- Sex: Women are four times more likely than men to develop varicose veins.
- Pregnancy: Due to increased blood flow and hormonal influx, pregnant women are more likely than others to be affected.
- Prolonged sitting or standing: If you have a job where you are on your feet or sitting down throughout the day, you are at higher risk for developing vein disease because of the increased pressure on your veins.
- Obesity: Excess weight puts additional strain on your veins and causes damage.
- Inactivity: Lack of physical activity affects overall blood circulation and can lead to diseased veins.
- Smoking: Along with contributing to other major medical issues, this unhealthy habit can weaken veins and reduce blood flow.
- Other underlying health conditions: Poorly managed health issues like high blood pressure and diabetes can result in strained vein valves.
We recommend consulting a vein specialist if you are at high risk for developing varicose veins. A vein specialist can closely monitor your vein health and intervene when needed. In general, early treatment leads to the best health outcomes.
The Genetic Link in Vein Conditions
While not everyone with vein conditions has a family history, research indicates a strong genetic link. Individuals who have a parent with varicose or spider veins are more likely to develop the condition. This increased likelihood is associated with two genetic factors: gene mutations and hereditary connective tissue weakness.
Gene Mutations: Scientists have identified genetic mutations that impact vein structure and function, increasing the risk of venous disorders.
Hereditary Connective Tissue Weakness: Conditions like Marfan syndrome and Ehlers-Danlos syndrome weaken the connective tissues in vein walls, making veins more prone to damage and dysfunction.
Are Varicose Veins and Spider Veins Genetic?
Family history is believed to play an important role in the occurrence of varicose veins. A National Institutes of Health study found that 61 percent of participants had a family history of varicose veins. This occurrence was more frequent in patients with a paternal family history of vein disease.
The exact genetic cause of varicose veins is not entirely understood. However, a study identified nine genes that are most likely linked to the development of varicose and spider veins. These genes influence factors such as blood pressure and blood cell traits.
Is Deep Vein Thrombosis Genetic?
Deep vein thrombosis (DVT) is a serious type of blood clot that develops in the deep veins. If left untreated, DVT can break off and travel to the lungs. This can lead to pulmonary embolism, a life-threatening situation that requires emergency medical treatment.
Although it’s not the only potential cause, genetics may play a role in the development of DVT. If you have venous insufficiency, you are considered at increased risk for DVT. Conversely, if you’ve already experienced DVT, you may be more likely to develop vein disease.
Other Contributing Factors Beyond Genetics
Genetics can play a role in varicose and spider veins. However, lifestyle, environmental factors, and hormonal changes can contribute to varicose and spider veins.
Lifestyle and Environmental Factors
Certain lifestyle factors are strongly linked to the development of vein health issues. This includes:
- Prolonged sitting: Sitting for long periods can restrict blood flow and lead to weakened veins.
- Standing for extended periods: Spending a lot of time standing can increase the vein pressure, leading to blood pooling and vein damage.
- A lack of physical activity: A lack of exercise is linked to reduced circulation and varicose and spider veins.
Hormonal Changes
The risk of varicose veins and other vein conditions increases during pregnancy due to:
- Increased blood volume: More blood circulates to support fetal development, putting extra pressure on veins.
- Hormonal shifts: Higher progesterone levels relax vein walls, making them more prone to stretching and valve dysfunction.
- Uterine pressure: As the uterus grows, it can compress veins in the lower body, slowing circulation and increasing the risk of blood pooling.
These changes make varicose veins more common during pregnancy, even for individuals without a family history. The risk also rises during menopause due to decreased estrogen levels, which can weaken vein walls and impact circulation.
Am I at Risk for Hereditary Vein Conditions?
While vein conditions often run in families, they can also occur in individuals without a known genetic link. Examining your personal and family health history to understand your risk of hereditary vein health conditions is important.
Varicose veins and spider veins can contribute to more serious health concerns if left untreated, such as:
- Blood clots
- Venous ulcers
- Deep vein thrombosis (DVT)
- Pulmonary embolism
Treating Varicose and Spider Veins
USA Vein Clinics offers state-of-the-art, non-surgical treatments tailored to each patient’s condition. Our specialists assess overall vein health and the severity of vein disease to create the most effective treatment plan.
Our advanced vein treatments include:
- Endovenous Laser Vein Treatment: This treatment uses a laser to collapse and seal veins.
- ClariVein®: This treatment closes damaged veins using a rotating fiber device.
- Varithena: Uses a specialized foam to close damaged veins.
- Ultrasound-Guided Sclerotherapy: A solution is injected to close damaged veins.
- VenaSeal™: A treatment that uses medical adhesive that is injected into the veins.
- Radiofrequency Ablation: During treatment, heat is used to close damaged veins.
- Sclerotherapy: A treatment that uses injected solution to close veins.
When to See a Vein Specialist To Access Your Hereditary Risk
Recognizing when to see a vein specialist can help detect varicose veins and other concerns before they worsen. If you notice leg swelling, visible veins that become larger over time, persistent heaviness, aching, itching, and discomfort around your veins, it may be time to seek professional evaluation from a vein specialist.
During the consultation, the specialist can assess your risk factors, discuss your symptoms and determine if further diagnostic testing is needed. Early intervention can slow progression, alleviate symptoms, and reduce the risk of complications.
Schedule your consultation: Call 888.768.3467 or click below.
FAQs
At what age do hereditary vein issues typically appear?
Hereditary vein issues typically appear after age 50. However, they can appear at any age.
Can exercise prevent hereditary vein conditions?
Exercise can help lower the risk of hereditary vein conditions, but it may not fully prevent them. However, staying active supports circulation and overall vein health.
Does pregnancy increase the risk of hereditary varicose veins?
If you are pregnant and have a family history of varicose veins, you may be at an increased risk of hereditary varicose veins.
Is chronic venous insufficiency hereditary?
Chronic venous insufficiency (CVI) can be hereditary, with studies showing a strong genetic link. If you have a family history of CVI, it’s recommended to get regular vein screenings to identify vein issues early.