Have you ever struggled with tired, achy legs at the end of the day? It could be a sign of Chronic Venous Insufficiency. Nearly half of women experience CVI in their lifetime, while impacting only 17 percent of men. It’s the underlying cause of varicose veins and spider veins and a risk factor for deep vein thrombosis (DVT).
CVI is a progressive condition that exacerbates over time and does not resolve spontaneously, even with adherence to healthy lifestyle practices. Therefore, it is imperative to consult a vein specialist upon noticing early signs of venous insufficiency.
However, the challenge is not everyone is aware of the symptoms to watch out for. Early indicators may be misconstrued as typical age-related changes, leading individuals to dismiss them without recognizing the potential seriousness of vein damage.
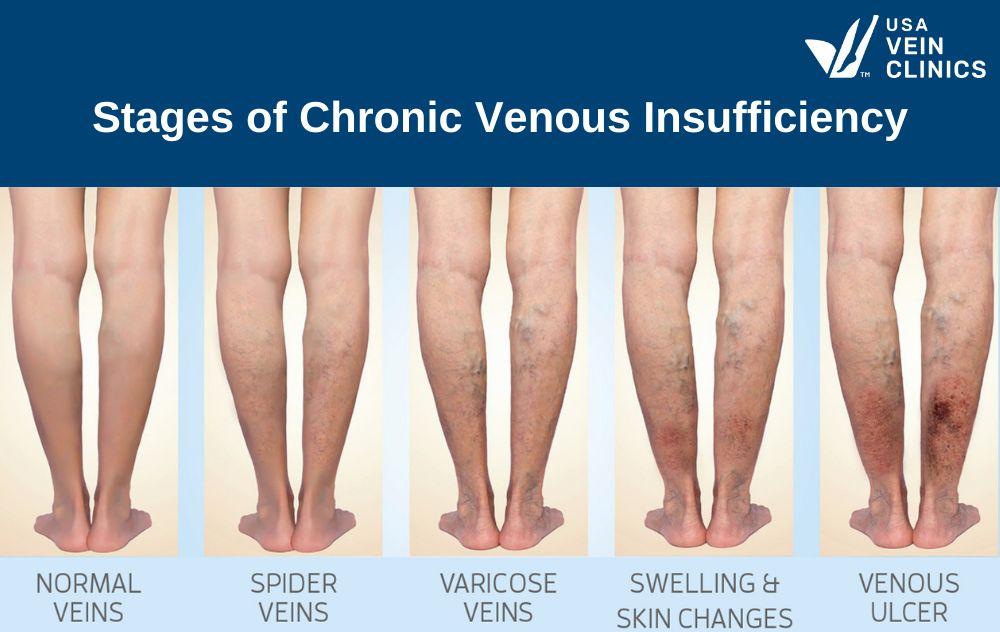
Understanding the Stages of Chronic Venous Insufficiency
Since chronic venous insufficiency is a progressive disease it is often categorized into stages (known as the CEAP classification):
-
Stage 0–1: No visible signs, or just spider veins
-
Stage 2: Varicose veins become noticeable
-
Stage 3: Leg swelling without skin changes
-
Stage 4: Skin discoloration or thickening
-
Stage 5–6: Healed or active venous ulcers
Early Stages of Venous Insufficiency
CVI, also known as vein disease, occurs when the veins in your legs become damaged.
Reasons for CVI to occur and present venous insufficiency symptoms include:
- Age: As we age, our veins naturally become less elastic and more prone to weakening.
- Pregnancy: Pregnancy puts extra pressure on the veins in your legs.
- Obesity: Excess weight strains the circulatory system, including the veins in your legs.
- Lack of exercise: Leg muscle movement helps pump blood back to the heart. Inactivity allows blood to pool in the legs.
- Family history: If close relatives have had CVI, you’re more likely to develop it.
This damage affects the proper functioning of the vein valves, disrupting blood flow regulation. Consequently, circulation problems arise, blood pressure within the affected veins increases, and various symptoms, such as skin changes and leg pain, may occur.
During the early stages of chronic venous insufficiency, your symptoms might be mild to moderate. You might have visible veins and some physical symptoms. As your everyday life isn’t impacted significantly at this point, you might not seek care.
Getting treatment promptly rather than delaying can expedite your recovery and prevent the onset of more serious symptoms.
Here are the first three stages of venous insufficiency you should be aware of:
Stage 1: Spider Veins
Visible veins underneath your skin’s surface are considered stage 1 venous insufficiency. You might notice spider veins, which are tiny, colorful, web-like veins. Like varicose veins, they most commonly impact the lower extremities; however, the face and other body areas can also be affected.
You might also see reticular veins, which are blue or purple in color but do not bulge out.
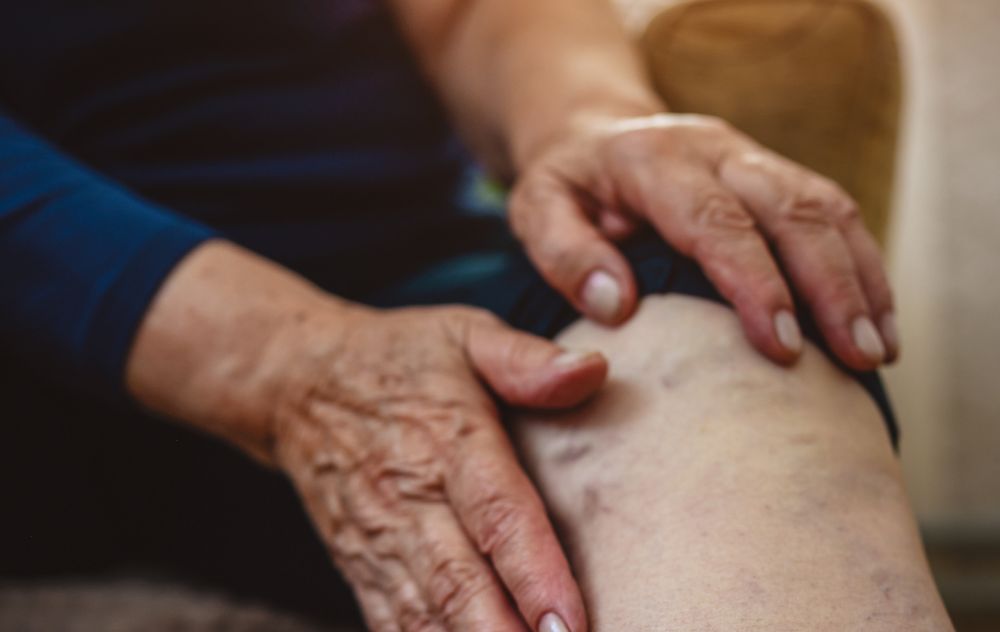
Stage 2: Varicose Veins
If you have varicose veins, your doctor might diagnose you with stage 2 chronic venous insufficiency.
Varicose veins are enlarged, twisted veins that rise above the skin’s surface. Besides being unsightly, varicose veins can cause painful and uncomfortable symptoms, including leg heaviness, restless legs, and leg cramps.
Although not all individuals experience pain or discomfort, many do. It’s also possible for leg pain and other uncomfortable symptoms to start developing after you start noticing the appearance of varicose veins.
Stage 3: Leg Swelling
When early signs and symptoms of vein disease are left untreated, additional ones are likely to occur. One chronic venous insufficiency symptom, edema or leg swelling, is a common sign of progressing vein disease.
You may notice difficulty or pain when putting on your shoes or boots. Your legs and ankles may feel heavy, making climbing stairs more difficult. This type of swelling may become severe enough to limit mobility and impact your quality of life.
Advanced Chronic Venous Insufficiency Stages
If you don’t get treatment for venous insufficiency in the early stages, your vein health can deteriorate, leading to more severe symptoms. The following are more advanced venous insufficiency changes.
Stage 4: Skin Changes
In stage 4, you’ll notice changes to your skin, such as:
- Itchy skin
- A red rash called venous stasis dermatitis
- Brown or gray markings
- Skin hardening or thickening
- Visible veins and blood vessels around your ankles, known as corona phlebectatica.
Stage 5: Healed Ulcers
As CVI progresses, wounds start forming on the skin. During stage 5, these wounds — which are known as venous stasis ulcers — heal. You might have areas on your legs that have already healed as well as open ulcers.
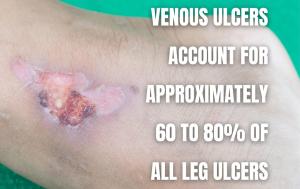
Stage 6: Open Ulcers
The last stage of venous insufficiency is characterized by venous ulcers that don’t heal easily. These ulcers can be painful. However, the greater concern lies in the risk of infection. Due to the impaired healing of your skin, these open wounds are more susceptible to becoming infected.
Why Knowing CVI Stages Matter
The earlier CVI is identified, typically in stages 1 to 3, the easier it is to treat and control. Minimally invasive treatments like endovenous laser therapy (EVLT), radiofrequency ablation (RFA), and sclerotherapy can close the malfunctioning veins, reroute blood through healthy ones, and relieve symptoms such as swelling, heaviness, pain, and fatigue.
So while you can’t undo the structural damage, you can stop the disease from progressing, improve your quality of life, and in many cases, eliminate your symptoms altogether
Request a Vein Consultation Today
Chronic Venous Insufficiency FAQs
What Are the Visible Signs of CVI?
Venous insufficiency has different stages so that you might notice certain visible signs at each stage.
- In the early stages, you’ll see visible veins, including spider veins and varicose veins. You also might notice leg swelling.
- As it advances, you’ll see skin changes, including hardened, waxy-looking skin, red rashes, and skin wounds that heal slowly or don’t heal at all.
What Does Venous Insufficiency Look Like?
Venous insufficiency manifests in various stages, each characterized by distinct visible signs. In the early stages, individuals may notice the appearance of spider veins or varicose veins, which are visible beneath the skin’s surface. These veins may present as tiny, colorful, web-like patterns (spider veins) or enlarged, twisted veins that protrude above the skin’s surface (varicose veins). Additionally, leg swelling may occur, particularly as the condition progresses.
As venous insufficiency advances, changes in the skin become more apparent. This may include the development of hardened, waxy-looking skin, red rashes (venous stasis dermatitis), and skin wounds that heal slowly or not at all. These visible signs indicate worsening vein health and should prompt individuals to seek evaluation and treatment from a vein specialist.
During Which Chronic Venous Insufficiency Stage Should You Get Treatment?
If you notice any signs of chronic venous insufficiency, it’s important to see a vein specialist. An experienced doctor can examine your symptoms and determine the stage. They will also provide a personalized treatment plan that can help restore your vein health.
USA Vein Clinics is a nationwide clinic staffed with experienced vein doctors. We can diagnose and treat your veins, no matter what stage of venous insufficiency you’re experiencing, helping to relieve your symptoms, support better circulation, and improve your overall vein health.
What Happens if Chronic Venous Insufficiency Is Left Untreated?
CVI is a progressive disease that will continue to get worse. If you have signs of early venous insufficiency, such as spider veins or varicose veins, you should see a vein specialist. Varicose veins don’t have a cure, but they are treatable.
If ignored, chronic venous insufficiency (CVI) can lead to severe complications, including deep vein thrombosis (DVT) and potentially even leg amputation. DVT is when a blood clot forms within a deep vein, usually in the legs. If left untreated, these clots can break loose and travel through the bloodstream, potentially causing a pulmonary embolism if they reach the lungs, which can be life-threatening. Additionally, untreated CVI can result in the development of venous ulcers, persistent wounds on the legs that are challenging to heal and increase the risk of serious skin infections.
There’s also the pain, swelling, and daily discomfort of the symptoms that typically appear in the more advanced stages of chronic venous insufficiency.
References:
Patel SK, Surowiec SM. Venous Insufficiency. [Updated 2023 Jul 18]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK430975/