Dealing with Varicose Veins During Pregnancy
Pregnancy brings many changes to an expecting mother’s body. Some side effects of pregnancy are positive, like thicker hair and glowing skin. Others, like unsightly or uncomfortable varicose veins, are not. While varicose veins rarely pose a risk to your physical health, if left untreated, they can lead to serious health conditions like blood clots and venous ulcers.
In this blog, we will explore:
- When Do Varicose Vein Start in Pregnancy
- Are Varicose Veins Normal During Pregnancy?
- What Causes Varicose Veins to Develop During Pregnancy?
- How to Prevent Varicose Veins During Pregnancy
- Do Varicose Pregnancy Veins Only Occur in the Legs?
- What Are Common Pregnancy Vein Symptoms?
- Will My Varicose Veins Get Worse While Pregnant?
- When to Worry About Varicose Veins During Pregnancy
- What Are My Treatment Options After Pregnancy?
Understanding the causes of varicose veins during pregnancy can help you find an effective treatment and enjoy peace of mind. If you are concerned about varicose veins, pregnancy, and vein disease, we are here to answer your questions. Learn more about these common pregnancy veins below.
When Do Varicose Vein Start in Pregnancy
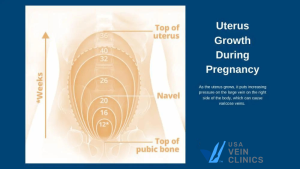
Varicose veins often develop during the second trimester and tend to worsen throughout the third trimester as you approach delivery. They may develop in the legs, vagina, and vulva. When your abdomen expands from the pregnancy, it places pressure on the inferior vena cava (the largest vein in your body), causing strain in the lower veins. This pressure only increases as your uterus continues to expand, restricting blood flow and causing the pooling that leads to varicose veins.
Are Varicose Veins Normal During Pregnancy?
The appearance of varicose veins during pregnancy is not uncommon. Increased hormone levels and physical pressure from your growing uterus cause varicose veins to develop, especially during the third trimester. For many women, varicose veins are merely a cosmetic issue, though they can also cause pain and discomfort if left untreated.
What Causes Varicose Veins to Develop During Pregnancy?
Two primary factors contribute to the development of varicose veins during pregnancy. First is the increased demand on your entire circulatory system. While your body naturally increases blood production during pregnancy, your growing uterus pushes against the large veins in the abdomen, causing increased back pressure. Excess pressure in the veins combined with increased blood volume can weaken the vein walls, causing the venous valves to malfunction. These valves are designed to prevent backflow; when they malfunction, blood pools in the veins, causing them to swell and become sensitive.
The second culprit is the influx of hormones that occurs throughout your pregnancy. Progesterone, a hormone that surges during pregnancy, causes veins to dilate. Dilated veins carry more blood, which allows a greater volume of blood to pool. Pooling blood puts stress on the vein walls and hastens the development of varicose veins.
How to Prevent Varicose Veins During Pregnancy
While varicose veins are common, taking proactive steps early in your pregnancy may help reduce your chances of developing them.
- Elevate your legs above your heart while lying down.
- Stay active and perform any exercises that increase your heart rate.
- Change positions often, including while working.
- Drink plenty of fluids.
- Wear compression stockings to take some pressure off your veins.
If you’re concerned about developing varicose veins or already have them and would like to discuss your options, call USA Vein Clinics today.
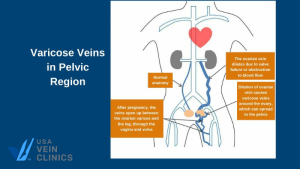
Do Varicose Pregnancy Veins Only Occur in the Legs?
Varicose veins during pregnancy typically occur in the legs but can develop in other locations. The pelvic area, including the buttocks, vulva, and vagina, is highly susceptible to varicose veins due to its proximity to the uterus. Varicose veins in these areas are most common in late pregnancy, and you may not know you have them until they’re discovered by your OB/GYN or midwife. Pay extra attention to all the changes occurring in your body to spot signs and symptoms of varicose veins sooner than later.
What Are Common Pregnancy Vein Symptoms?
Pregnancy can place a great deal of stress on the veins of your lower extremities. Although some women may not experience any issues during pregnancy, others may develop symptoms of venous issues. These can include:
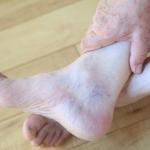
- Varicose veins: Large, twisted, often discolored veins appearing at the skin’s surface.
- Spider veins: Small, dilated blood vessels resembling a spiderweb, seen on the surface of the skin.
- Swelling: Edema or swelling in the legs, ankles, and feet.
- Cramps: Cramping can occur in the lower extremities, typically in the later stages of pregnancy.
- Itching or tingling: Reduced blood flow from vein issues can cause different sensations around problem areas.
Be sure to notify your provider if you start noticing any new or worsening symptoms of vein disease. While rare, more complicated conditions like a blood clot or ulcer may develop.
Will My Varicose Veins Get Worse While Pregnant?

Varicose veins tend to worsen as pregnancy progresses, especially in the third trimester, as increased hormones, greater blood volume, and an expanding uterus place more strain on your veins. As your veins swell and become more visible, you may also experience increased pain and discomfort.
You may be wondering what this all means after pregnancy. Often, varicose pregnancy veins resolve on their own. However, the more severe your varicose veins are, the more likely they’ll stick around afterward and require treatment. The good news is that varicose veins in your vagina or vulva almost always resolve naturally after delivery. Although painful varicose veins can be ugly and uncomfortable, they are not usually a major cause for alarm during pregnancy. However, bear in mind that vein disease has the potential to lead to serious complications. If you’re struggling with severe varicose veins during pregnancy, consult a vein specialist.
When to Worry About Varicose Veins During Pregnancy
Varicose veins are very common among pregnant women, but some situations require medical advice and possibly treatment. Although generally harmless, varicose veins can increase your risk of developing a blood clot or venous ulcers.
There are two main types of blood clots. Varicose veins most often lead to a type called superficial venous thrombosis (SVT), which does not usually travel to the lungs. However, severe varicose veins increase the risk of a blood clot called deep vein thrombosis (DVT), which can be life-threatening. In addition, the reduction of blood flow to the lower limbs can cause skin ulcers or wounds that take a long time to heal, increasing your risk of infection.
Please seek emergency care if you notice that:
- Your varicose veins take on a hard, rope-like quality
- The surrounding area seems hot, painful, or tender
- There are notable changes in vein color
- Sores develop on the skin
- There is severe swelling in either leg
These symptoms could indicate a serious problem requiring immediate medical attention. Speak with a vein specialist today if you’re concerned about your varicose veins and pregnancy.
What Are My Treatment Options After Pregnancy?
If you’ve developed varicose veins during pregnancy, treatment is available. While varicose veins can’t be treated during pregnancy, USA Vein Clinics offers minimally invasive, non-surgical treatment options that can improve your symptoms after you’ve given birth. Our specialists treat spider and varicose veins quickly at over 160 locations across the country.
If your varicose veins don’t go away on their own after pregnancy, we can help resolve the issue. Schedule an appointment online or call us at 855-768-3467. For your safety and convenience, we offer appointments either in our offices or through telemedicine.