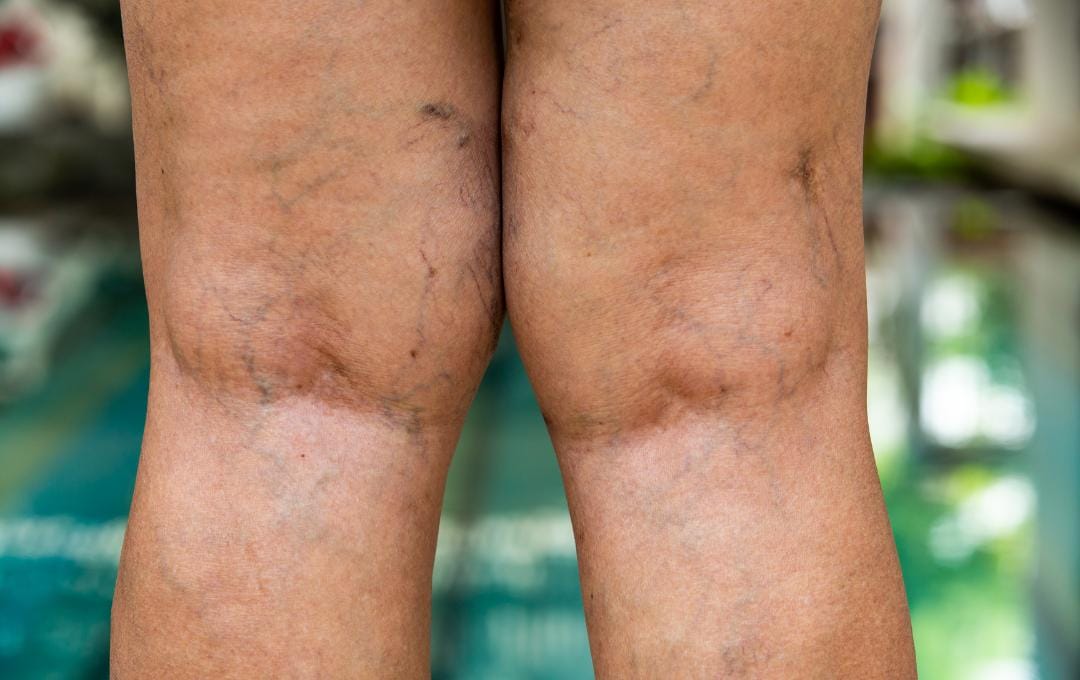
Over 30 million Americans suffer from chronic venous insufficiency (CVI), a disease that causes the veins to function improperly and worsens over time. As the vein’s internal valves weaken or become scarred, they can no longer close tightly. This damage can impede blood flow back to the heart, causing blood to pool in the legs and bringing symptoms such as swelling, discomfort, and visible varicose or spider veins.
If untreated, CVI can worsen, causing the skin to discolor or break down. Many studies also show that CVI can increase the risk of a serious blood clot known as deep vein thrombosis (DVT). Vein experts at USA Vein Clinics emphasize the importance of recognizing risk factors for CVI to help manage the condition in patients, or to help those at risk address their vein health now before complications occur.
What Causes Chronic Venous Insufficiency (CVI)?
Chronic venous insufficiency (CVI) is primarily caused by weakened or damaged valves inside the veins. Vein valves act as one-way doors, ensuring that blood continues to flow upward toward the heart. Once the valves weaken, blood flows backward, adding pressure to the veins and worsening circulation over time.
Gravity plays a significant role in the development of CVI because the veins in the legs work the hardest against gravity. This makes the legs the most susceptible to blood pooling, which can worsen with your CVI risk factors.
4 Most Common Risk Factors for Chronic Venous Insufficiency

Developing chronic venous insufficiency (CVI) significantly increases if you have more than one of the following risk factors:
Family History and Genetics
Many studies have shown a genetic link to CVI. If you have a family history of venous insufficiency, there’s a higher chance that you may develop the condition. The National Institutes of Health also reports that inherited traits or conditions, such as , can lead to weakened or damaged veins.
Age & Biological Changes
As people age, their veins naturally lose elasticity. This makes it easier for veins to weaken and lead to blood pooling. Vein disease is more common in adults over the age of 50, although it may develop earlier depending on other risk factors.
In addition to age, hormonal shifts in women—such as during pregnancy, menopause, or from birth control and hormone replacement therapy—can influence CVI risk. Increased progesterone during pregnancy can relax vein walls and cause veins to expand. A lack of progesterone later in life may cause veins to weaken over time.
Occupational Hazards: Prolonged Sitting or Standing During Long Shifts
Whether your job requires standing all day, such as in nursing or retail, or sitting for long hours at a desk or behind the wheel, prolonged inactivity increases your risk of venous insufficiency. In both scenarios, the calf muscles aren’t pumping blood effectively back to the heart, leading to leg pain, swelling, and fatigue felt at the end of the shift.
Lifestyle Factors: Obesity, Smoking, and Activity Levels
Your lifestyle may also impact your veins and potentially contribute to the development of CVI. These lifestyle factors include:
- Obesity: Excess weight adds pressure on the veins in the legs. This pressure gradually weakens vein valves and interferes with normal circulation.
- Smoking: Cigarettes and vapes constrict the blood vessels, limiting blood flow and gradually damaging veins.
- Sedentary Behaviors: When you’re inactive most of the day, the calves are not working to help pump blood back toward the heart. This causes blood to pool in the legs and the veins to bulge and twist.
What Are the Early Warning Signs of Chronic Venous Insufficiency?
Recognizing the early warning signs of CVI in the legs can help people seek care before the condition progresses. These signs include:
- Swelling
- Fatigue or heaviness
- Aching, throbbing, or cramping
- Restlessness, especially at night
- Visible varicose or spider veins
These symptoms may seem mild and easy to dismiss; however, ignoring symptoms will allow CVI to progress into more advanced stages. If you have noticed any of these symptoms, take our quick quiz to help determine if you are experiencing warning signs of CVI.
Why Early Action Matters: Complications of Untreated Chronic Venous Insufficiency
When CVI is untreated, the increased pressure inside the veins can damage the surrounding tissues.
Complications of CVI include:
- Persistent leg swelling
- Skin discoloration or thickening
- Slow or non-healing wounds or sores
- Increased discomfort or limited mobility
These symptoms can affect daily life and may require more advanced treatments to help the legs heal.
Patients with CVI may also be at risk of deep vein thrombosis (DVT), a blood clot that forms in major veins. DVT can cause significant swelling, skin redness, and pain in the affected leg. If the blood clot breaks off and travels toward the lungs, it can be life-threatening.
Early evaluation allows specialists to identify circulation issues before complications develop, and there are several steps patients can take to reduce the risk.
Preventing and Managing Chronic Venous Insufficiency
While some risk factors cannot be changed, several strategies may help prevent or manage chronic venous insufficiency (CVI). These approaches include:
- Regular physical activity to support circulation
- Maintaining a healthy body weight
- Elevating the legs when resting
- Avoiding prolonged sitting or standing when possible
- Wearing compression stockings, if recommended by a healthcare provider
When symptoms persist, minimally invasive treatments can help bring long-lasting relief. Various CVI treatment options are available that close damaged veins. Once these veins are sealed shut, blood will reroute through healthier veins, alleviating leg pain, swelling, and fatigue. Visible varicose and spider veins will fade over time.
USA Vein Clinics uses advanced, evidence-based CVI treatments designed for the modern schedule. Procedure times may vary based on the treatment and the patient’s needs; however, these office-based treatments are completed without an extended time commitment. Patients are able to drive themselves home and resume most daily activities shortly after their treatment.
The Benefits of Regular Vein Screenings at USA Vein Clinics
It’s recommended that you be screened for CVI regularly if you have symptoms or multiple risk factors. Early intervention for vein disease stops symptoms such as skin changes from progressing and helps maintain long-term vascular health. By addressing CVI in its initial stages, you can effectively resolve visible concerns and prevent more complex circulation issues from developing.
At USA Vein Clinics, our specialists use advanced diagnostic ultrasound imaging to evaluate blood flow in the legs. This technology allows physicians to “map out” the veins and detect valve damage or circulation problems that may contribute to leg pain, swelling, and heaviness. If CVI is detected, treatments can be personalized to fit each patient’s condition or needs.
Benefits of regular vein screenings at USA Vein Clinics include:
- Earlier detection of vein disease leads to early treatments
- Timely treatments reduce the risk of CVI complications
- Personalized treatment plans tailored for each patient’s needs
- Peace of mind for patients at a higher risk of vein disease
If you are at risk of CVI, or if you are noticing symptoms, schedule a screening with a vein specialist for clarity and a path to healthy legs.
Frequently Asked Questions
Is chronic venous insufficiency dangerous?
Chronic venous insufficiency is not immediately life-threatening, but it can lead to serious complications if left untreated. These complications include persistent swelling, skin changes, non-healing wounds, and an increased risk of blood clots, such as deep vein thrombosis (DVT).
What are the long-term effects of CVI?
Long-term effects may include chronic leg swelling, skin discoloration, thickened skin, and venous ulcers near the ankles. Early treatment can help reduce the risk of these complications.
Can you live a long life with chronic venous insufficiency?
Many people live long lives with CVI, especially when the condition is monitored and managed appropriately. Lifestyle changes and medical treatments can help improve symptoms and protect circulation.
How do I know that I’m in the early stages of CVI?
Early stages of CVI may include mild swelling in the ankles, leg heaviness, visible veins, or aching in the calves after standing or sitting for long periods. A vein screening with a specialist can help determine whether these symptoms are related to venous insufficiency.