If you are confused by the difference between venous and arterial ulcers, you’re not alone. Although the root cause is different, both types of ulcers can be painful, difficult to eliminate, and leave you prone to infection.
Below, we discuss arterial ulcers vs venous ulcers. If you have additional questions, our leading vein specialists are available to answer them.
What is an Ulcer?
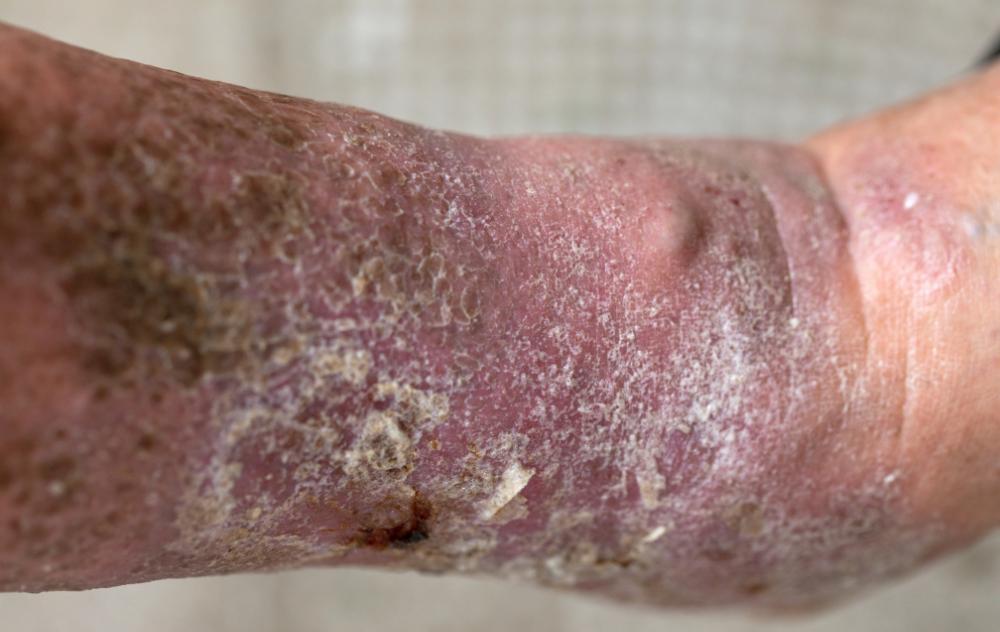
Ulcers are defined as abnormal breaks in the skin or mucous membrane. They are typically characterized as slow-healing or non-healing if healing takes more than 5-6 weeks. Although ulcers can develop anywhere on the leg, ankle, or foot, they usually develop on the inside of the calf, just above the ankle.
Ulcers are the result of poor circulation. When the affected area is deprived of essential oxygen and nutrients, your skin can become inflamed, crack or break open, and eventually lead to the formation of an open wound.
Leg ulcers can develop due to various health conditions, including vein disease and peripheral artery disease (PAD). To alleviate pain and discomfort from challenging leg ulcers, you may require treatment for the underlying health condition.
What is the Difference Between Arterial and Venous Ulcers?
Although there are many different types of ulcers, we are going to focus on two main types that affect the lower extremities: arterial vs venous ulcers.
Arterial Ulcers
These ulcers are related to diseased arteries that carry oxygen and nutrients from the heart to all body organs and tissues. Arterial ulcers may be a sign of peripheral artery disease (PAD), a serious health condition that can severely impact your quality of life. It can also place you at risk for heart attack, stroke, and limb amputation. PAD occurs when plaque builds up in the arteries, causing them to become narrowed or completely blocked.
Arterial ulcers are often found between or on the tips of toes, on the outer ankle, or in the areas where you experience pressure while walking. Left untreated, arterial ulcers can cause infection or death of tissue (necrosis). In extreme cases, amputation of the leg may be necessary.
Common symptoms of arterial ulcers include:
- Deep wound, sometimes through several layers of skin
- Wound edges are smooth
- Loss of hair on the legs
- Tenderness around the wound
- Red, yellow, or brown sores
- Leg may turn pale when elevated
- Affected area is cool to the touch
- Wound does not bleed
You may be able to minimize complications from arterial ulcers if you:
- Examine feet, ankles, and legs regularly for sores or discoloration
- Schedule an Ankle Brachial Index (ABI) test
- Exercise regularly and as frequently as comfortable
- Quit smoking as smoke hardens and clogs your arteries
- Wear footwear that fits correctly
- Manage your blood cholesterol, blood pressure, and glucose levels
- Follow treatment recommendations from a vascular specialist
Arterial ulcer treatment may involve lifestyle changes, medications, and medical procedures to treat the underlying cause: peripheral artery disease.
Venous Ulcers
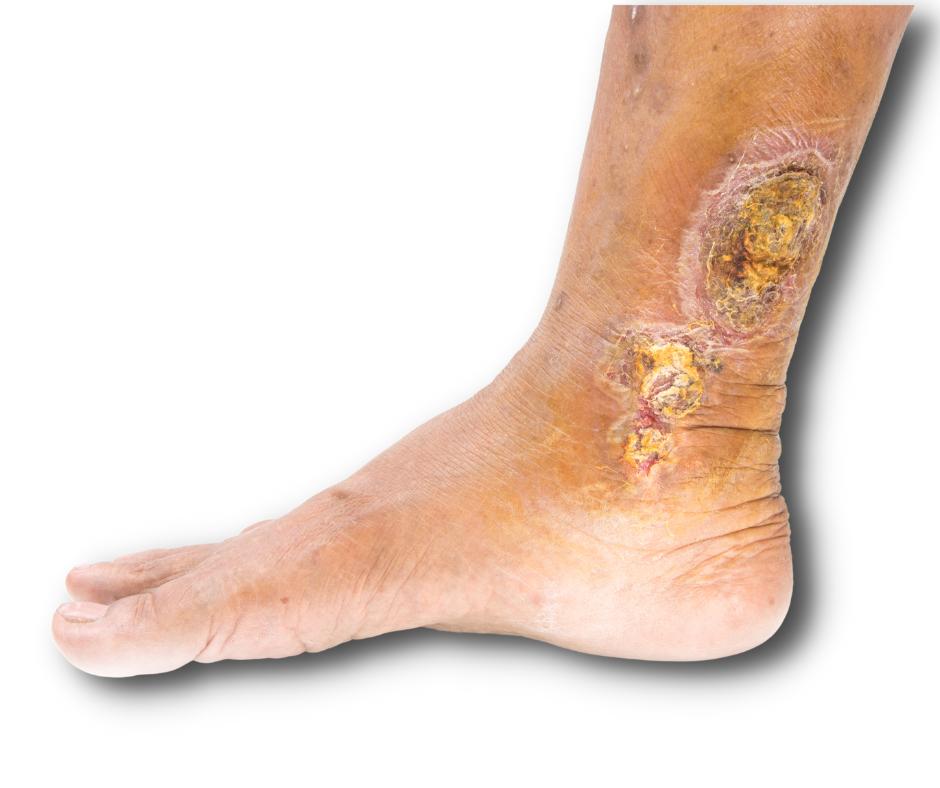
Venous ulcers are more common than arterial ulcers, accounting for over 90% of all leg ulcers. They most often occur on the lower leg or upper part of the ankle.
Venous ulcers develop when tiny, one-way vein valves become damaged. While veins are responsible for carrying blood back to the heart for reoxygenation, damaged veins can lead to symptoms like leg swelling. This further prevents the flow of blood to surrounding tissue and skin. Over time, your skin may begin to crack, break open, and form ulcers.
Common signs and symptoms of venous ulcers can include:
- A shallow wound
- Formation on the lower leg or ankle
- Discharge
- Itchy, dry skin
- Swelling, especially in the affected area
- Inflammation and redness before the wound progresses
- Achy, heavy feeling in the affected leg
- Skin discoloration
- Flakiness surrounding a wound
If you experience any of the above, we recommend consulting a vein specialist. Venous ulcers are a sign of progressing vein disease. This common health condition also causes varicose veins, spider veins, and other venous issues.
When left untreated, vein disease can lead to a range of painful and uncomfortable symptoms, including leg swelling, cramping, itching, fatigue, and venous ulcers. Vein disease can also place you at risk for deep vein thrombosis (DVT), a serious type of blood clot.
You may be able to prevent venous ulcers or keep them from getting worse if you:
- Examine feet, ankles, and legs regularly for non-healing wounds or discoloration
- Tell your doctor if you’re taking heart medications that may increase your risk of swelling
- Exercise regularly
- Maintain a healthy weight
- Quit smoking
- Move around frequently throughout the day
- Elevate your legs to alleviate pain and swelling
- Seek minimally invasive, outpatient treatment from an experienced vein specialist
Treatment Options for Venous Ulcers
If you have a venous ulcer, keep it clean, dry, and dressed to prevent infection. Minimally invasive, office-based treatment can help address the underlying cause: progressing vein disease.
At USA Vein Clinics, we offer a range of non-surgical treatments that can alleviate painful symptoms like leg swelling and venous ulcers. Most treatments take under an hour, from start to finish. Afterward, our patients can leave immediately and return to most normal activities.
Our treatments aim to seal off malfunctioning veins and divert blood flow to healthy, surrounding ones. Once healthy circulation is reestablished, your venous ulcer can begin to heal.
After treatment, lifestyle modifications may help prevent additional venous issues. We generally recommend:
- Get regular exercise
- Maintain a healthy body weight
- Avoid smoking
- Eat a healthy diet
- Manage underlying health conditions like high blood pressure and diabetes
- Avoid prolonged standing or sitting
Schedule a Consultation at USA Vein Clinics
Whether you suffer from varicose veins, spider veins, venous ulcers, or other venous issues, our vein specialists are available to help. We now perform minimally invasive, outpatient vein treatment at over 100 locations nationwide. For your convenience, we also offer telemedicine consultations.
For expert recommendations, simply give us a call at 888.768.3467 or schedule an appointment online today.
Reviewed by Dr. Yan Katsnelson, the founder and CEO of USA Vein Clinics. Dr. Yan Katsnelson is a highly skilled cardiac surgeon who completed a fellowship at the Brigham and Women’s Hospital, Harvard School of Medicine, in Boston, MA. His clinical area of expertise includes minimally invasive procedures to treat vein and vascular diseases. Dr. Katsnelson has established himself as a strong advocate for accessible, affordable, and compassionate healthcare services.