For many people dealing with chronic leg pain, heaviness, swelling, or visible vein changes, the decision to seek treatment often comes down to one question: Is vein treatment covered by insurance?
The most important thing to know is this: vein disease is a progressive medical condition and not just a cosmetic concern. When symptoms like venous reflux (poor blood flow), aching legs, swelling, or skin changes are present, vein treatment is often considered medically necessary and therefore covered by insurance.
At USA Vein Clinics, the majority of our minimally invasive vein treatments are covered by a wide range of insurance providers, including Medicare and Medicaid. When a procedure meets medical necessity criteria, your health plan is designed to help cover the cost of diagnosis and treatment often significantly reducing or even eliminating out-of-pocket expenses.
Check Your Insurance Coverage Online
What Does Medically Necessary Mean for Vein Care?
Insurance companies use the term medical necessity to determine whether a vein treatment qualifies for coverage. In simple terms, a procedure is considered medically necessary when it is required to relieve physical symptoms, correct abnormal blood flow (venous reflux), or prevent serious health complications, not just improve appearance.
When a vein condition causes pain, swelling, skin damage, or circulation problems, treatment is typically recognized as medical. Procedures performed solely for aesthetic reasons, without symptoms or medical risk, are generally classified as cosmetic.
Symptoms That Commonly Establish Medical Necessity
Insurance approval is based on documented symptoms and diagnostic findings, not appearance alone. From an insurer’s perspective, medical necessity is often established by the following:
-
Persistent Leg Pain or Heaviness
Aching, throbbing, or cramping that interferes with daily activities or work. -
Clinical Edema (Leg Swelling)
Visible or pitting swelling in the legs or ankles that affects comfort or mobility. -
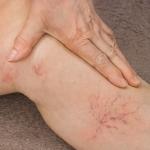
Skin Changes (Stasis Dermatitis)
Brown discoloration, redness, itching, or thickened skin near the ankles—signs of chronic venous pressure. -
Venous Ulcers or Non-Healing Wounds
Open sores that indicate advanced vein disease and an increased risk of infection. -
Nocturnal Leg Cramps or Restless Legs
Painful nighttime cramping (“charley horses”) that disrupts sleep. -
Documented Venous Reflux
Abnormal backward blood flow confirmed through Duplex Ultrasound vein mapping.
How Medical Necessity Is Determined
Medical necessity is not decided by guesswork. At USA Vein Clinics, board-certified vein specialists follow a structured, insurance-aligned process:
-
Comprehensive Clinical Evaluation
A detailed review of symptoms, medical history, and lifestyle limitations. -
Duplex Ultrasound Vein Mapping
A real-time diagnostic scan to identify failed valves and precise reflux patterns. -
Insurance-Aligned Documentation
Medical records prepared to meet payer-specific criteria and maximize approval likelihood.
Important: Many insurance denials occur not because treatment isn’t necessary but because symptoms or ultrasound findings were not properly documented by a general practitioner or initial provider. A specialized second evaluation is often the key to reversing a denial and securing coverage.
Which Vein Conditions Qualify for Insurance Coverage?
While every insurance plan is different, most providers follow similar medical necessity guidelines. If your condition significantly impacts your quality of life or poses a risk of complications like blood clots, your treatment is typically eligible for coverage.
Commonly Covered Conditions:
| Condition | Key Symptoms | Why Insurance Covers It |
|---|---|---|
| Chronic Venous Insufficiency (CVI) | Heaviness, skin changes, aching | To prevent permanent skin damage and ulcers. |
| Symptomatic Varicose Veins | Throbbing, “rope-like” veins, swelling | To resolve physical pain and mobility issues. |
| Venous Stasis Ulcers | Open sores, slow-healing wounds | To prevent infection and serious tissue loss. |
| Restless Legs Syndrome (RLS) | Nighttime “creepy-crawly” sensations | When linked to venous reflux, RLS is a significant sleep disruptor. |
| Superficial Thrombophlebitis | Red, painful, hardened veins | To monitor and prevent Deep Vein Thrombosis (DVT). |
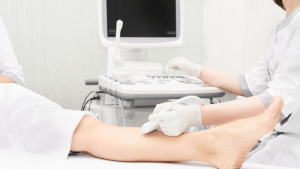
The Role of Duplex Ultrasound in Your Approval
Insurance approval cannot be based solely on a visual exam. Insurers require objective evidence of failed vein valves to determine medical necessity.
At USA Vein Clinics, we perform a Duplex Ultrasound during your initial visit. This advanced scan maps your blood flow in real time. By documenting the exact duration of venous reflux (blood flowing backward), we provide the clinical proof your insurance provider needs to authorize your treatment.
Did you know?
Many patients who were previously denied coverage at other clinics find success with us because our ultrasound mapping is specifically designed to meet stringent insurance coding requirements.
Get personalized answers tailored to your needs.
Types of Insurance Coverage for Vein Treatment
Coverage for vein treatment depends on your specific insurance plan, but most major providers follow similar medical necessity guidelines. At USA Vein Clinics, we are in-network with a wide range of providers to ensure you can access care without unnecessary delays.
Below is an overview of the most common insurance types that cover medically necessary vein treatment:
1. Private Health Insurance (PPO & HMO)
Most private insurers cover vein treatment when symptoms such as pain, swelling, skin changes, or venous reflux are documented. We work with all major national and regional providers, including:
-
Blue Cross Blue Shield (BCBS)
-
UnitedHealthcare (UHC)
-
Aetna
-
Cigna
-
Humana
Coverage requirements typically include documented symptoms, Duplex Ultrasound confirmation, and evidence of venous reflux.
2. Medicare and Medicare Advantage
Medicare Part B generally covers vein treatment when it is medically necessary. Because vein disease is often progressive, Medicare frequently covers evaluation, ultrasound diagnostics, and minimally invasive procedures for:
-
Chronic Venous Insufficiency (CVI)
-
Symptomatic Varicose Veins
-
Skin changes or venous ulcers
3. Medicaid
Medicaid coverage is state-dependent, but medically necessary vein treatment is frequently covered when complications are present. Our specialists are experts at navigating:
-
State-specific clinical requirements
-
Prior authorization processes
-
Documentation of symptoms and diagnostics
4. Employer-Sponsored & PPO Plans
Employer-based plans often provide broader coverage and more flexibility, making it easier to access vein specialists without a primary care referral.
Important Note About Coverage: Even with the best insurance, approval depends on precise documentation. Many denials occur because a general practitioner didn’t record findings correctly. Our team aligns every medical record with your specific insurer’s requirements before treatment begins to maximize your chance of approval
How to Verify Your Insurance Coverage for Vein Treatment
Checking your coverage shouldn’t be a hurdle to getting healthy. At USA Vein Clinics, our dedicated team of insurance specialists handles the “red tape” for you. We want to ensure you understand your benefits before you walk through our doors, so you can make the most informed decision about your treatment.
You can verify your coverage in three easy ways:
1. Instant Online Tool
Use our secure online insurance verification tool to enter your provider details and get your eligibility in real-time. It takes less than 60 seconds to get the information you need no waiting, no commitment.
2. Speak with a Specialist
Call us at 888.768.3467. Our team will work directly with your insurance provider to get a full breakdown of your benefits, including whether conservative therapy (like compression stockings) is required first.
Contact us now to get all your questions answered.
3. During Your Initial Consultation
When you book your first evaluation, we automatically verify your primary and secondary insurance as part of the check-in process—no extra steps needed.
Note: Verifying your insurance is a no-obligation process, it’s just our way of ensuring you have full transparency and peace of mind before deciding on treatment.
Understanding the Costs of Vein Treatment: What to Expect
The total cost of vein treatment is based on your personalized needs. Since we offer FDA-approved, minimally invasive procedures, most treatments are performed in-office in under an hour, helping you avoid the high costs associated with hospital stays and general anesthesia.
Factors That Determine Vein Treatment Cost
Anesthesia
The need for anesthesia can significantly affect the overall cost of vein treatments. Procedures requiring local or general anesthesia may cost more due to the involvement of additional medical staff, equipment, and medication.
Number of Treatment Sessions
Some vein conditions may require multiple treatment sessions to achieve optimal results. The total cost increases with the number of sessions needed, which depends on the severity of your condition and the type of treatment selected.
Treatment Procedure
Different vein treatments, such as sclerotherapy, laser therapy, or endovenous ablation, have varying price points. The complexity and duration of the procedure often determine the cost. The team at your local USA Vein Clinics can break down the costs of each treatment. Call 888-768-3467 to learn more.
Insurance Coverage
Your insurance plan greatly influences the out-of-pocket cost of vein treatment. Coverage depends on your provider, the type of insurance (HMO or PPO), if your provider is in-network or out-of-network, and whether the treatment is medically necessary.
Out-of-Pocket Costs
No matter your insurance coverage, you will be responsible for out-of-pocket costs. The exact costs can depend on your specific plan but often include:
Copay: This is the fixed amount you must pay for a covered healthcare service. Insurance plans with lower monthly premiums often have higher copays, and vice versa.
Coinsurance: Some health insurance plans require paying a percentage of expenses after meeting your deductible instead of a co-pay. For example, an 80/20 plan means that after reaching your deductible, your plan will pay 80% of expenses. You will be responsible for the other 20% until you reach your plan’s out-of-pocket maximum.
Deductible: This is the amount you pay for covered services before your health insurance plan takes over and starts to pay. If you have a $1,000 deductible, you must pay for all healthcare services until costs reach $1,000. Not all insurance plans involve a deductible. Deductibles will restart at the beginning of a new plan year.
Financial Options for Every Patient
We believe that financial constraints shouldn’t prevent anyone from receiving the vein care they need. If you have a high-deductible plan or are seeking a cosmetic procedure not covered by insurance, we offer the following options:
-
CareCredit: A healthcare credit card that allows you to pay for treatment in manageable monthly installments.
-
Flexible Self-Pay Plans: Transparent, flat-rate pricing for patients without insurance or those seeking non-medically necessary treatments.
We’re here to help make sure that you get the treatment you need, no matter your financial situation.
What Happens During Your Vein Treatment Appointment?
Knowing what to expect makes the decision to move forward much easier. Many patients assume vein treatment involves surgery, hospital beds, and weeks of recovery but modern vein care is nothing like that.
Today’s vein treatments are simple, minimally invasive, and performed entirely in our outpatient clinics—not hospitals. There is no general anesthesia, no hospital stay, and little to no downtime.
At USA Vein Clinics, your appointment is designed to be efficient, informative, and focused on your comfort.
Step 1: Check-In & Insurance Confirmation
When you arrive, our team confirms your insurance coverage and reviews any remaining eligibility details. We believe in full transparency—your benefits and expected out-of-pocket costs are discussed before any treatment begins.
Step 2: Diagnostic Duplex Ultrasound (The Proof)
If you haven’t had one recently, a Duplex Ultrasound is performed during your visit. This painless, in-office scan is the most important step because it:
-
Confirms Venous Reflux
Identifies exactly where blood is flowing backward. -
Secures Insurance Approval
Provides the objective medical evidence insurers require to prove medical necessity. -
Identifies the Root Cause
Ensures treatment addresses the source of your symptoms—not just surface veins.
This real-time imaging allows your specialist to make precise, evidence-based decisions.
Step 3: Personalized Treatment Plan Review
Your vein specialist will review your ultrasound results with you in plain language. They will explain why a specific treatment such as EVLT, RFA, or VenaSeal™ is recommended and what you can expect during recovery.
No treatment proceeds until you feel fully informed and confident.
Step 4: The In-Office Procedure
Most vein treatments take 30 to 60 minutes and are performed right in the clinic. Local anesthesia is used, so you remain awake and comfortable throughout the procedure.
Most patients describe the sensation as mild pressure not pain.
Step 5: Walk Out and Resume Your Day
This is often the biggest surprise for patients:
-
You walk out on your own
-
No stitches or large incisions
-
Most patients return to normal activities the same day
You’ll receive simple post-care instructions such as wearing compression stockings briefly to support healing and long-term results.
Why You Shouldn’t Delay Vein Treatment?
Vein disease is not static—it is progressive. While symptoms may start as mild discomfort or cosmetic changes, untreated vein conditions tend to worsen over time as pressure continues to build inside the veins.
Delaying treatment can lead to:
-
Worsening pain and swelling as venous reflux increases
-
Permanent skin damage such as thickening, discoloration, or inflammation
-
Venous ulcers that are slow to heal and prone to infection
-
Higher risk of blood clots, including Deep Vein Thrombosis (DVT)
-
More complex treatment plans requiring additional sessions or procedures
Early intervention is often simpler, faster, and more cost-effective. Patients who seek care sooner typically require fewer treatments, experience quicker symptom relief, and have an easier time meeting insurance approval criteria.
Just as important, insurance coverage is often easier to secure before complications develop. Waiting until symptoms become severe can introduce delays, denials, or additional medical requirements.
If your legs are already telling you something isn’t right, getting evaluated now can prevent years of discomfort—and unnecessary risk—later.
Get Started with USA Vein Clinics
If you’re experiencing leg pain, swelling, heaviness, or visible vein changes, the next step is a proper medical evaluation not guesswork.
At USA Vein Clinics, we make it easy to move forward with confidence:
-
Most major insurance plans accepted
-
Medicare & Medicaid welcome
-
In-office evaluation with Duplex Ultrasound
-
No obligation to proceed with treatment
Your evaluation will confirm whether treatment is medically necessary, verify your insurance coverage, and give you clear answers—before any decisions are made.
Schedule Your Vein Evaluation Today
Frequently Asked Questions
Do I Need a Referral to See a Vein Specialist?
You don’t generally need a referral to see the vein specialists at USA Vein Clinics. To make an appointment, call us today at 888.768.3467.
What are the common vein treatments that insurance covers?
Insurance often covers minimally invasive treatments such as Endovenous Laser Therapy (EVLT), Radiofrequency Ablation (RFA), sclerotherapy, ClariVein® Varithena, and VenaSeal™.