Venous insufficiency is one of the most common medical problems that affect adults in the United States. Every year, approximately 150,000 new patients are diagnosed with venous insufficiency. You may be more familiar with its visible results — varicose veins, spider veins, and leg ulcers. Poor circulation and its effects have been well-documented for centuries. And while you may not associate vein problems with antiquity, varicose veins and their effects have been present in humans, and our literature and art, since the days of Hippocrates.
If you’re like most people who are suffering from deep vein thrombosis (DVT), varicose veins, or other forms of vein disease, the history of vein treatment is interesting, but not necessarily reassuring. After all, these conditions can be painful. And, until recently, the treatments associated with them were often painful. But thanks to research and a lot of progress, today’s vein therapy treatments are highly effective, minimally invasive, and offer relatively quick relief from the pain and discomfort associated with venous insufficiency.
The history of vein therapy has been well-documented. At this point in the history of vein therapy, we know more about these conditions and how to treat them than ever before. And our patients are benefiting from centuries of research.
If you or someone you love is suffering from varicose veins or another occurrence of venous insufficiency, there’s never been a better time to look for help from experienced medical professionals.
What Is Vein Disease?
Vein disease, also referred to as venous insufficiency, is when the veins have trouble sending blood from the legs to the heart. The valves in your veins should keep blood flowing toward the heart. With long-term venous insufficiency, the vein walls become weak and valves are damaged. As a result, blood stays in the veins and leads to painful symptoms and skin changes.
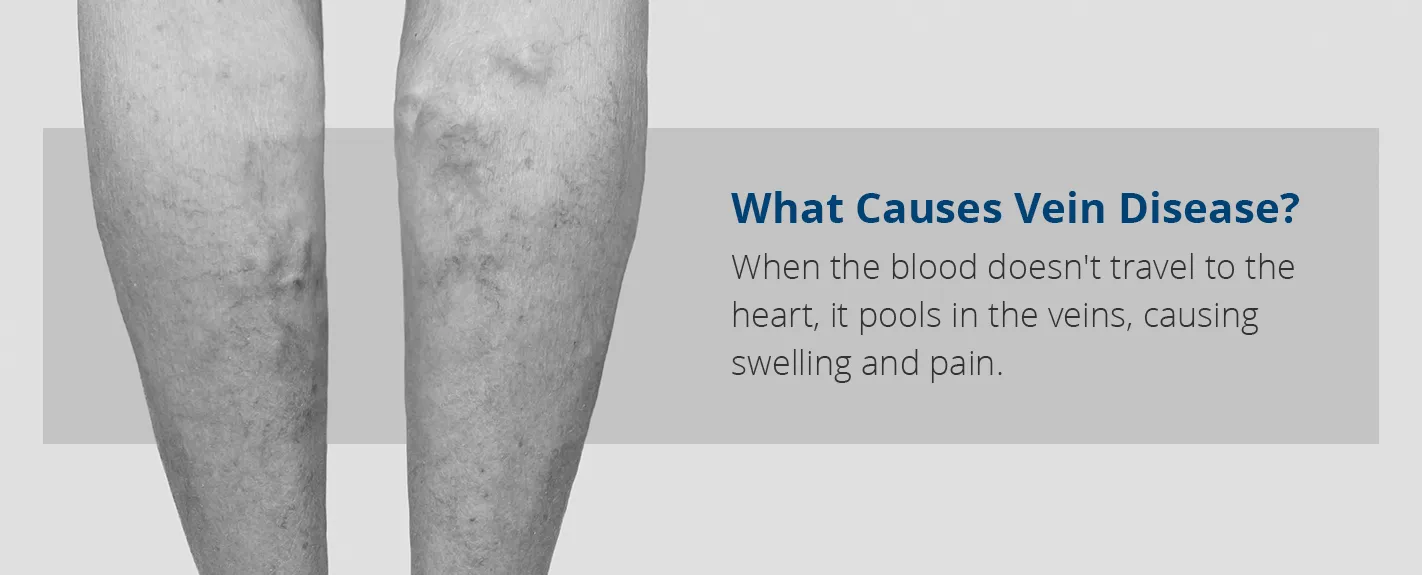
What Causes Vein Disease?
When blood doesn’t travel to the heart and pools in the veins, it causes swelling and pain. When this happens, it causes your other veins to work harder to compensate for the compromised vein, which can cause other veins to experience the same malfunction over time.
Although incredibly painful, this condition is not initially life-threatening. You might not even notice the problem for a long time. However, the most significant risk associated with vein disease is that minor issues can snowball into bigger ones. If left untreated, a small circulation issue can one day cause a significant — and potentially life-threatening — health problem.
Symptoms of Vein Disease
Symptoms of venous insufficiency may include:
- Pain or cramping in legs
- Difficulty standing
- Swollen legs
- Restless leg syndrome
- Skin discoloration
- Burning or itching
- Blood clots
Who’s at Risk for Vein Disease?
While anyone can certainly develop problems with their veins, typically those who are at a greater risk for vein disease include adults who are:
- Over 50
- Female
- Pregnant
- Obese
- Current or former smokers
- Sedentary lifestyle
- Sitting or standing for long periods
- Family medical history
In other words, at any age or stage of your life, you may be vulnerable to poor circulation and its effects. By choosing to live a healthy, balanced lifestyle, you can decrease your chances of developing this problem as you age. However, remember some people are at increased risk of developing vein disease because of genetics. Even if you are living a healthy, active life, it’s crucial to remain vigilant and pay attention to your body over time.
The History of Vein Treatment
Vein diseases, specifically varicose veins, have been recognized for thousands of years. For example, the Ebers papyrus of 1550 B.C. describes varicose veins as “serpent-shaped dilation of the lower limbs.” Here’s a brief history of vein therapy to show you how vein therapy has improved over thousands of years of discoveries and research:
- 400 B.C.: From 460 to 377 B.C., Hippocrates notes ways blood flow affects parts of the body. For example, he claims that standing up exaggerates leg ulcerations. Hippocrates also mentions in his writings treatment of varicose veins with a metal instrument.
- 15th century: From about 1485 to 1515, Leonardo da Vinci makes anatomical drawings based on his dissections. His drawings of veins help doctors understand how the venous system works.
- 1525: Ambroise Paré, a French surgeon, describes bandaging leg ulcers from the foot to the knee.
- 1585: Surgeon Fabrice d’Acquapendente explains vein valves. The valves in the veins keep blood from flowing backward.
- 1676: Richard Wiseman, an English surgeon, invents the first supportive stockings.
- 1860: Charles Pravaz invents a syringe and introduces sclerotherapy, which involves injecting a special mixture into the veins to cause the veins to disappear and be absorbed by the body.
- End of the 19th century: Friedrich Trendelenburg performs the first ligation of the greater saphenous vein. Ligation refers to the tying of veins to prevent pooling of blood.
- Early 20th century: During this time, the surgeons W.L. Keller, C.H. Mayo and W. Babcock establish the technique of vein stripping. In 1906, Alexis Carrel reports the first venous transplantation.
- 1938: Robert Linton is the first to suggest ligation of communicating veins as the primary form of therapy in treating vein disease.
- 1953: Sven Ivar Seldinger invents a method for venous access called the Seldinger technique.
- 1964: Charles Dotter performs the first percutaneous transluminal angioplasty with a catheter. Dotter’s contributions led to further use of catheters, stents and angioplasty to treat vascular disease.
- 1960s and 1970s: The late 60s and early 70s was known as the sonic boom because it was during this time that real-time ultrasound started to appear. A duplex ultrasound, for example, is a critical tool in vein disease treatment. A duplex ultrasound sees how blood moves through a patient’s veins.
- 1999 to the present: Various modern devices and systems, such as radiofrequency ablation, are approved by the Food and Drug Administration (FDA) to treat vein disease. Radiofrequency ablation involves heating up tissue to form scar tissue which then closes off a vein.
What Is Vein Therapy?
Vein therapy is an umbrella term that refers to a variety of surgical treatments and medical treatments designed to repair veins that are causing pain and other health problems. Vein therapy treats several manifestations of vein disease and vein-related issues including — but not limited to — DVT, leg ulcers, varicose veins, spider veins, lower leg edema, venous ulcers, poor circulation and May-Thurner syndrome.
Ancient art depicts a variety of painful leg conditions, as well as the invasive attempts made to relieve the pain. A Middle Ages manuscript from 1271 tells the story of a 20-year-old cobbler named Raoul who, as it turns out, was suffering from DVT. The document goes on to tell the story of his miraculous healing, thanks to the help of some sacred dust, which obviously isn’t a treatment we’d recommend today.
Even in more recent years, vein therapies have developed a reputation for being painful. We’ve encountered many patients who are terrified because they’ve heard older relatives recount their experience with outdated vein therapies.
If you need treatment, rest assured today’s vein therapy isn’t anything like doctors did in the past.
What Is Vein Stripping?
Vein stripping is a surgical procedure which involves removing varicose veins in the legs. During treatment, the surgeon will remove or tie off the superficial saphenous vein in the leg to help treat varicose veins. The procedure usually takes up to one and a half hours, and patients may receive either general anesthesia or spinal anesthesia. To access the vein, the surgeon will make two or three cuts into the leg near the different sections of the damaged vein. Using a plastic wire, the surgeon will pull the vein out and sew the cuts shut with stitches.
Why Is Vein Stripping Outdated?
Today, there are much less painful ways to treat varicose veins such as endovenous laser therapy (EVLT), which is minimally invasive. Patients no longer have to endure treatment that requires anesthesia. Nor do they have to leave the treatment room with large incisions that could take months to heal or could get infected. Today’s treatments are more effective, take less time, and are far less invasive.
How Has Vein Treatment Improved?
Treatment of varicose veins and spider veins has come a long way since the days of Hippocrates. The advancement in vein therapy is due in large part to the medical community’s constantly increasing knowledge of vein disease and its impact on the body. While many adults consider varicose veins a “rite of passage” into middle age, the truth is that they are a wake-up call. Even if they haven’t become painful yet, varicose veins and their tiny spider vein cousins are a sign that your blood vessels may be struggling to meet your body’s needs for optimal circulation.
We aren’t suggesting you should run to your emergency room in a panic if you see one small spider vein. These are indeed common in older adults and, in many cases, they don’t cause any problems. However, the history of vein therapy and its modern counterparts have taught us it’s better to pay attention to those early signs than to wake up and discover a severe problem later.
At USA Vein Clinics, we treat patients with venous insufficiency using the latest technology. We offer the following minimally invasive non-surgical treatments to reduce varicose veins:
- Endovenous Laser Treatment: EVLT has been used for over a decade and is considered the best treatment for venous insufficiency. With EVLT, your doctor will insert a thin laser fiber into the diseased vein using a real-time ultrasound for guidance. Then your doctor will use laser energy to heat and close the malfunctioning veins. Your surrounding healthy veins will immediately take over the blood flow as the treated vein is absorbed by the body. This type of treatment usually lasts 15 minutes, so it is much faster than vein stripping. Also, unlike vein stripping, which requires weeks or longer to recover, you can resume your regular activities after EVLT.
- Varithena® vein treatment: Our Varithena treatment involves using foam to treat issues with the great saphenous vein and the surrounding veins. With Varithena treatment, the doctor will inject Varithena foam into the vein, which will cause the vein to collapse. The blood will be directed to other healthy veins. Like EVLT, Varithena treatment is quicker than vein stripping and does not require anesthesia.
- Ultrasound-guided sclerotherapy: Ultrasound-guided sclerotherapy is a type of treatment that uses live ultrasound technology to treat varicose veins near the skin’s surface. It is a minimally invasive technique that closes malfunctioning varicose veins and allows them to be absorbed by the body. The doctor will use ultrasound technology to locate the diseased vein and inject medication into the vein. This type of treatment provides almost immediate relief of varicose vein symptoms.
Patients who choose one of our treatments can expect the following benefits:
- Convenience: In most cases, our varicose vein treatments take less than 15 minutes. You can go home immediately after treatment. Depending on your needs, you can schedule treatment into a regular workday if you wish.
- Low risk: Non-Surgical varicose vein treatment has a high success rate and a high chance of a successful recovery.
- Fast: Your recovery is fast after our treatments. Some patients choose to go right back to work after treatment. You can continue light daily activities and drive yourself home after treatment, so there’s no need to ask someone for a ride.
- Latest technology: At USA Vein Clinics, we proudly offer the latest technology in the most advanced facilitates to provide our patients with the highest level of care possible. We strive to make our patients comfortable and cared for every step of the way, and we aim to make treatment a stress-free experience as part of a personalized care plan.
Reasons to Seek Vein Treatments
Here are some problems relating to vein disease and treatment options. If you have any questions or concerns about vein treatment and the best treatment for you, reach out to us, and we’ll be happy to assist you however we can.
1. Varicose Veins and Spider Veins
When we start talking about vein disease and treatment, one of the most common conditions people think of is varicose veins and spider veins. The terms are familiar, but what exactly are they?
Varicose veins are swollen blood vessels — usually in the legs — that are often prominently noticeable as they twist and turn in the legs. Spider veins are smaller blood vessels that, like their varicose counterparts, twist and turn, creating unsightly red and blue lines that are visible through the skin, typically in the legs or face.
So what causes varicose veins and spider veins?
There are a variety of factors that may predispose an individual to develop varicose veins, including genetics, age, hormones, gender and medical history. Often, when they first appear, people view them as a cosmetic inconvenience and, since they usually occur with age, many people consider them a sign of aging. While there may be some truth to this — varicose veins typically form as a person’s blood vessels become damaged or weakened over time — several other factors besides age can lead to these problems.
Besides their visual appearance, varicose and spider veins can become painful. Other symptoms of these conditions include:
- Restlessness
- Throbbing
- Burning
- Fatigue
- Tingling or heavy feeling in the legs
Ulcers and swelling are rare but can develop over time if you experience these symptoms but don’t seek treatment from a doctor.
In many cases, you can find relief for your varicose and spider veins by elevating your legs to relieve pressure. But sometimes, that’s not enough. The good news is, you can receive EVLT treatment or ultrasound-guided sclerotherapy to quickly treat painful varicose veins.In some cases, if your varicose and spider veins are related to the great saphenous vein, your doctor may prescribe Varithena vein treatment. Either way, your doctor will determine the best treatment for you.
2. Poor Circulation and Venous Insufficiency
Poor circulation doesn’t require much explanation because it’s exactly what it sounds like: the body’s inability to circulate blood throughout the body the way it should. In many cases, this may happen because of venous insufficiency, or what happens when a person’s veins are unable to circulate blood throughout the body the way they should. This issue can lead to muscle cramping, the buildup of fluid in the legs and feet, numbness, leg ulcers and varicose veins.
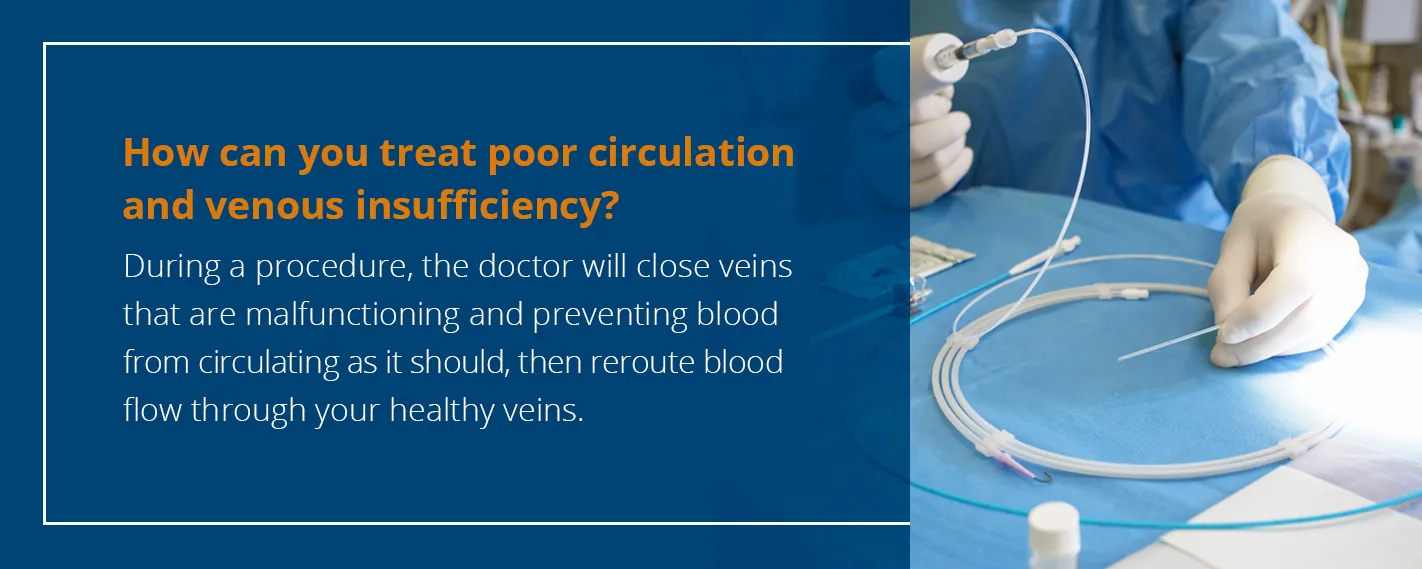
So how can you treat this problem?
While you can take care of minor cases of poor circulation at home, especially if your poor circulation relates to other health issues, individuals suffering from poor circulation due to venous insufficiency often require surgical treatment. During treatment, the doctor will close veins that are malfunctioning and preventing blood from circulating as it should, then reroute blood flow through your healthy veins.
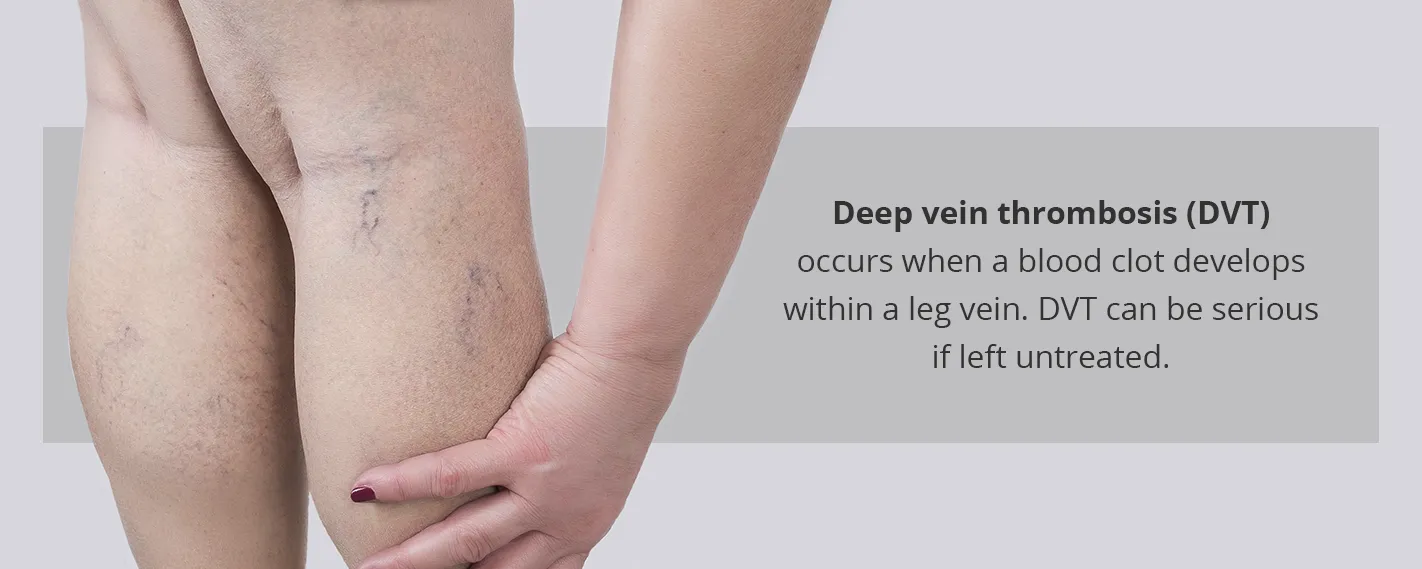
3. Deep Vein Thrombosis
Deep vein thrombosis occurs when blood clots inside a vein, often in the leg. When blood clumps together in this way, it can become extremely painful. Besides being painful, clots formed from DVT can break free and travel through the veins to the lungs, causing a pulmonary embolism (PE), which can be fatal if doctors don’t diagnose it in time.
Although DVT doesn’t receive mentions in ancient medical literature like venous ulcers, DVT and its treatment have been well-documented throughout history. Up until the 1930s, DVT treatments included various combinations of bed rest, elevation and warm compresses. Doctors knew DVT could lead to PE, so their goal, even then, was to reduce the size of the clot and prevent it from traveling to the lungs. Despite their more rudimentary treatments, including the use of leeches for bloodletting, they made great progress in identifying the tendency for DVT to show up after a woman gave birth or during other surgical treatments where infection could occur or a patient was on bed rest for long periods.
In more recent years, the medical field has spent a lot of its time and energy refining the DVT diagnosis process, which is one example of how vein therapy has improved. With DVT, time is of the essence. The sooner doctors discover the clot, the quicker they can break it up or remove it, preventing the patient from PE.
DVT and varicose veins are not the same. However, many of their symptoms are similar. Because of this, doctors will often use an ultrasound to diagnose DVT. While pain and discomfort are significant symptoms of DVT, they don’t always tell the whole story. And the best way to prevent this condition from happening in the first place is to make sure your veins are healthy. If you are having pain or discomfort in your leg or you suffer from varicose veins, it’s crucial to seek medical care and treatment.
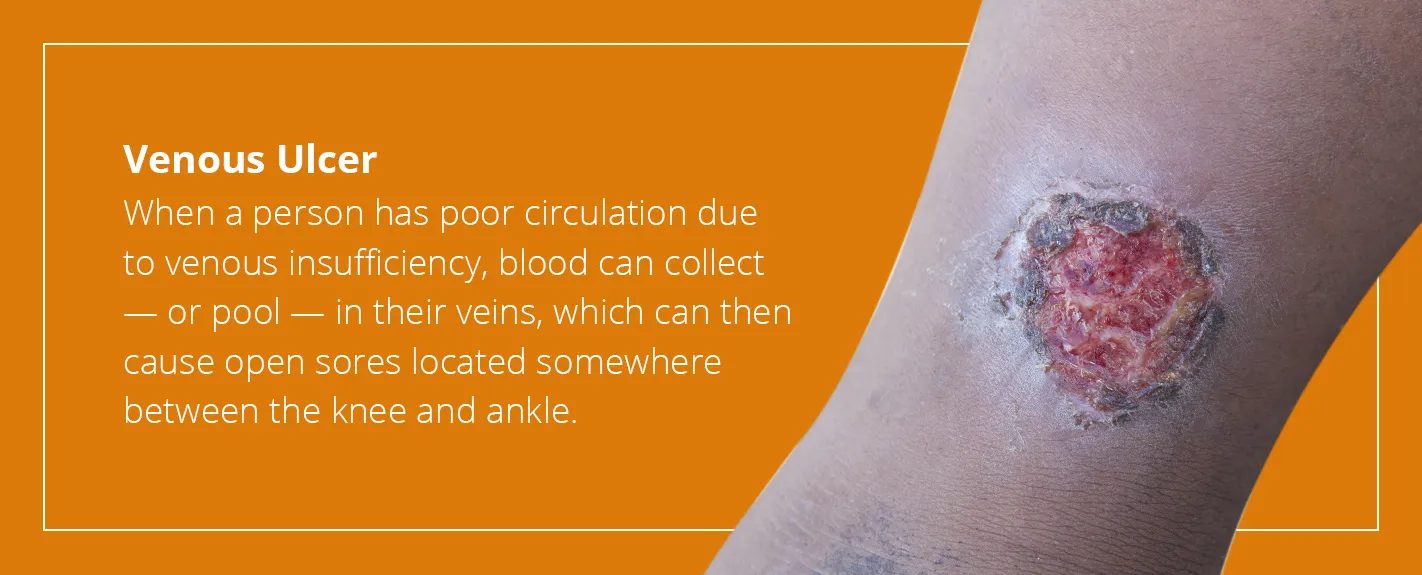
4. Venous Ulcer
Venous ulcers typically develop when venous insufficiency and poor circulation are present. Venous insufficiency is responsible for as many as 80% of all diagnosed leg ulcers. When a person has poor circulation due to venous insufficiency, blood can collect — or pool — in their veins, which can then cause open sores located somewhere between the knee and ankle.
In most cases, ulcers begin as a “rash” that won’t go away. Over time, the rash develops into an open wound that can be swollen, painful and even emits discharge. If left untreated, the ulcer can become infected and cause more severe health complications.
To heal ulcers and prevent them from reoccurring, patients must address their cause: venous insufficiency. Their ulcers will only go away permanently when they seek treatment for venous insufficiency. One of the essential things to note about venous ulcers is that they often happen because people ignore the initial symptoms, such as pain and a rash. If you have ongoing pain in your legs or a rash that appears without explanation and remains over time, consult with your doctor to determine its source.
5. May-Thurner Syndrome
May-Thurner syndrome is when the right iliac artery compresses its counterpart on the left side of the body at the point where they cross each other in the pelvic region. When the left iliac artery gets compressed, blood flow becomes compromised and swelling can occur. Unfortunately, May-Thurner syndrome isn’t something people know they have until they experience the effects of it.
May-Thurner syndrome is known to cause DVT in the left leg, because of the compression of the left iliac artery. Most people discover they have this after they have received a diagnosis of DVT.
However, some people are at higher risk of May-Thurner syndrome than others. These risk factors include:
- Being female
- Recently giving birth
- Giving birth to more than one child
- Having scoliosis
- Taking oral contraceptives
- Dehydration
- Having other health issues that increase the risk of excessive clotting
Medical professionals use imaging tests to determine if May-Thurner syndrome is present. When doctors discover a person who has May-Thurner syndrome, they can perform a minimally invasive treatment to open the left iliac artery and prevent clots in the future. The doctor inflates the left iliac artery and then inserts a stent to keep it open so blood can flow through properly.
How Can I Manage Leg Pain?
There are ways you can decrease the discomfort of varicose veins at home besides lying around with your legs elevated. These temporary, pain management treatments include the following.
1. Change Positions Frequently
Don’t sit or stand for long periods. If you work at a desk, take regular breaks to stand, walk or even do a few stretches. If you have a job that keeps you on your feet for hours at a time, make sure you take breaks to sit or stretch as well.
2. Watch Your Weight
A low-salt diet can prevent your body from retaining water and increasing swelling and pressure on your legs. And, losing a few pounds can also take some of the pressure off your legs as well. Eat healthy foods that will provide proper nutrition to your body. If this isn’t something you’ve done in the past, talk to your doctor about how to safely and effectively lose weight.
3. Choose Your Wardrobe Carefully
Avoid wearing tight-fitting clothes or high-heeled shoes. Believe it or not, tight clothing can restrict blood flow in certain areas of the body. If you already suffer from poor circulation, the last thing you want to do is make it worse by what you wear. Flat shoes work your calf muscles more, which can also improve the health of the veins in your legs. And they’re so much more comfortable anyway!
4. Exercise
Incorporating a walk into your daily routine can have a positive impact on your veins. It’s helpful if you’re trying to lose weight, but it’s also good for your circulation. If you want to do more than walk, check with your doctor before beginning an exercise routine, especially if you have other health conditions that increased physical activity might affect.
Find Relief at USA Vein Clinics
While pain management is effective in some cases, it’s essential to talk to a doctor before implementing a regimen of self-care. Why? A doctor who specializes in the treatment of vein diseases will be able to guide you to figure out what the problem is and the best way to treat it. In many cases, varicose veins are a sign of a much more severe problem that requires medical intervention.
At USA Vein Clinics, the largest network of vein treatment centers in the U.S., our patients receive minimally invasive treatments to treat vein disease and the symptoms that accompany it. Our vascular specialists dedicate their careers to providing one-on-one attention and care designed to address your individual health needs. Thanks to their years of experience, they can provide educated and effective treatment plans for many different situations.
Besides our large network of experienced medical professionals, our patients also receive support from an experienced and dedicated staff who are committed to providing personal care. We love helping people get healthy and start feeling good again. It’s why we do what we do!
If you’re ready for relief from the pain of vein disease, we’ve made it easy to book your appointment. You can use our online scheduler to make an appointment or feel free to call us at 888-768-3467.