Topics Covered in this Blog:
- Athletes and Blood Clots
- What Are the Symptoms of DVT and PE?
- Athletes and Varicose Veins
- Athletes with Varicose Veins
- Am I at Risk for Vein Problems if I’m Not an Athlete?
- Schedule an Initial Consultation
When you think of an athlete, you probably imagine a young, fit, healthy individual — not someone who has to worry about developing a sudden health condition. Yet, even the most accomplished athletes are at risk of developing blood clots.
A 2017 study reviewed the injury reports from four professional sports leagues to determine how many athletes had experienced deep vein thrombosis (DVT) or pulmonary embolism (PE)[1]. DVT occurs when a blood clot forms in a vein deep within the body. A pulmonary embolism is a life-threatening emergency that occurs if the clot breaks loose and travels to the lungs.
The study found DVT and/or PE affected the athletes 55 times over the course of the study. Some athletes had both conditions. While the athletes’ ages ranged from 19 to 42, the average age at the time of the DVT or PE was 29 years old. The average time away from play after diagnosis was six months, but some athletes saw their careers end after experiencing a blood clot.
Why do athletes get blood clots? Below, we discuss athletes, blood clots, and athletes with varicose veins and other venous conditions. If you are concerned about your vein health, we recommend consulting a vein specialist for personalized recommendations.
Athletes and Blood Clots
What causes blood clots in athletes? There are many risk factors for blood clots, including age, genetics, and lifestyle. Athletes are subject to the same risk factors as other people, along with being more likely to have experienced recent surgery, broken bones, or other injuries. All of these things make blood clots more likely to occur.
DVT risk factors include:
- Being over the age of 40
- Recent surgery or broken bone
- Recent illness or injury that leaves you bedridden
- Extended travel (common during sports season for pro athletes)
- Underlying health conditions, such as diabetes or high blood pressure
- Pregnancy
- Smoking
- Being overweight or obese
- Having varicose veins
- Personal or family history of DVT
- Varicose veins and spider veins
In the same study previously mentioned, about 40% of the athletes who experienced blood clots had risk factors, including:
- Family history of a clotting disorder
- Known clotting disorder
- An injury or trauma
- Recent surgery
- A previous blood clot
If you are an athlete at high risk of developing DVT, close monitoring by a vein specialist may be beneficial.
What Are the Symptoms of DVT and PE?
Whether or not you have known risk factors for deep vein thrombosis and pulmonary embolism, the ability to identify their symptoms is key to obtaining timely treatment. Earlier treatment generally leads to the best health outcomes.
Common DVT symptoms include:
- Swelling in a limb (usually your leg, but may be an arm, depending on your sport)
- Pain or tenderness in your limb, which may feel like a cramp
- Skin discoloration
- Warm feeling in your limb
If you experience DVT symptoms, seek medical evaluation as soon as possible.
Symptoms of pulmonary embolism include:
- Sudden shortness of breath
- Sudden rapid heart rate
- Pain in your chest that is sharp and may worsen with deep breaths
- Passing out
- Sudden cough, sometimes accompanied by bloody mucus
If you experience PE symptoms, call 911 or head directly to the nearest emergency room.
In addition to being on the lookout for these symptoms, there are some measures that athletes and active individuals can take to reduce their risks of developing DVT and PE. These include:
- Move around and stretch frequently, especially when traveling long distances
- Drink plenty of water to stay hydrated before, during, and after travel and sporting events
- Know your risk factors for blood clots, including whether you have a family history of them
- Pay attention to unusual symptoms and seek medical care as advised above
These simple tips can help prevent blood clots in athletes and anyone else.
Athletes and Varicose Veins
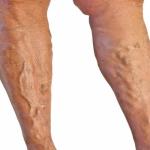
Do athletes get varicose veins? Many athletes develop varicose veins at some point in their lifetime, along with the painful and uncomfortable symptoms that often accompany them. Not only can varicose veins cause leg swelling, cramping, and other issues, their presence can raise the risk of blood clots in both athletes and non-athletes.
Common varicose vein symptoms include:
- Swelling: Along with the visible veins, swollen legs, ankles, and feet are common signs of vein disease. Some patients observe that their shoes feel tighter, while others report pain or discomfort in swollen areas. If you notice unexplained swelling in your lower extremities near varicose veins, we recommend seeking medical evaluation.
- Cramping: Leg cramps are another common effect of venous insufficiency. You may suffer from cramps at night that impact sleep, or you notice daytime cramping in your calves, thighs, or buttocks. Since there are many possible explanations for leg cramps, it is important to visit your doctor to diagnose the underlying cause.
- Heaviness: If you have enlarged, visible veins and your legs seem unusually heavy, you may want to visit an experienced vein specialist. People with varicose veins sometimes feel like they carry weights around their ankles.
- Numbness: Another potential varicose vein symptom is numbness in the legs and feet. This may occur when blood circulation slows due to venous insufficiency.
- Itching and burning: Skin changes near varicose veins can indicate advancing vein disease. Although you may be tempted to use regular lotions and creams, they probably won’t be effective. Treating underlying vein disease can bring relief to this type of discomfort.
- Pain relief when legs are elevated: If you have leg pain that is alleviated by propping your feet and legs up, this may be an early-stage varicose vein symptom.
Minimally invasive, office-based treatment is widely available and should be considered for varicose veins in athletes and other individuals. Vein treatment can alleviate painful venous symptoms, reduce the risk of deep vein thrombosis and pulmonary embolism, and improve quality of life. You may even find that your athletic performance improves after treatment.
Athletes with Varicose Veins
Believe it or not, even the world’s best athletes can get varicose veins and experience the painful symptoms and challenges varicose veins present. Summer Sanders, Olympic gold medalist in swimming, sports commentator, reporter, TV show host and actress, shared her story as the spokesperson of a campaign called “Rethink Varicose Veins.” This campaign is designed to educate the public about this common, yet serious condition and dispel misconceptions. Read Summer’s story below.
“My own mother suffered from varicose veins most of her life,” says Summer. “She was often on her feet due to her work as a flight attendant and would find herself in pain during long trips. She began to notice her varicose veins when she was pregnant with me and always joked that varicose veins are hereditary; according to my mom, you get them from your kids!
It soon hit me that, even though I was active, I was starting to get my mother’s legs. Like many moms, my lifestyle requires me to be on my feet constantly. I noticed my legs were heavy and achy after a long day, but I assumed these symptoms were just something I had to deal with.
My doctor and I decided the best path for me was a minimally invasive treatment. The procedure was quick and I was back to my regular activities within a short period of time. Now my legs feel awesome again. Varicose veins are not just a cosmetic issue; you don’t have to live with them anymore.”
Similar to Summer, many other athletes experience the challenging effects of athlete varicose veins and their symptoms. Since minimally invasive, office-based vein treatment involves little downtime, it can quickly help athletes return to their preferred activities.
Am I at Risk for Vein Problems if I’m Not an Athlete?
Although we have mostly discussed athletes and blood clots, as well as athletes with varicose veins, you should know that anyone who is physically active (or sedentary) can also be at risk. While you may be surprised to notice bulging varicose veins on your legs if you are young and work out regularly, the reality is that anyone of any age and activity level can develop venous issues.
On the other hand, regular activity can help improve circulation and promote healthy blood flow. To avoid venous issues, most experts recommend aiming for at least 30 minutes of physical activity each day, five days a week. Additionally, avoid prolonged standing or sitting and move around frequently throughout the day.
You can also improve your vein health by:
- Maintaining a healthy body mass index (BMI)
- Eating a well-rounded diet
- Quitting smoking
- Managing other underlying health issues
- Wearing compression socks as prescribed
Schedule an Initial Consultation at USA Vein Clinics
Although athletes and blood clots can go hand-in-hand, there is plenty of help available. At USA Vein Clinics, our vein specialists provide a range of minimally invasive, office-based vein treatments for varicose veins, spider veins, and other venous issues.
While our vein specialists do not offer treatment for deep vein thrombosis or pulmonary embolism, we do treat several venous conditions that can place you at risk for developing these dangerous health conditions.
For an initial consultation, schedule an appointment online today. We offer over 100 clinic locations nationwide and convenient virtual doctor visits. Vein treatment is covered by most health insurance plans, including Medicare and Medicaid. To discuss your plan’s coverage details, just give us a call at 888.768.3467.
[1] Meghan Bishop et al., “Venous Thromboembolism within Professional American Sport Leagues,” Orthopaedic journal of sports medicine (SAGE Publications, December 19, 2017), https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5753956/.