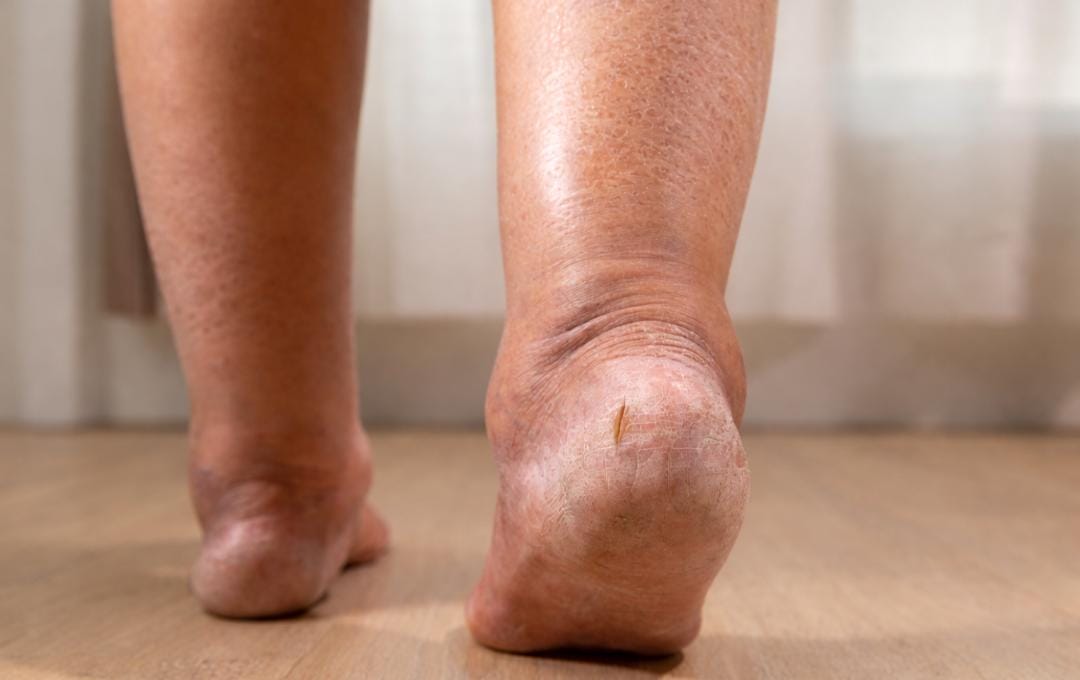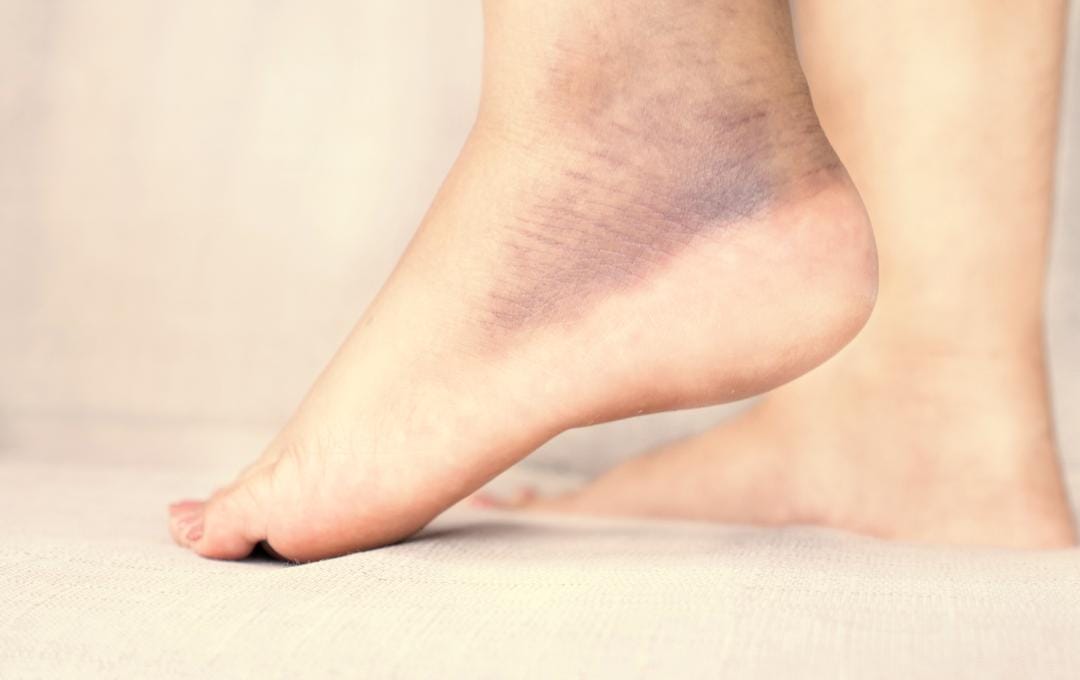
Are you noticing golden or rusty-brown spotting on your feet or lower legs that isn’t going away? This skin change may be caused by hemosiderin staining.
Hemosiderin staining occurs when iron from red blood cells deposits in the skin, causing the skin to darken. While the discoloration isn’t painful, it often indicates a progressive, underlying condition that impairs blood circulation. This condition, known as vein disease, can lead to other skin changes that can significantly impact overall health if untreated.
Understanding what causes hemosiderin staining and recognizing its symptoms can help people take proactive steps to prevent these complications.
What is Hemosiderin Staining?
Hemosiderin staining happens when iron-rich proteins called hemoglobin accumulate underneath the skin. Hemoglobin comes from red blood cells and helps carry oxygen throughout the body. When red blood cells break down, hemoglobin is released and deposited into the skin.
Hemosiderin staining often results from chronic venous insufficiency (CVI), where blood pools in the legs due to weak or damaged veins. The pooling adds pressure to the veins, making blood and hemoglobin more likely to “leak” into the surrounding tissues. It can also cause the veins to expand and twist in the form of varicose or spider veins.
What Does Hemosiderin Staining Look Like?
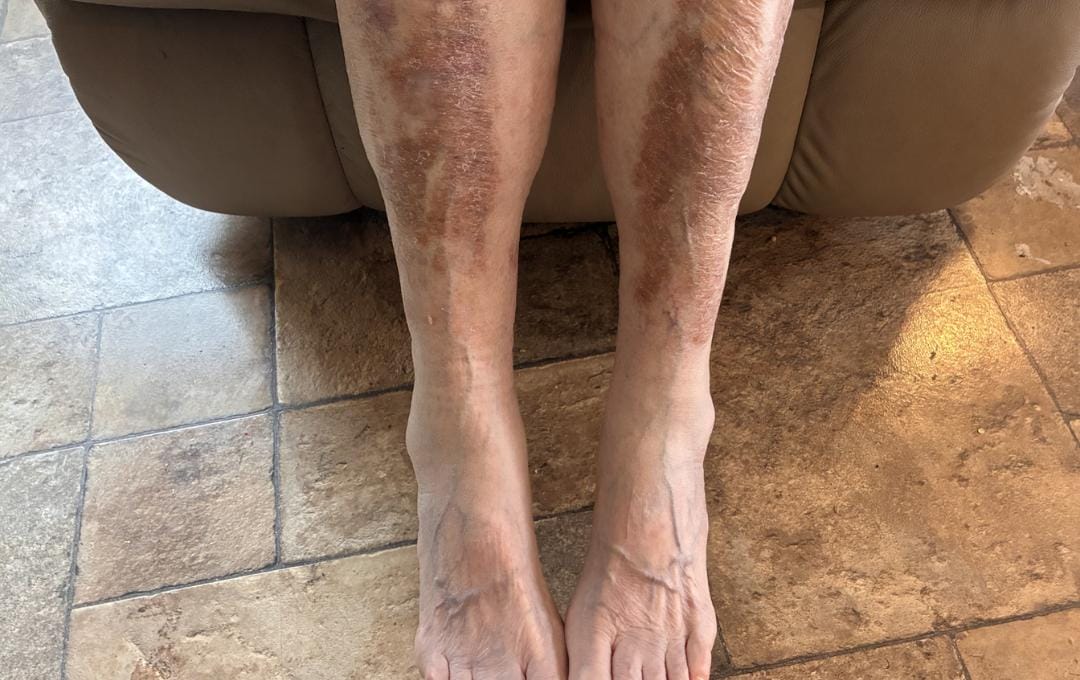
Hemosiderin staining looks like hyperpigmentation on the skin, typically around the lower legs and ankles. It may resemble a bruise on darker skin tones. The skin may also appear dry or hardened and may feel itchy, which can indicate underlying vein disease.
What Are the Symptoms of Hemosiderin Staining?
While no two individuals experience hemosiderin staining symptoms the same way, here are some common signs to look out for:
Skin Discoloration
Brown or yellow spots may appear on the legs, particularly the lower legs and ankles. Staining may also look like a permanent bruise discoloration. The visibility of this discoloration can vary based on skin tone.
Skin Hardening
Iron-rich deposits from broken-down red blood cells may also harden the surrounding skin, causing it to feel firm or leathery.
Itchiness or Skin Irritation
The buildup of hemosiderin can trigger an inflammatory response, leading to dry, itchy, or irritated skin. The compromised circulation and skin barrier can also make the area more sensitive.
Swelling
Swelling in the lower legs may be a common symptom alongside hemosiderin staining. However, swelling is primarily due to chronic venous insufficiency (CVI), where poor blood flow causes fluid to accumulate in the legs.
Early Hemosiderin Staining Signs to Watch For
Hemosiderin staining is commonly associated with advanced venous disease, which can increase the risk of blood clots or non-healing wounds. Recognizing the early signs of vein disease can help guide patients to the best treatments to alleviate or prevent the condition from worsening. These early signs include:
- Leg pain, cramping, or aching
- Swelling
- Fatigued or “heavy” legs
- Restlessness, especially at night
- Varicose or spider veins
If you have these symptoms and are unsure if it’s caused by vein disease, USA Vein Clinics has an online symptom quiz to help determine whether you need to see a vein specialist.
Causes of Hemosiderin Staining on the Legs
The primary cause of hemosiderin staining on the legs is vein disease, but it can be a result of other conditions or circumstances. Common causes include:
Chronic Venous Insufficiency (CVI)
In healthy veins, one-way valves help push blood upward toward the heart. Chronic venous insufficiency (CVI), or vein disease, occurs when these valves no longer function, causing the blood to pool in the legs. Blood pooling can also leak into the skin, leaving a hyperpigmented patch.
Varicose Veins
Varicose veins are a symptom of chronic venous insufficiency. These veins can look twisted and bulge from underneath the skin. In addition to their appearance, varicose veins can cause leg pain, swelling, and skin changes like hemosiderin staining.
Deep Vein Thrombosis (DVT)
Deep vein thrombosis (DVT) is a blood clot that forms in veins deep inside the legs, obstructing normal blood flow and increasing pressure on the area. This slowed traffic causes blood to flow out of the vein and into the surrounding tissue, resulting in hemosiderin staining. If untreated, DVT can become life-threatening if the clot breaks loose and travels to the lungs.
Medications
Blood thinners (anticoagulants) and antiplatelet drugs (like aspirin) don’t directly cause the stain, but they make it much easier for blood to leak out of the capillaries into the skin tissue. If a patient has even minor pressure or “leaky” vessels, blood thinners prevent the blood from clotting quickly, allowing more red blood cells to escape. Certain calcium channel blockers (used for high blood pressure) can cause leg swelling (edema), which increases pressure on the capillaries and leads to leakage.
Chronic Edema (Swelling)
Persistent swelling from causes other than vein disease—such as lymphedema, heart failure, or kidney disease—puts immense pressure on the small blood vessels in the legs. Over time, this pressure “pushes” red blood cells through the vessel walls.
Stasis Dermatitis
This is an inflammatory skin condition that often happens alongside vein issues. The inflammation itself damages the small capillaries, making them more prone to “micro-hemorrhages” that leave iron behind.
Leg Trauma
A recent or chronic injury, such as an ankle sprain, bruising, or a bone break, can damage the surrounding blood vessels and lead to skin discoloration.
Is Hemosiderin Staining Dangerous?
While hemosiderin staining itself is not dangerous, if underlying vein disease is what caused the hyperpigmentation, it can lead to serious complications if left untreated, including:
- Venous ulcers: Open sores on the legs that are slow to heal or may not heal at all. Venous ulcers typically occur in advanced vein disease and are more prone to infections if untreated.
- Cellulitis: Bacterial infection of the skin and surrounding tissue. If untreated, cellulitis may progress to osteomyelitis, a bone infection usually found in the lower legs and ankles.
- Stasis Dermatitis: Also known as “varicose eczema,” stasis dermatitis happens because of poor circulation and causes skin inflammation that leads to dry, itchy, and flaky skin near the affected veins. It is a clinical indication of CVI.
Hemosiderin Staining Treatment Options
If you have persistent skin discoloration, the best action to take is to discuss hemosiderin staining with a vein specialist. Because hemosiderin staining is a physical symptom of internal vein pressure, topical creams alone cannot resolve the discoloration. A vein specialist can determine if vein disease is causing the hyperpigmentation and recommend minimally invasive treatment options to prevent the progression of the staining. Early detection and treatment can help reduce the risk of developing more serious complications like stasis dermatitis or venous ulcers.
USA Vein Clinics can personalize treatments for each patient’s condition. Vein specialists will use advanced imaging techniques, such as a duplex ultrasound, to guide a specialized catheter to the affected vein and close it. As a result, hemosiderin staining will fade and any leg pain, swelling, or fatigue will subside. Since these procedures are minimally invasive, there are minimal risks and side effects. They are also performed in office-based settings, allowing patients to return home the same day as their treatment.
When to See an Expert Vein Specialist
You don’t need to experience leg pain or swelling to benefit from a vein evaluation. Evaluation becomes especially important if there are signs that the underlying vein disease is progressing. These signs include skin that:
- Continues to darken
- Spreads across the lower legs
- Causes itching or irritation
- Firms or hardens
Vein disease becomes easier to manage and treat when it’s detected early. Early treatment can stop the disease from progressing, allowing patients to take control of their vein health before complications occur.
Find Effective Relief at USA Vein Clinics
USA Vein Clinics focuses exclusively on diagnosing and treating vein disease to address symptoms like hemosiderin staining. Our team of vein specialists are experienced in advanced imaging to accurately diagnose vein disease and recommend the best treatment to restore healthy circulation.
Care is provided in a comfortable outpatient setting designed for vein treatment. This approach allows a more streamlined experience, allowing patients to return home the same day as their treatment.
To make the process easier for patients, our team verifies insurance coverage when appointments are scheduled and helps guide patients through the next steps of care. With over 160 locations nationwide, accessing specialized vein treatment is both convenient and straightforward.
To get started, enter your zip code below to find a vein clinic near you.
FAQs
How long does hemosiderin staining last?
Hemosiderin staining can linger for months or even years as the pigment gradually accumulates in the skin. However, treating its underlying cause can help discoloration fade over time.
What does hemosiderin deposition mean?
Hemosiderin deposition is the same as hemosiderin staining. It occurs when iron-rich protein in the blood seeps into the skin and leaves a brown, rust-like pigment on the surface. It is more commonly associated with chronic venous insufficiency (CVI) or vein disease.
What diseases cause hemosiderin staining?
Vein disease is the primary cause of hemosiderin staining, which includes specific conditions such as chronic venous insufficiency (CVI), deep vein thrombosis (DVT), or varicose veins.
How do you get rid of hemosiderin staining?
Minimally invasive treatments can significantly reduce hemosiderin staining. It can also alleviate accompanying symptoms, such as leg pain, swelling, and visible varicose or spider veins.
Medically Reviewed By:
Dr. Yan Katsnelson is a philanthropist, business owner, and highly skilled cardiac surgeon. He is the Founder and CEO of USA Vein Clinics, which is part of USA Clinics Group, the parent company of USA Fibroid Centers, USA Vascular Centers, and USA Oncology Centers, with more than 100 facilities nationwide. Dr. Yan has established himself as a strong advocate for accessibility and affordability of the most advanced medical care close to home. His mission is to create a positive experience for each patient with compassionate, personalized, and expert care.