Noticing that your veins look more visible than usual can be unsettling, especially if it seems to happen suddenly or is accompanied by new symptoms. In many cases, visible veins are simply related to natural factors like age, skin tone, hydration levels, or exercise. However, increasingly prominent or bulging veins can also be an early sign of vein disease. Understanding the difference between harmless and medically concerning causes can help you decide when it’s time to speak with a vein specialist.
Book Your Ultrasound and Consultation
Why Veins Become More Visible: Harmless Causes
Several everyday factors can make veins stand out without indicating any underlying medical issue. People with naturally lighter or thinner skin tend to see their veins more easily, and this visibility increases with age as collagen decreases and skin becomes more translucent. Heat exposure such as during warm weather or hot showers also causes veins to dilate, bringing them closer to the skin’s surface.
Exercise and weightlifting increase blood flow and temporarily enlarge the veins, particularly in individuals with lower body fat. Dehydration can make veins appear more raised due to increased blood concentration. Hormonal changes during pregnancy, menopause, or due to hormonal medications may also increase vein visibility. Both weight gain and rapid weight loss can change how close veins appear to the skin.
Veins may also look more visible when swelling is present and circulation changes can similarly make veins appear darker or more raised, a pattern seen in individuals with reduced leg circulation.
When Visible Veins May Indicate Vein Disease
The most common medical cause of increasingly visible or bulging veins is chronic venous insufficiency (CVI), a condition where the valves inside the leg veins weaken and allow blood to flow backward, or reflux. When this happens, blood pools in the lower legs, increasing vein pressure and causing veins to enlarge, darken, twist, or bulge.
Individuals experiencing visible veins alongside symptoms such as heaviness, swelling, itching, throbbing, or nighttime leg discomfort may be experiencing early signs of CVI. Many of the earliest signs are subtle, which is why recognizing vein disease symptoms.
Take Our Easy Symptoms Quiz Now
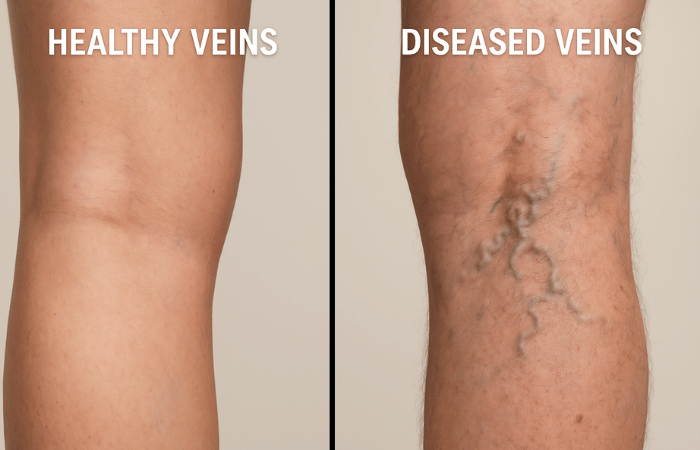
Healthy Veins vs Diseased Veins: How to Tell the Difference
Healthy veins typically lie flat beneath the skin and do not cause discomfort. Veins affected by vein disease often appear bulging or twisted due to weakened valves that disrupt normal blood flow.
Visible Veins: Warning Signs That Need Medical Attention
Key Warning Signs Discussed by Dr. White
In the video below, our board-certified vein expert, Dr. Jacob White, delves into the specific red flags that should never be ignored. He covers how to identify symptoms such as:
- Persistent Aching or Heaviness: A constant discomfort in the legs, especially after long periods of standing or sitting.
- Swelling (Edema): Noticeable puffiness in the ankles and lower legs that may worsen throughout the day.
- Skin Changes: Discoloration, dry, itchy skin (venous eczema), or the development of non-healing sores (venous ulcers).
- Bleeding: If a varicose vein is bumped and begins to bleed excessively.
Learn more about the warning signs of visible veins, when to seek a consultation, and the latest treatment options from Dr. Jacob White:
Healthy Veins vs. Vein Disease Symptoms
If you worry about why your veins are suddenly so visible, it’s important to pay attention to other symptoms you may be feeling. If CVI is causing your veins to be more prominent, here are signs you should look out for:
- Veins bulging underneath the skin
- Aching
- Throbbing
- Swelling in the legs, feet, or ankles
- A burning sensation
- Skin changes like discoloration, dryness, itchiness, or thickened skin
- Nighttime cramping
- Leg heaviness or fatigue
- Restless legs
If your veins are visible and accompanied by discomfort, or if they are becoming more visible over time, it may be a sign of chronic venous insufficiency.
Why Veins Sometimes Become Suddenly Visible
Some people notice that their veins appear more visible “overnight.” While true overnight changes are rare, visibility can increase quickly due to:
- Long periods of sitting, standing, or travel
- Heat exposure
- Rapid weight loss
- Pregnancy or postpartum changes
- Hormonal fluctuations
- Dehydration
- Valve weakening after a past minor clot
Sudden changes combined with warmth, redness, or swelling require prompt evaluation.
How Vein Specialists Diagnose the Cause of Visible Veins
At USA Vein Clinics, diagnosis begins with a comprehensive duplex ultrasound exam, which evaluates vein valve function and blood flow. Specialists also perform valve reflux testing to determine whether blood is flowing backward through the legs. Vein disease severity is often categorized using the CEAP classification system, which helps guide treatment planning.
Visible veins can also occur in people who delay treatment for varicose veins, and early evaluation can prevent complications.
Concerned About Visible Veins? Schedule a Consultation
Minimally Invasive Treatment Options at USA Vein Clinics
When visible veins are caused by vein disease, minimally invasive treatments can help restore circulation and reduce symptoms. Office-based, non-surgical procedures include:
- Endovenous Laser Therapy (EVLT)
- Radiofrequency Ablation (RFA)
- Varithena™ Foam Treatment
- Ultrasound-Guided Sclerotherapy
- Visual Sclerotherapy
- ClariVein® Mechanical & Chemical Ablation
- VenaSeal™ Vein Closure System
Most patients resume normal activities the same day. Individuals often ask about recovery expectations after a procedure, which are outlined in our vein treatment recovery guide.
Why Choose America’s Leading Vein Specialists
USA Vein Clinics offers comprehensive, accessible, and evidence-based care delivered by board-certified specialists across more than 168 outpatient locations. Patients benefit from personalized treatment plans, minimally invasive procedures, and insurance-covered care. Read What Our Patients Say
If your veins suddenly become very visible and you are unsure if it’s a sign of vein disease, call us at 888.768.3476 to schedule an appointment or book online to find a leading vein treatment clinic near you.
Consult with a Vein Specialist
FAQs About Visible Veins
Why are my veins so visible on my arms and hands?
Visible veins on the arms and hands may appear due to factors such as heat, aging (which thins the skin), low body fat, genetics, exercise, hormonal fluctuations, anxiety, and stress.
Does dehydration make veins more visible?
Dehydration can make veins more visible. If you are not drinking enough water, your blood can thicken, requiring more pressure to pump through your body. This extra pressure can cause veins to bulge.
When should you worry about very visible veins?
You should worry about visible veins accompanied by symptoms such as pain, swelling, tenderness, or heaviness in the legs. It’s also important to pay attention to any veins that are very visible if you have a history of blood clots, or if you develop new symptoms like skin changes, ulcers, or a tender lump in the leg.
What test confirms vein disease?
A duplex ultrasound is the most accurate and widely used diagnostic test for confirming CVI.