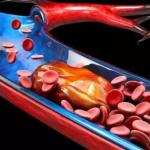
Although varicose veins are often considered an aesthetic issue, they are a symptom of vein disease. Varicose veins can cause a range of painful and uncomfortable symptoms, along with placing you at increased risk for several serious health issues like blood clots and venous ulcers.
If you are concerned about potential varicose vein problems, we recommend consulting a vein specialist for a full evaluation.
SCHEDULE A CONSULTATION ONLINE
What to Know About Varicose Veins
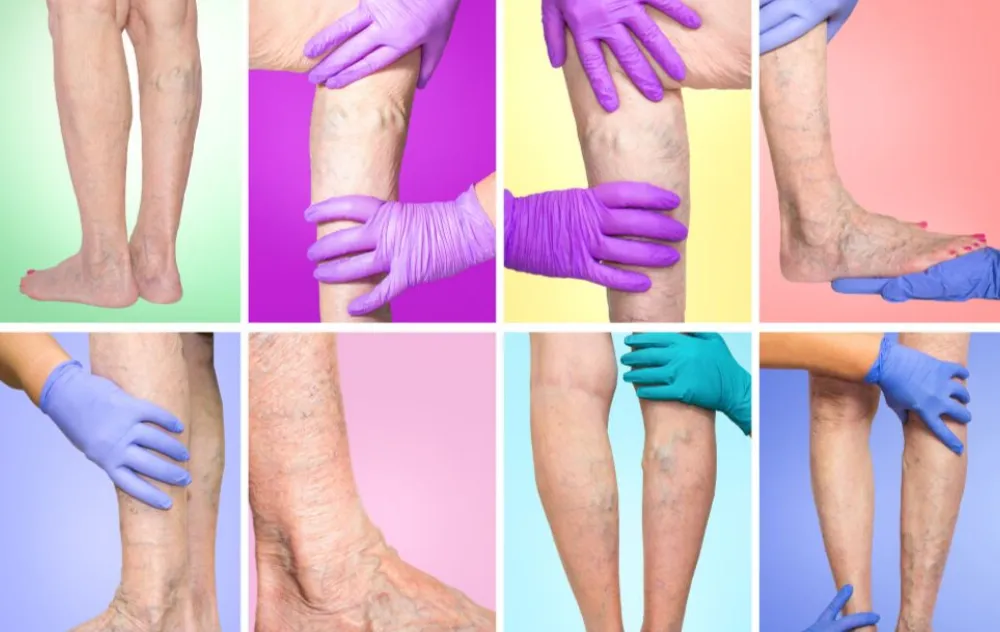
Varicose veins are enlarged, twisted veins that can appear dark blue or purple in color. Usually, they appear on the legs or feet as a result of standing or sitting for prolonged periods, which places pressure on the veins in your lower extremities. Genetics and additional lifestyle factors are also contributing factors to the development of vein disease.
Often, varicose veins don’t cause any symptoms whatsoever. Some individuals, on the other hand, experience pain and discomfort due to:
- Muscle cramps
- Bleeding
- Achy or heavy feeling in the legs
- Worsening pain from standing or sitting
- Burning sensation
- Throbbing
- Muscle cramping
- Swelling in the lower legs
- Red discoloration of the skin
Take Our FREE VEIN Symptom Quiz
Are Varicose Veins Dangerous If Not Treated?
Varicose veins are a sign of underlying vein disease and may require treatment. All varicose veins should be evaluated by a medical professional.
Vein disease is a progressive condition. Even if your varicose veins are not bothersome, they may eventually lead to symptoms like leg swelling, cramping, itching, and fatigue. Beyond that, enlarged veins place you at risk for several dangerous venous conditions, including blood clots and venous ulcers.
Varicose veins are a sign of underlying vein disease and may require treatment. All varicose veins should be evaluated by a medical professional.
Vein disease is a progressive condition. Even if your varicose veins are not bothersome, they may eventually lead to symptoms like leg swelling, cramping, itching, and fatigue. Beyond that, enlarged veins place you at risk for several dangerous venous conditions, including blood clots and venous ulcers.
When Are Varicose Veins Dangerous?
Varicose veins are always considered dangerous because they can lead to other concerning health conditions, including bleeding veins, deep vein thrombosis (DVT), supraventricular tachycardia (SVT), venous ulcers, and lipodermatosclerosis.
Below, we discuss these issues and explain what to be on the lookout for. Early diagnosis and treatment usually leads to the most desirable health outcomes.
Bleeding Varicose Veins
Varicose veins near the surface of the skin can rupture or begin to bleed as a result of an injury. This condition is sometimes referred to as “leaky veins” and is not typically painful. For instance, veins that leak near the ankle may bleed spontaneously but not cause any tenderness or pain.
Varicose veins tend to leak when their walls stretch and weaken due to pooling blood. Although unusual, blood from a leaking varicose vein can shoot several feet away from its source. When bleeding is significant, it can be life-threatening.
Varicose Veins and Supraventricular Tachycardia
When varicose veins are present, another potential issue that can arise is supraventricular tachycardia (SVT). This term describes a condition involving fast or erratic heart beats that affect the upper chamber of the heart. The heart rate speeds up as a result of abnormal electrical impulses in the heart and affects blood flow in the rest of the body.
Common symptoms include:
- Heart pounding
- Heart palpitations
- Dizziness
- Lightheadedness
- Fainting or near-fainting episodes
- Fatigue or a lack of energy
- Shortness of breath
- Chest discomfort
- Throat tightness
- Sweating
SVT can cause issues with your circulatory system since the veins and arteries must work harder to compensate for an unhealthy heart. To alleviate symptoms, both varicose vein and SVT treatment may be necessary.
Varicose Veins and Deep Vein Thrombosis
Deep vein thrombosis (DVT) is a serious health condition that occurs when a blood clot develops in the deep venous system. The deep veins are nestled between the muscles, so they’re not visible to the eye.
Along with causing painful symptoms, a blood clot in the deep veins can break off from its original location and lead to a life-threatening issue called pulmonary embolism. Pulmonary embolism occurs when a blood clot travels to a lung artery and blocks blood flow. If you experience sudden leg pain and swelling, shortness of breath, coughing, chest pain, clamminess, or fever, seek medical evaluation immediately.
Varicose Veins and Leg Ulcers
A leg ulcer is a type of painful sore that occurs when skin on the leg breaks down. As the skin breaks down, air and bacteria enter into the tissue. Many non-healing wounds heal over the course of a week or two, whereas others remain longer or worsen. We recommend seeking treatment for both types.
Venous conditions can lead to ulcers as a result of pressure in the vascular system. In fact, approximately 80% of all leg ulcers stem from the veins not working properly. The same underlying condition, known as vein disease or venous insufficiency, can also lead to the formation of varicose veins.
Both venous ulcers and varicose veins can occur when tiny, one-way valves in the veins of your legs become damaged. This results in veins that are unable to efficiently transport blood back to your heart. Instead, blood begins to flow backwards or pool in place.
The valves in your legs may become damaged over time as a result of both genetic and lifestyle factors.
Lipodermatosclerosis and Venous Disease
Some varicose vein problems are lesser known. If you have vein disease, you may be at increased risk for lipodermatosclerosis, an inflammatory condition of the subcutaneous fat in the lower portion of the legs. Lipodermatosclerosis can affect one leg or both of them. People who have the condition usually notice swelling above the ankle initially.
In its early stage, the condition appears similar to cellulitis, a type of skin infection. Symptoms include pain, swelling, and redness. As the condition progresses, it becomes chronic and may cause the skin to harden or thicken. You may also notice increased pigmentation or small white scars in the area.
It’s also possible for lipodermatosclerosis to cause fluid retention in the legs, making them appear larger near the ankles. Symptoms of lipodermatosclerosis can range from mild to severe.
Typically, women develop lipodermatosclerosis more than men. It usually impacts individuals with chronic venous insufficiency or varicose veins, although the connection between these conditions isn’t fully understood. If you experience symptoms, contact a vein specialist as soon as possible.
MORE QUESTIONS? TALK TO A VEIN SPECIALIST TODAY
When to See a Doctor About Varicose Veins
The best way to find out if your varicose veins are considered problematic is to visit a vein specialist. Vein treatment can help alleviate painful symptoms and reduce your risks of developing complications.
Prior to your appointment, it may be helpful to take note of vein color and track changes over time. Colors changes may signify a serious vascular problem is occurring. The skin around a vein also tells a lot about the condition of the vein. For instance, inflammation, pigmentation changes, and changes in the texture of the skin can indicate disease progression.
When evaluating the skin near varicose veins, be on the lookout for ulceration. Ulcers can occur not only as a result of venous problems, but they can also indicate diabetes or another serious issue. It’s vital to seek the assistance of a specialist to determine the cause. Typically, your blood vessels are flexible tubes that carry blood to and from the heart. It’s an indication of a problem if you experience hardening in a vein. It could mean there’s a clot that’s preventing blood from flowing normally.
For expert medical evaluation and personalized treatment recommendations, consult a vein specialist.
Request a Consultation at USA Vein Clinics
Since varicose veins can be dangerous, we always recommend their evaluation by a vein specialist. At USA Vein Clinics, our highly-skilled vein specialists are available to evaluate your vein health in state-of-the-art treatment centers across the nation.
If you have varicose veins or other venous symptoms, we usually recommend treatment for vein disease. For a personalized treatment plan, contact USA Vein Clinics today by calling 888.768.3467 or scheduling an appointment online.