Varicose veins are often considered a strictly cosmetic problem; however, they’re a symptom of vein disease, which can lead to serious health issues if left untreated. Treatment can diminish unattractive, bulging veins, improve blood circulation, and alleviate debilitating symptoms. Something you may not know, though, is that your blood pressure and your varicose veins are related.
Schedule a Consultation With a Vein Specialist
Do Varicose Veins Cause High Blood Pressure?
You might wonder if your veins can influence your blood pressure, and in some cases, the answer is yes. There is clear evidence that hypertension can lead to the development of varicose veins. And, varicose veins can lead to a condition known as venous hypertension.
What are Varicose Veins?
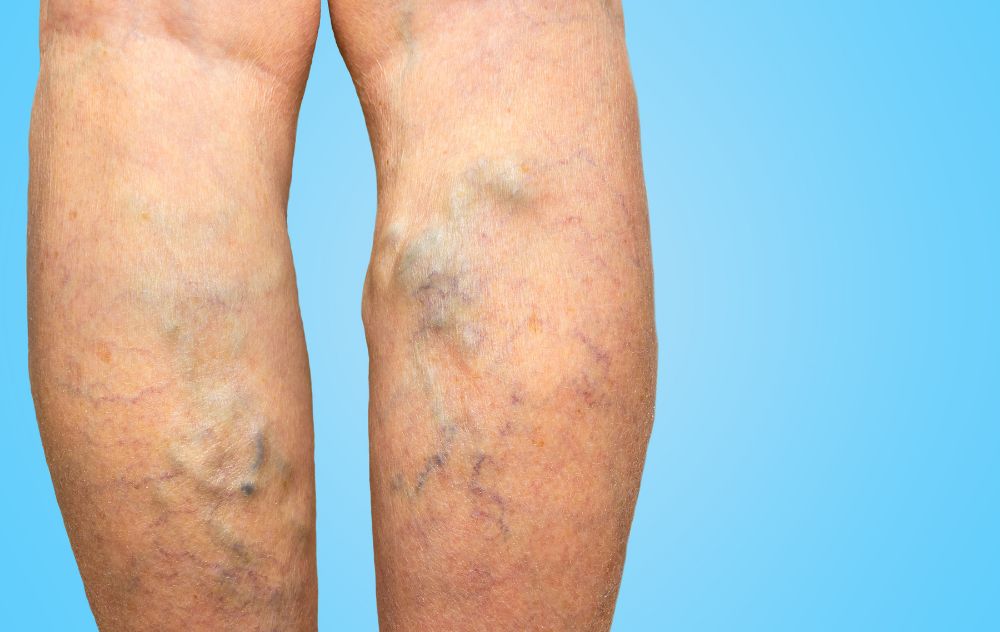
A varicose vein is a vessel that carries blood to the heart and protrudes through the skin. This gnarled, enlarged vein stands out among your other blood vessels. Although a varicose vein is possible in any vein, most of the time, the veins that become varicose are in your legs and feet because of the pressure you put on them when you stand or walk. Since varicose veins cause pressure to build up in the veins of the legs, varicose veins can increase your blood pressure.
What Causes Varicose Veins?
Veins are responsible for carrying blood from other places of your body to your heart for it to recirculate. Unfortunately, veins in the lower portion of your body must fight gravity, making them work harder. As a result of the veins working hard, their valves become damaged or weaken, causing blood to back up. When it does so, the blood pools into your veins, which causes them to bulge and become more prominent due to the building pressure. In some cases, they twist to squeeze into their confined space.
As you age, your veins naturally lose their elasticity, causing them to stretch and weaken. As they become weaker, they’re more prone to becoming a varicose veins. Women tend to develop varicose veins more than men, especially during pregnancy and menopause. The hormone changes before menstruation increase a woman’s risk as well. Other risk factors include:
- Family history
- Living a sedentary life
- Having an occupation where you stand for long periods of time
- Obesity
Varicose Veins and Venous Hypertension
Damage to the valves in the leg veins leads to venous hypertension. Due to the damage, blood starts to collect in the lower legs. The heart is under more stress as the blood continues to pool because more force is required to return the blood to the heart.
The entire cardiovascular system must function together to pump blood throughout your body. When one portion of the cardiovascular system has to work harder than it should, it causes the entire system to compensate for the inefficiency. A National Library of Medicine study examined the risk of arterial disease and hypertension in people with varicose veins. A five-year study found that new arterial disease occurred significantly more often in individuals with varicose veins. [1]
When veins cannot send blood back to your heart efficiently, it’s known as venous insufficiency. Varicose veins and weakness of the veins in the legs can cause pressure to build up in the legs, which can then cause venous hypertension as a result. Venous hypertension can sometimes lead to changes in skin color, leg ulcers, or swelling in the lower portion of the legs or ankles.
Varicose Veins and Hypotension (Low Blood Pressure)
Varicose veins don’t just cause high blood pressure; they can even cause low blood pressure, called orthostatic hypotension. This form of low blood pressure occurs when your blood vessels fail to constrict, which causes a sudden drop in blood pressure when standing up from lying down. Orthostatic hypotension can be caused by multiple conditions, including varicose veins, so if you chronically experience sudden dizziness when standing and you have varicose veins, you should reach out to a healthcare professional to determine the underlying cause of your hypotension.
If you experience high or low blood pressure and have varicose veins, you may want to consult a vein specialist to evaluate your condition and determine the best course of treatment. At USA Vein Clinics, we have over 160 vein treatment clinics across the United States so that you can get the care you need.
Risk Factors of Varicose Veins and High Blood Pressure
Varicose veins and high blood pressure may occur simultaneously in people because they both share some of the same risk factors. For example, you’re more at risk for hypertension and varicose veins as you age. Men tend to develop high blood pressure around 45, while women tend to develop it after age 65. Additionally, the aging process places wear and tear on the valves in the veins, making varicose veins more likely as you age.
Being overweight or obese increases your risk for varicose veins and high blood pressure. The amount you weigh affects the amount of blood you have, and when you have more blood, it takes more pressure to circulate it throughout your cardiovascular system. If you’re overweight, you’re placing extra weight on the veins in your legs, which adds to your risk of developing varicose veins.
A sedentary lifestyle puts you at a greater risk of numerous health conditions, including hypertension and varicose veins. When you sit for long periods, your blood doesn’t flow as well, increasing your risk of developing varicose veins. Less physically active people tend to have higher heart rates, so your heart must work harder. You’re also at a greater risk of obesity when you lead an inactive lifestyle, increasing your risk of hypertension.
The likelihood of a woman developing varicose veins is higher than a man’s due to hormone changes like pregnancy, birth control pills, and menopause. Although men are at a greater risk of developing hypertension, the hormonal fluctuations that increase a woman’s risk of developing varicose veins are the same ones that increase a woman’s chance of hypertension.
Do Varicose Veins Cause Other Health Risks?
Varicose veins can sometimes indicate more serious vein problems. For example, supraventricular tachycardia is a rapid heart rhythm disorder that starts in the upper region of the heart. Due to abnormal electrical impulses in the heart, the rate it beats increases, leading to the heart working hard because it doesn’t fill up before it contracts. The veins and arteries also work harder, increasing a person’s risk of developing varicose veins.
Leg ulcers also can occur in your legs due to high pressure in your veins when you stand. The pressure in your veins damages the skin, which in return, causes an ulcer to form. The connection between lipodermatosclerosis and varicose veins isn’t known yet, but this condition of leg swelling contributes to the onset of varicose veins.
Treatment for High Blood Pressure Caused by Varicose Veins
Treatment for varicose veins can impact your blood pressure if you have venous insufficiency, but in most cases, varicose veins and high blood pressure require separate treatments. At USA Vein Clinics, we only offer treatments for vein diseases that are non-surgical, minimally invasive, and can be done in an outpatient setting. Depending on the severity of your condition, treatment can take as little as 30 minutes. After your procedure, you should be able to return to normal activities within one week.
Treat Your Varicose Veins
Whether you have varicose veins, spider veins, or venous ulcers, our clinics treat a variety of vein disease conditions. If you believe you are suffering from high blood pressure due to vein disease, contact us at 888.768.3467 to learn more about which treatment would work best for you, or you can click the button below to schedule your appointment online.
Schedule An Appointment Online Today
[1] National Library of Medicine arterial disease and varicose veins
[2] American Heart Association, High Blood Pressure and Women