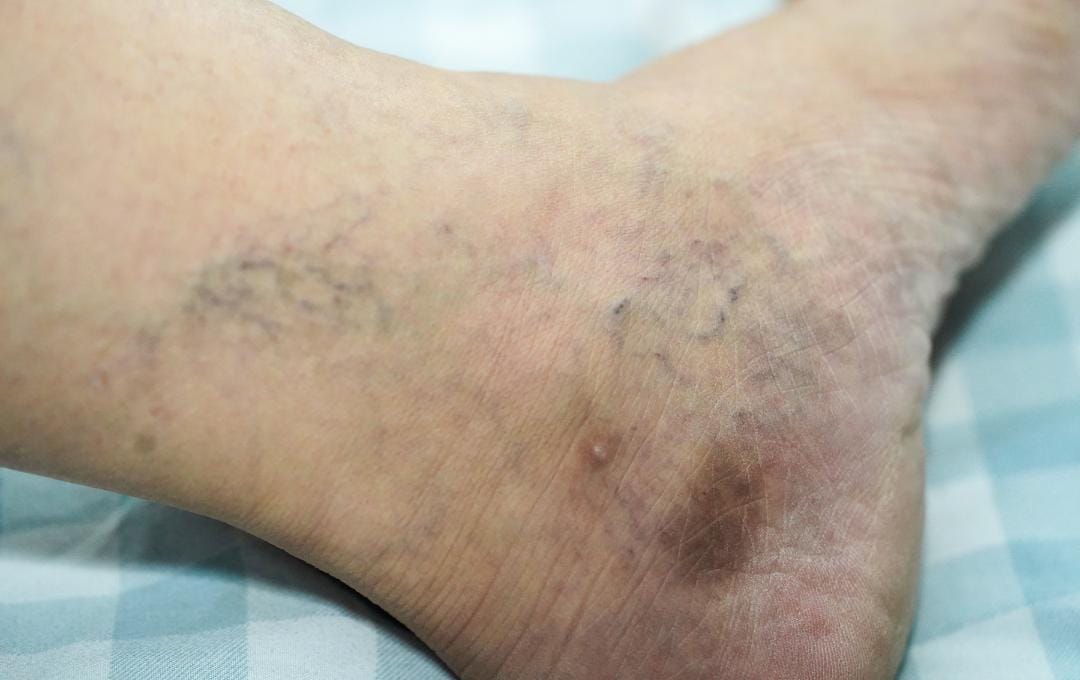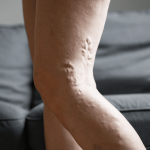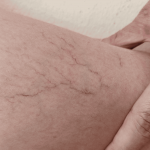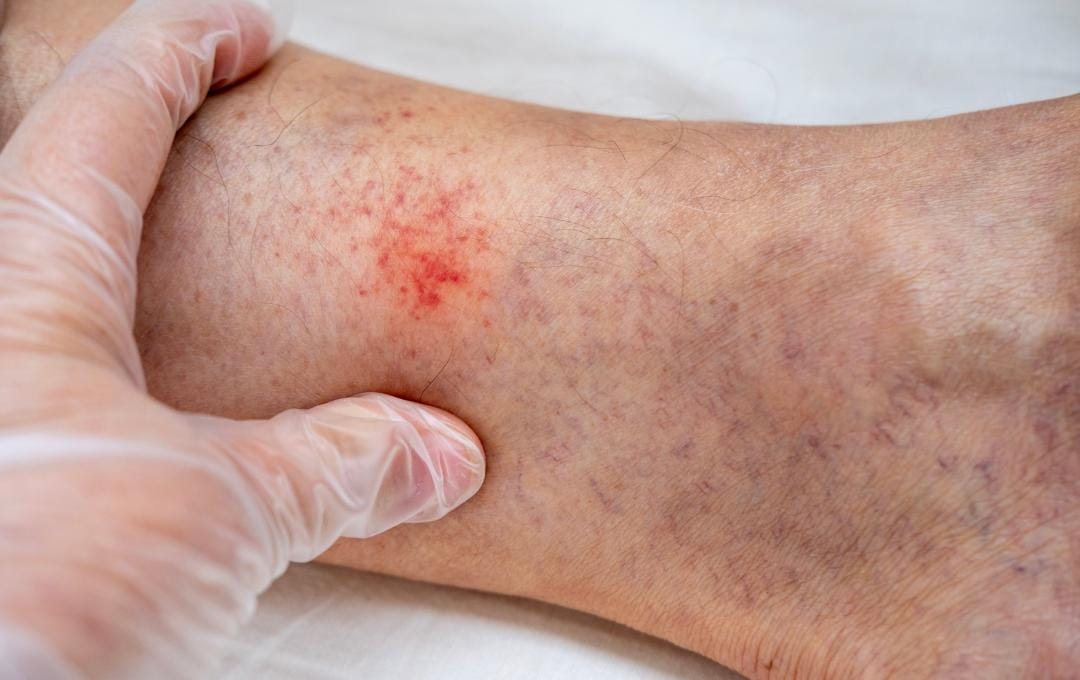
If you’ve noticed persistent skin changes on your lower legs and ankles, such as itching, redness, or eczema-like patches, it may be more than a simple rash. It may be stasis dermatitis, a common inflammatory skin condition caused by impaired blood flow in the legs. This condition is closely associated with vein disease or chronic venous insufficiency.
Left untreated, the condition can progress, leading to skin breakdown or non-healing wounds on the legs. Understanding the causes, symptoms, and treatment options for stasis dermatitis is essential for protecting your skin and overall vascular health.
What Is Stasis Dermatitis?
Stasis dermatitis — also known as venous stasis dermatitis or varicose eczema — is a skin condition that signals the progression of chronic venous insufficiency (CVI). CVI happens when tiny, one-way valves inside the veins that help bring blood back to the heart become weak or damaged.
When vein valves fail, blood collects in the lower legs instead of returning to the heart. This sustained pressure damages surrounding tissues and triggers chronic inflammation.
What Causes Stasis Dermatitis?
Stasis dermatitis is primarily caused by excessive pressure on the leg veins (venous hypertension). Smaller blood vessels connecting the veins and arteries (capillaries) leak inside the skin. This causes the skin to swell, thicken, and harden, leading to dry, discolored patches similar to eczema.
Certain conditions and characteristics lead to stasis dermatitis, including:
- Previous blood clots or family history of clotting
- Excess weight
- Standing or sitting for long periods
- Aging
- Pregnancy
- Previous injury or surgery
Stasis Dermatitis Symptoms
Recognizing stasis dermatitis symptoms in the lower legs or ankles early can help prevent complications. Symptoms often develop gradually and include:
- An itchy red mark or discolored patches on the legs or ankles
- Swelling in the lower legs
- Thickened or leathery skin
- Flaking or scaling
- Oozing or crusting in severe cases
In advanced cases, untreated stasis dermatitis can lead to open sores called venous ulcers. According to the National Institutes of Health, venous ulcers account for nearly 70 to 90 percent of chronic leg wounds in older adults. If you notice open sores on your legs that haven’t healed after two to four weeks or show signs of an infection, seek an evaluation.
Many patients with CVI often dismiss their symptoms as signs of aging, fatigue, or a long day on their feet. However, mistaking vein disease as something else allows it to progress into skin changes. Common symptoms include:
- Pain or cramping
- Swelling
- Fatigue
- Aching or heaviness
- Visible varicose veins or spider veins
If these symptoms sound familiar, a vein screening can help determine whether CVI is the underlying cause.
How Do You Treat Venous Stasis Dermatitis?
Effective stasis dermatitis treatments focus on improving circulation and reducing inflammation. While creams may temporarily ease itching, addressing the underlying cause can lead to longer-lasting improvement.
Conservative Management of Stasis Dermatitis
Conservative management involves non-invasive, supportive methods that include:
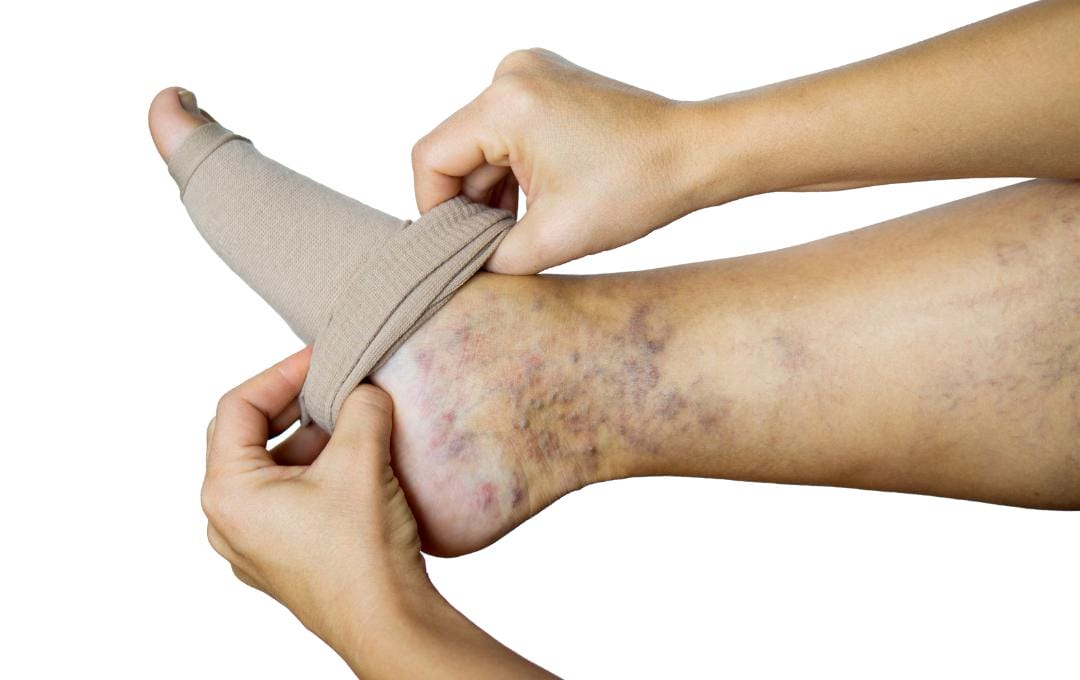
- Compression therapy: Compression stockings apply pressure to the ankles to help support healthy blood flow and reduce swelling.
- Leg elevation: Propping the legs above the heart several times daily helps blood move back towards the heart.
- Moisturizers: Gentle skin moisturizers protect the skin barrier and reduce dryness.
- Lifestyle changes: Incorporate movement throughout the day to avoid prolonged sitting or standing.
While these measures can reduce discomfort, persistent symptoms often indicate underlying vein dysfunction. The next step is identifying whether CVI is contributing to your skin changes.
Importance of Vein Screenings for Prevention
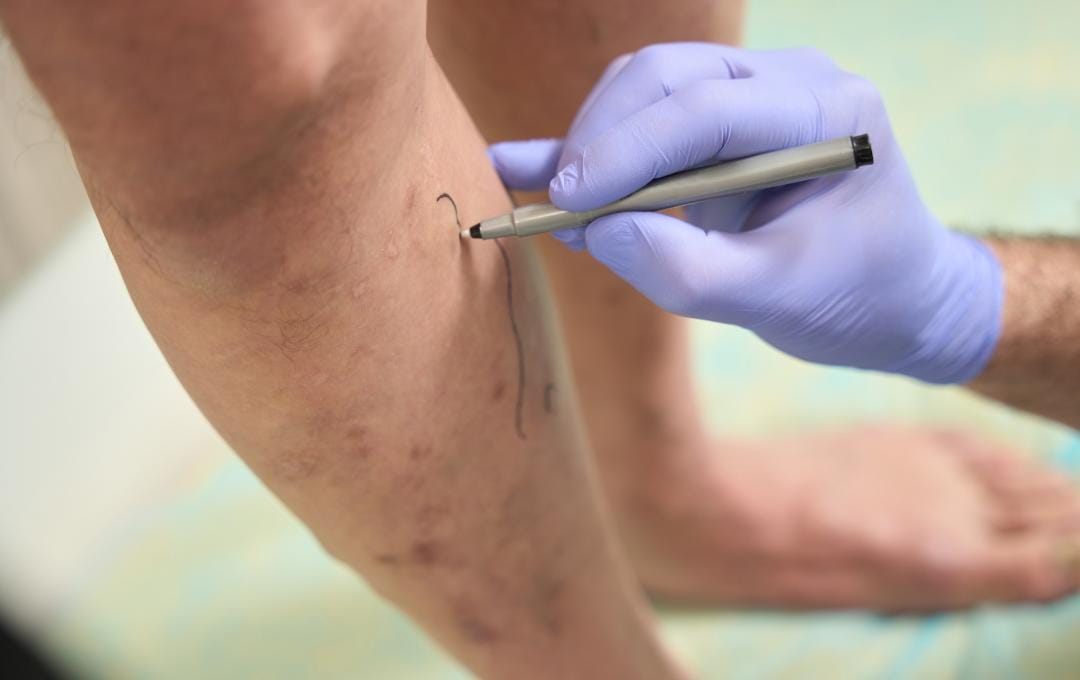
Vein screenings provide a closer look inside your veins. Vein specialists use advanced tools, such as a Doppler ultrasound, to pinpoint vein valve failure and abnormal blood flow, allowing early intervention before the underlying vein disease worsens.
Preventive benefits include:
- Identifying vein reflux early
- Reducing the risk of ulcers
- Supporting long-term stasis dermatitis management
Once the vein specialist provides an accurate diagnosis, they will recommend a personalized treatment plan to restore healthy blood flow and prevent further skin damage.
Minimally Invasive Vein Treatments
For patients with chronic venous insufficiency, minimally invasive procedures can reduce vein pressure and reroute blood flow to promote healing from stasis dermatitis. These treatments may also improve accompanying symptoms, such as leg swelling and visible veins, and can be personalized to fit each patient’s condition.
Common treatment options include:
- Endovenous Laser Therapy (EVLT): Uses laser energy to close malfunctioning veins.
- ClariVein®: Combines mechanical and chemical ablation to address larger veins.
- Varithena Vein Treatment: Injects a specialized foam to close twisted veins.
- Venaseal™: Seals the vein shut with a medical adhesive.
- Sclerotherapy: Injects a sclerosing agent into smaller varicose veins and spider veins to collapse them.
- Radiofrequency Ablation (RFA): Applies controlled heat to seal diseased veins.
Contact USA Vein Clinics
If you’re experiencing persistent redness, swelling, or irritation around your lower legs, it may be time to look beyond topical creams. Addressing circulation concerns can protect both your skin and overall vascular health.
USA Vein Clinics has more than 20 years of experience diagnosing and treating vein disease across the country. Their vein specialists, many of whom are board-certified, use advanced imaging and minimally invasive procedures designed for patient comfort and safety.
Patients choose USA Vein Clinics for:
- Streamlined, convenient care without a hospital stay.
- High-quality, evidence-based treatment plans.
- Experienced vein specialists focused exclusively on vein care.
- Comprehensive evaluations.
If your symptoms suggest stasis dermatitis, start your path toward better health by scheduling a consultation.
FAQs about Venous Stasis Dermatitis
Can chronic venous insufficiency be mistaken for eczema?
Chronic venous insufficiency (vein disease) often causes skin irritation that resembles eczema. However, skin changes from CVI usually appear on the lower legs and are accompanied by swelling or visible veins. A Doppler Ultrasound can confirm the diagnosis.
Is stasis dermatitis dangerous?
Untreated stasis dermatitis can be dangerous because, if untreated, the skin can break down into non-healing wounds. These wounds can become infected and lead to sepsis if they are not addressed promptly.
Can stasis dermatitis be cured?
Stasis dermatitis cannot be cured; however, addressing the underlying cause of stasis dermatitis can significantly improve symptoms and the appearance of the legs. Vein treatment can alleviate symptoms related to vein disease, including pain, tired limbs, and swelling. These treatments also reduce the risk of vein disease complications, like venous ulcers and DVT.