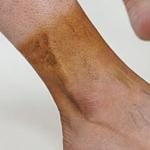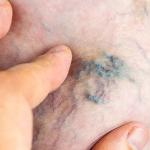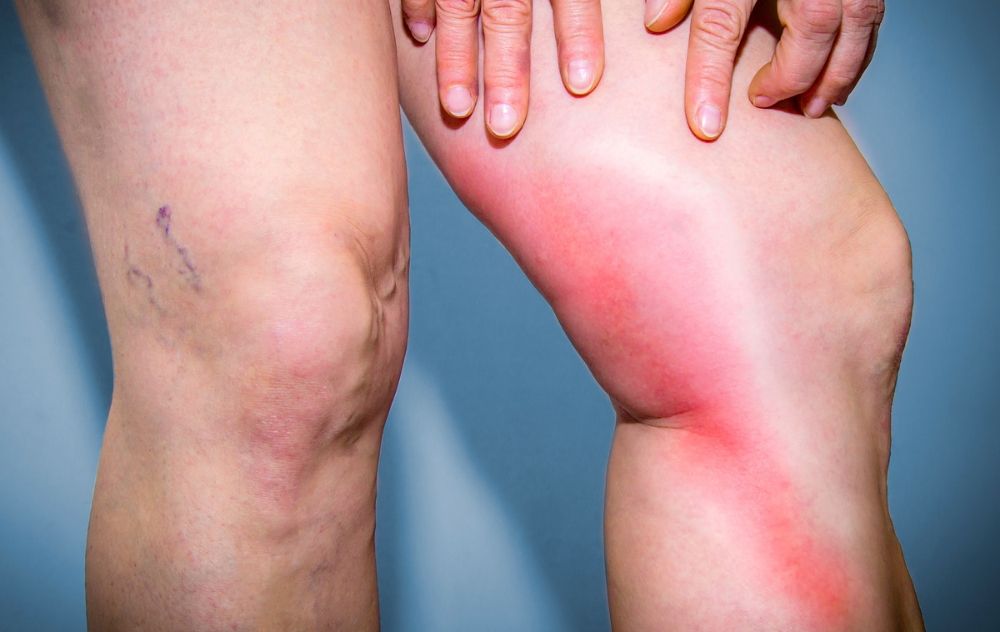

Are your legs feeling tender, swollen, or unusually warm? You might be experiencing a common vascular condition known as phlebitis. By definition, phlebitis simply means the inflammation of a vein. While it most frequently occurs in the legs, understanding what phlebitis is and recognizing its symptoms early is important for protecting your circulation. Whether it is a mild surface irritation or a sign of a deeper vein issue, knowing what causes it, how long it lasts, and how to treat it can make all the difference. Read on to learn how to spot the signs of phlebitis, manage the discomfort, and discover when it could be time to seek a professional vein screening.
Phlebitis Definition and Meaning
The definition of phlebitis is relatively straightforward. Phlebitis is the medical term for the inflammation of a vein. This inflammation can cause the affected vein to swell, become tender, and turn red or warm to the touch, most commonly occurring in the legs.
When searching for answers online, it’s easy to get tripped up by medical terminology. It is important to note that “flebitis” is a very common search variant and phonetic misspelling. Whether you spell it with a “ph” or an “f,” the meaning remains exactly the same, and the underlying condition requires the same careful attention.
Understanding what phlebitis is also means knowing that it typically falls into two main categories, depending on where the inflammation occurs:
- Superficial Phlebitis: This affects veins close to the surface of your skin. While it can be uncomfortable, it is usually temporary and less serious.
- Deep Vein Thrombosis (DVT): This affects the larger, deeper veins farther inside the leg. DVT is a more critical condition because it carries the risk of blood clots traveling to the lungs.
Recognizing these differences can help your vascular health by helping you know when to seek professional care.
What Causes Phlebitis?
The main cause of phlebitis isn’t just a single trigger. Phlebitis occurs when a vein becomes irritated or damaged, which can happen for several different reasons.
Understanding what causes phlebitis can help you identify your personal risk factors. The most common causes of phlebitis include:
- Local Trauma or Injury: An injury to the vein wall—often caused by a medical procedure like inserting an intravenous (IV) catheter or drawing blood—is a frequent cause of superficial phlebitis.
- Inactivity and Sluggish Blood Flow: Extended periods of immobility, such as bed rest after surgery or sitting for long hours on an airplane, can cause blood to pool in the lower legs, triggering inflammation.
- Underlying Vein Conditions: For many individuals, phlebitis is linked to a deeper issue with circulation. Conditions like chronic venous insufficiency (CVI) weaken the vein valves, causing blood to flow backward and pool in the legs. This increased pressure and stagnation frequently lead to varicose veins and recurrent phlebitis.
- Blood Clotting Disorders: Certain medical conditions, genetics, or medications (such as hormone replacement therapy) that increase the risk of blood clotting can also lead to vein inflammation.
By identifying these underlying causes, you can take steps to improve your circulation and prevent future flare-ups. If you have any of these risk factors and think you may have phlebitis, take our quick symptom quiz to find out if you should seek medical attention.
What Does Phlebitis Look Like in the Legs?
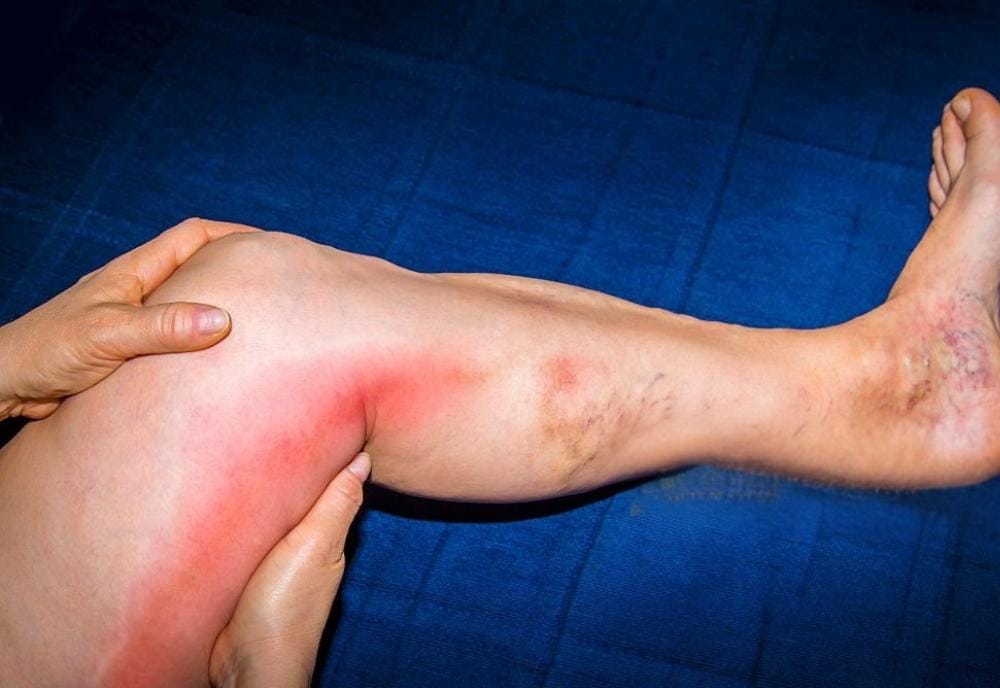

If you are wondering what phlebitis of the leg is, the visual signs are often your first clue. If you were to look up phlebitis leg pictures, you would typically see a distinct, red, or dark “cord-like” line tracing the path of a vein. When dealing with superficial phlebitis on the leg, the area directly over the vein will look raised, swollen, and highly flushed compared to the surrounding skin.
To easily recognize what phlebitis in the legs looks like, watch for these three main signs:
- A hard, red streak or cord beneath the skin.
- Localized swelling or a bumpy texture over the vein.
- Skin that looks shiny, red, or discolored.
If your leg matches this description, it is a clear indicator that your veins are inflamed and need a professional look.
Phlebitis Symptoms and Four Signs to Watch For
Recognizing the early signs of phlebitis can help you address vein inflammation before it escalates into a more uncomfortable or serious condition. While visual changes are common, the physical sensations you experience are just as telling. Understanding these phlebitis symptoms will help you determine what your leg pain is telling you and when it’s time to seek a medical evaluation.
The most common physical symptoms include:
- Tenderness and Pain: The area along the vein may feel sore, throbbing, or intensely tender to the touch, often worsening when you put weight on the leg.
- Warmth: The skin over the inflamed vein will feel noticeably hot or warm compared to the rest of your leg.
- Itching or Burning: You might experience a persistent itching or burning sensation directly over the affected vein.
Since many vein disease symptoms overlap, monitoring these changes closely is crucial. If you notice a tender, warm streak on your leg, it is highly recommended to have it evaluated by a specialist to ensure proper healing and protect your circulatory health.
Phlebitis vs Thrombophlebitis: What’s the Difference?
When researching vein health, you will frequently see the terms phlebitis and thrombophlebitis used interchangeably. While they are closely related and share similar symptoms, there is a key medical distinction between the two.
The main difference in the phlebitis vs thrombophlebitis debate comes down to the presence of a blood clot:
- Phlebitis: This is simply the inflammation of a vein. It can be caused by local trauma, an IV line, or poor circulation, but it does not necessarily involve a clot.
- Thrombophlebitis: This occurs when a blood clot (thrombus) forms inside the vein and causes inflammation.
If the clot is in a surface vein, it is called superficial thrombophlebitis. However, if it occurs in a deeper vein, it is known as deep vein thrombosis (DVT), a much more serious condition that requires immediate medical care.
Since thrombophlebitis is so closely tied to varicose veins, treating the cause of poor circulation is important. If you are experiencing symptoms of either condition, a comprehensive vein screening can help protect your legs from future complications.
How Long Does Phlebitis Last?
If you are dealing with the discomfort of an inflamed vein, your top priority is likely finding out how long phlebitis lasts. The timeline for recovery generally depends on whether the inflammation is on the skin’s surface or deeper in the leg.
For most standard cases of superficial phlebitis, the acute symptoms—such as the intense heat, redness, and sharp tenderness—typically begin to improve within a few days to a week. However, the healing process underneath the skin takes a bit longer. It is completely normal for the vein to feel hard, lump-like, or “cordy” for several weeks, and any skin discoloration or bruising around the area can also take a month or more to fully fade.
If your symptoms do not start to ease after a week, or if the swelling and pain suddenly worsen, it could be a sign of a more serious deep vein issue. Persistent symptoms mean it is time to have your legs evaluated by a vascular specialist to ensure your veins are healing safely.
When to See a Vein Specialist for Phlebitis
While mild phlebitis symptoms can sometimes improve with home care, knowing when to transition from home remedies to medical evaluation is vital for your vascular health. Because vein inflammation can mimic or lead to more serious conditions, recognizing the early signs of phlebitis can prevent long-term complications.
You should schedule an appointment with a vein specialist if you notice:
- Symptoms that do not improve or worsen after a few days of elevation and warm compresses.
- Increased swelling, redness, or pain spreading further up your leg.
- A hard, painful lump near your groin or knee.
If your leg swelling is sudden and severe, or if your leg pain is accompanied by chest pain or shortness of breath, seek emergency medical attention immediately, as these can be signs of a dangerous deep vein clot (DVT). A vein specialist can properly assess your veins, rule out deep tissue clots, and provide a targeted treatment plan to get you back on your feet comfortably.
Treatment Options for Phlebitis

When dealing with vein inflammation, many patients ask, what is the fastest way to get rid of phlebitis? While mild superficial cases can be managed at home, the quickest and most effective route to recovery always depends on the underlying cause.
For quick at-home symptom relief, you can start with the basics:
- Apply warm compresses to the area for 15–20 minutes several times a day.
- Elevating your legs above heart level to reduce swelling.
- Taking over-the-counter anti-inflammatory medications (like ibuprofen) to ease pain.
However, home care only masks the symptoms; it doesn’t fix the problem. If your phlebitis is caused by underlying venous insufficiency (poorly functioning vein valves), the inflammation is likely to return.
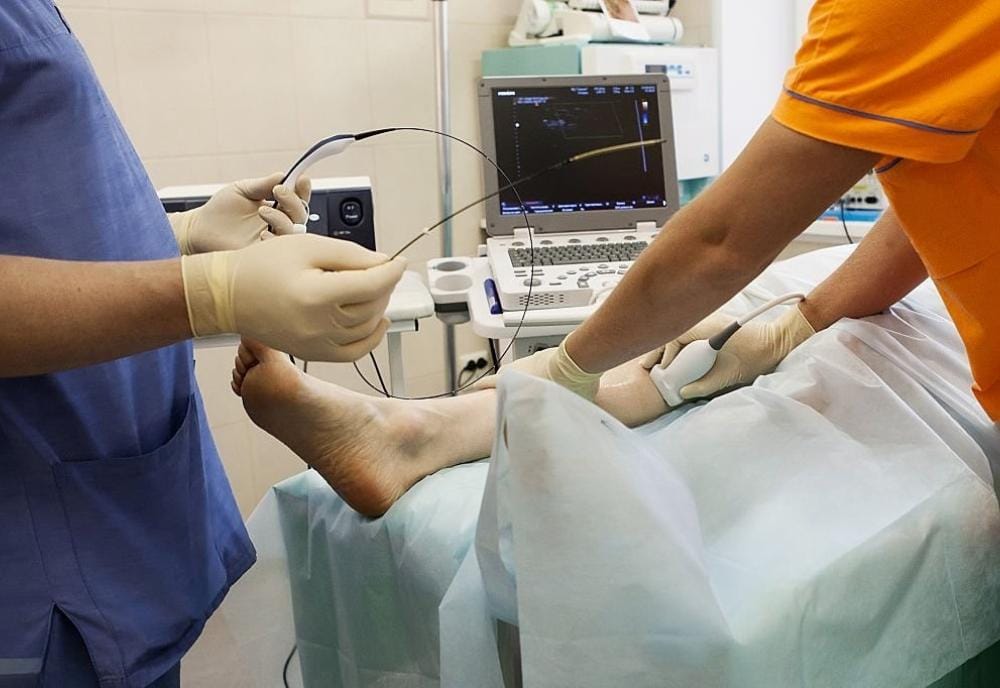
To permanently resolve the issue and prevent future flare-ups, professional medical intervention is key. Modern, minimally invasive treatments, offered at USA Vein Clinics, can safely close off the damaged veins, redirecting your blood flow to healthier pathways and providing long-term relief.
Get Expert Answers at USA Vein Clinics
If you suspect you are dealing with phlebitis, you shouldn’t have to guess about your vein health. At USA Vein Clinics, our experienced vein specialists provide expert evaluations to pinpoint the exact cause of your discomfort. Using advanced, non-invasive ultrasound diagnostics, we can check for underlying venous reflux (poor blood flow) or hidden blood clots to ensure you receive an accurate diagnosis.
If an underlying vein issue is found, we offer safe, minimally invasive treatments designed to restore healthy circulation with little to no downtime. We make prioritizing your health simple and affordable by accepting most major insurance plans, including Medicaid and Medicare.
Use our convenient online scheduling tool to book your appointment today.
FAQs About Phlebitis
What is the fastest way to get rid of phlebitis?
The fastest way to ease superficial phlebitis is to reduce inflammation. You can speed up your comfort by applying warm compresses to the area for 15–20 minutes several times a day, elevating your legs above heart level while resting, and taking over-the-counter anti-inflammatory medications if approved by your doctor.
How long does phlebitis last?
Mild cases of superficial phlebitis usually begin to improve and feel better within a few days to a week. However, the visible redness, skin discoloration, or the hard, “cord-like” feel of the vein itself can take several weeks to completely disappear.
What is the difference between phlebitis vs thrombophlebitis?
Phlebitis is a broad term that simply means a vein is inflamed. Thrombophlebitis means the vein is inflamed because a blood clot has formed inside it. In other words, thrombophlebitis is a specific type of phlebitis where a clot is actively causing the irritation.
What is the difference between phlebitis vs. DVT?
Phlebitis is a generally non-life-threatening inflammation of a vein near the skin’s surface, whereas DVT (deep vein thrombosis) is a serious blood clot in a deep vein that carries a high risk of traveling to the lungs.