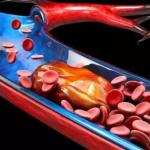
How to Prevent Blood Clots While Traveling
Varicose veins can make everyday activities, let alone travel, a challenge. The discomfort and pain associated with this condition can make simple tasks difficult and limit one’s ability to enjoy life.
While some people do not experience symptoms of vein disease, others struggle with chronic pain and discomfort, along with visible veins. These symptoms can worsen when sitting for long periods of time, such as while traveling by plane or car. Traveling can also place you at increased risk for developing dangerous blood clots in the leg.
Blood clots tend to develop while traveling as a result of poor circulation from sitting for hours. If you have varicose veins, it’s important to be mindful of any potential risks and to understand what steps to take to prevent blood clots while traveling.
If you have upcoming trips that involve traveling, the vein specialists at USA Vein Clinics are available to provide personalized recommendations on varicose veins when driving or flying. While both flying and driving for long periods can increase your risk of blood clots, there are some key differences in how to mitigate those risks. Discover practical tops to keep your blood flowing smoothly and what symptoms to look out for if you’re traveling with varicose veins.
Varicose Veins Increase Your Risk of Blood Clots When Traveling

The risk of developing blood clots increases when you travel, especially if you are sitting or standing still for an extended amount of time. Blood clots occur when blood thickens and clumps together or when a blood vessel is damaged. Varicose veins increase the risk of developing blood clots because the vein walls can no longer provide support to the vessels, and this increases the likelihood that a clot can form.
One such condition, known as traveler’s thrombosis, also known as deep vein thrombosis (DVT), is a type of blood clot that forms in the deep veins of the legs. It often occurs when people are immobile for long periods, such as during air travel, train rides, bus trips, or a long car journey. Though anyone can be at risk for DVT, individuals with varicose vein are particularly susceptible.
DVT is often referred to as a “silent condition” because some people may experience no symptoms. However, the most common symptoms of DVT are leg pain, swollen ankles, discoloration, red blotches on legs, cramping, or warmth in the affected area. The longer you are immobile, the greater your risk of developing DVT. When left untreated, DVT can travel through the bloodstream to the lungs, causing a pulmonary embolism, a life-threatening condition.
Symptoms of pulmonary embolism include:
- Chest pain
- Difficulty breathing
- Shortness of breath
- Coughing up blood
If you notice any of these issues, seek urgent medical care.
Additional DVT risk factors include age, genetics, obesity, smoking, poor diet, and pregnancy. If you are concerned about driving or flying with varicose veins, it may be beneficial to consult a vein specialist.
How to Avoid Blood Clots When Flying
Understanding blood clots can help you avoid them.
Factors to Consider When Flying:
- Limited Mobility: Airplane seats are often cramped, limiting your ability to move around freely.
- Dehydration: The low humidity in airplane cabins can contribute to dehydration, which can thicken your blood and increase clotting risk.
- Cabin Pressure: Changes in cabin pressure can affect blood circulation
To reduce your risk of blood clots while flying, try the following:
- Drink water: Staying well-hydrated keeps vein walls from narrowing, along with regulating blood pressure.
- Move around: Take walks before your flight and during layovers to help prevent blood clots while flying. When safe to do so during your flight, get up to stretch and walk up and down the aisles. If stuck in your seat, try pointing and flexing your feet, rolling your ankles, or massaging your legs, ankles, and feet to improve blood circulation.
- Wear compression stockings: Wearing compression socks while flying with varicose veins is a great way to boost blood flow. Not only can this help prevent blood clots while traveling, but it can also alleviate venous symptoms like leg swelling and cramping.
- Don’t wear restrictive clothing: If you have varicose veins and flying is a concern, wear loose garments and comfortable footwear. Tight clothing and shoes can place additional pressure on your veins, further elevating the risk of blood clots.
- Elevate: Although not always possible, elevating your legs can reduce your varicose veins flying risk. This is because when you elevate your legs, less pressure is placed on your veins.
- Avoid alcohol or caffeine: Alcohol and caffeine is a diuretic and can dehydrate you. This forces the body to work harder to circulate blood, which may be dangerous if you have varicose veins.
If you have varicose veins, are predisposed to blood clots, or recently had vein treatment, make sure your doctor knows that you are planning a trip to fly. They can provide personalized recommendations on how to prevent blood clots while traveling.
How to Avoid Blood Clots While Driving
While driving, you have more mobility to move your legs and change positions. There are plenty of tips to prevent blood clots while traveling by car.
If you have varicose veins and driving plans, our vein specialists suggest:
- Take breaks: Get out of the car to stretch your legs by going on short walks, play Frisbee at a rest stop, or even take the stairs at a shopping center to encourage circulation, as well as reduce blood clot risks.
- Stay hydrated: Drink plenty of water to avoid dehydration.
- Change your position: With varicose veins and driving, the risk of developing blood clots comes from sitting in one position. Change your posture, your sitting position, and even your seat altogether as often as possible throughout the drive to help prevent blood clots while traveling.
- Stretch: Roll your ankles, flex your feet, wiggle your toes, and extend your legs to promote healthy circulation.
- Watch your diet: Try to avoid fast food en route. While the drive-thru may be convenient, foods high in sodium, fat, and cholesterol can take their toll on your veins. Instead, pack a cooler full of healthy options like fresh fruits and vegetables, along with sandwiches made from lean proteins or nut butter on whole-grain bread.
- Keep cool: Hot weather can cause leg pain. Keep cool and remember to drink water. Wear light clothing, blast the A/C, or roll down the windows.
Vein Treatment Before Your Trip
We understand that traveling can be stressful, especially when it comes to learning how to avoid blood clots when flying or driving. Although our tips can help prevent blood clots while traveling, they are not alternatives to treatment for vein disease, the underlying cause of varicose veins.
If you have an upcoming trip planned, we want you to know that vein treatment can reduce your varicose veins flying risk, ease painful venous symptoms, and improve the safety and quality of your travels. You may also benefit from following a healthier lifestyle. This may include losing weight, exercising more, improving your diet, or quitting smoking.
At USA Vein Clinics, our vein specialists offer a range of minimally invasive, office-based vein treatments for varicose veins, spider veins, and other venous issues. Our treatments are minimally invasive and require little downtime, allowing you to return home the same day as your treatment, resuming daily activities immediately.
We provide non-surgical vein treatment at over 168 locations nationwide. To learn more on how to avoid blood clots when traveling, schedule an appointment online or give us a call at 888.768.3467.
Medically Reviewed by:
Dr. Yan Katsnelson, M.D.
Dr. Yan Katsnelson is the founder and CEO of USA Vein Clinics. Dr. Katsnelson is a highly skilled cardiac surgeon who completed a fellowship at the Brigham and Women’s Hospital, Harvard School of Medicine, in Boston, MA. His clinical area of expertise includes minimally invasive procedures to treat vein and vascular diseases. Dr. Katsnelson has established himself as a strong advocate for accessible, affordable, and compassionate healthcare services. He spoke about the potential impact of COVID-19 on blood clots and vein health in a recent publication.