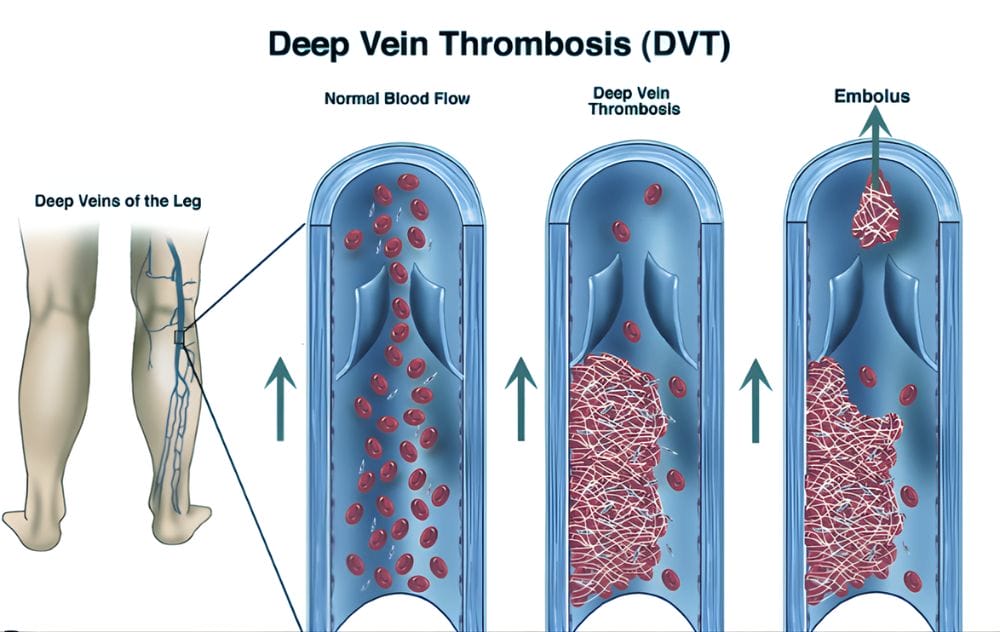
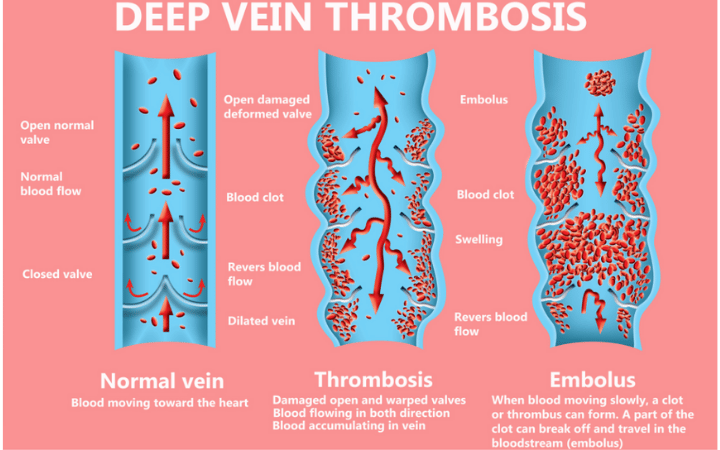
Deep Vein Thrombosis (DVT) is a serious vascular condition where a blood clot forms within a deep vein—most commonly in the legs, thighs, or pelvis. Since these veins carry blood back to the lungs and heart, a clot can become life-threatening if it breaks loose and travels to the lungs, causing a pulmonary embolism (PE).
As a result, DVT is considered a medical emergency and requires prompt evaluation and treatment.
Understanding what DVT is, why it happens, and how to recognize early signs can help reduce complications and protect your long-term health.
What Is Deep Vein Thrombosis (DVT)?
Deep vein thrombosis occurs when blood thickens and clots in the deep venous system, as opposed to superficial veins located closer to the skin. While superficial clots can be uncomfortable, venous DVT clots are far more dangerous due to their ability to travel through the bloodstream.
Venous thrombosis typically develops when blood flow slows, making the blood more prone to clotting or damaging the vein wall. If part of the clot breaks away, it can move to the lungs and block oxygen exchange, leading to a pulmonary embolism, a life-threatening complication requiring immediate medical care.
What Causes Deep Vein Thrombosis?
Vein health plays a major role in clot formation, so understanding the causes of deep vein thrombosis and contributing factors is essential.
DVT develops when three factors—known as Virchow’s triad—overlap, which include:
- Reduced blood flow (venous stasis): Venous stasis is more likely to occur if you are sitting or immobile for periods of time, including long flights, hospitalization, and sedentary work.
- Hypercoagulability (increased clotting tendency): Several conditions can increase the risk of clotting, including genetic disorders, hormonal medications (birth control, HRT), pregnancy and the postpartum period, cancer, smoking, and chronic inflammatory conditions.
- Vessel wall injury: A damaged vessel wall from trauma or surgery, leg injuries, or the placement of a catheter or IV can also increase your risk of DVT.
If you’re worried about developing deep vein thrombosis symptoms, schedule an evaluation with an experienced vein doctor. They can help identify your individual risks, recommend beneficial lifestyle changes, and perform treatments to improve blood flow.
Find A Vein Specialist Near You
DVT Risk Factors
Anyone can develop DVT, as blood clots occur in 900,000 people in the US each year, resulting in 60,000-100,000 deaths.³ However, there are risk factors that may make DVT more likely in individuals. Some people are more likely than others, especially if they have multiple risk factors.
These deep vein thrombosis risk factors include:
- Personal or family history of blood clots
- Varicose veins
- Obesity
- Pregnancy or recent childbirth
- Increasing age (risk rises after age 40)
- Elevated estrogen levels
If you are concerned about your risk for deep vein thrombosis, a vein specialist can assess your circulation, identify underlying vein disease, and recommend preventive steps or treatment.
Deep Vein Thrombosis (DVT) Symptoms
Vein health affects the risk of developing blood clots. Understanding the common deep vein thrombosis causes, signs, and symptoms can help you protect yourself and know when to seek medical assistance.
Deep vein thrombosis symptoms can cause excessive pain and impact mobility. Proper diagnosis is important because symptoms of a blood clot in the leg can resemble those of varicose veins. However, the first signs of a blood clot from DVT commonly occur on only one side of the body, typically in one leg or arm.
A few early signs of DVT include:
- Pain, tenderness, or cramping in one leg (often the calf)
- Swelling in one leg
- Skin that feels warm to the touch
- Red, purple, or discolored skin near the affected area
A DVT blood clot in the leg doesn’t always cause obvious symptoms. Some people do not notice their blood clot symptoms until they travel to the lungs, causing a pulmonary embolism. Symptoms of a pulmonary embolism (PE) include:
- Sudden shortness of breath
- Chest pain that worsens when you take a deep breath
- Dizziness
- Rapid breathing
- Rapid heart rate
DVT can be a serious condition, so if you notice swelling, pain, or skin changes in one leg, seek immediate medical care for a diagnosis and treatment to prevent serious complications.
Complications of DVT
Two major problems can happen after a blood clot forms in your leg. These complications of deep vein thrombosis include post-thrombotic syndrome and pulmonary embolism.¹
Post-thrombotic syndrome: When a blood clot obstructs blood flow, blood pressure upstream of the clot can rise dramatically, leading to leakage of blood and other materials from the veins, causing inflammation and skin issues.²
Pulmonary embolism: This occurs when a piece of a blood clot breaks away and travels to your lungs. This blood clot is called an embolism. It can obstruct blood flow and prevent the body from absorbing oxygen, posing a serious risk and requiring immediate treatment.
There are signs you can watch out for if you are experiencing any DVT complications. Go to the emergency room if you experience these blood clot symptoms, as they may indicate a pulmonary embolism:
- Sudden shortness of breath
- Chest pain that worsens with breathing
- Rapid heart rate
- Lightheadedness or fainting
- Coughing up blood
How Is Deep Vein Thrombosis Diagnosed?
Symptoms of DVT and pulmonary embolism can often overlap with other conditions, such as muscle strain, cellulitis, or varicose veins. As a result, you should visit a medical professional for an official diagnosis.
Doctors use several medical imaging methods to visualize blood flow, including ultrasound, X-rays, and blood tests.4 Once diagnosed, deep vein thrombosis treatment usually involves blood-thinning medications, along with additional interventions, to prevent complications or recurrence.
How to Prevent Deep Vein Thrombosis
While DVT is serious, it is often preventable. There are plenty of steps you can take to reduce the risk of clots forming and avoid the possible long-term effects of deep vein thrombosis.
Some ways you can prevent DVT include:
- Moving more frequently: Because blood clots often form during travel or when standing or sitting for long periods, moving at least every two hours can help reduce your risk.
- Exercising regularly: In addition to avoiding prolonged sitting and standing, aim for at least 30 minutes of activity per day, five days a week.
- Wearing loose-fitting clothing: Tight clothing can compress your veins, reducing circulation to your legs, so try wearing loose-fitting clothing when traveling or sitting for prolonged periods.
- Maintaining a healthy weight: Losing extra weight can alleviate pressure on your veins, lowering your risk for DVT.
- Quitting smoking: Smoking damages blood vessels, so quitting can help lower your risk for deep vein thrombosis.
- Wearing prescribed compression stockings: Medical-grade compression stockings can alleviate DVT symptoms, boost circulation, and reduce your risk of developing additional venous issues.
- Reviewing your medications: Certain medications may increase your risk for DVT. Discuss the pros and cons of your medications with your doctor.
- Treating underlying vein disease: If you have vein disease, one of the best ways to prevent DVT is to address venous insufficiency.
Understanding deep vein thrombosis and the treatment options available from providers like USA Vein Clinics can help address venous insufficiency.
How USA Vein Clinics Can Help
Preventing deep vein thrombosis starts with taking control of your health. Underlying vein disease, such as varicose veins, can increase the risk of DVT.
USA Vein Clinics has experienced vein specialists who diagnose and treat vein disease with patient-focused care. Our non-surgical treatments improve circulation with minimal downtime.
We accept insurance from many providers to cover our deep vein thrombosis treatments, including Medicare and Medicaid. With convenient online scheduling, bilingual phone support, and locations nationwide, we make it as easy as possible for you to access specialized vein care close to home.
FAQs about Deep Vein Thrombosis
Is deep vein thrombosis dangerous?
Deep vein thrombosis is dangerous, especially if it causes a pulmonary embolism (PE), which can damage lung tissue, lower oxygen levels, and potentially cause cardiac arrest. If you suspect you are experiencing a PE, you should seek immediate medical attention.
What does deep vein thrombosis feel like?
Deep vein thrombosis can cause throbbing pain and tender or hardened veins. DVT symptoms may resemble muscle strain or varicose veins, so seek medical evaluation if your symptoms persist or worsen.
Can you live with deep vein thrombosis?
You can live with deep vein thrombosis, although it typically involves long-term management methods like blood-thinning medication, compression therapy, and regular follow-ups to prevent complications.
References
- Kevin McLendon, Amandeep Goyal, and Maximos Attia, “Deep venous thrombosis risk factors,” in StatPearls [Internet] (Treasure Island, FL: StatPearls Publishing, 2017).
- Jeffrey J Farrell, Christopher Sutter, Sidhartha Tavri, and Indravadan Patel, “Incidence and interventions for post-thrombotic syndrome,” Cardiovascular Diagnosis and Therapy 6 no. 6 (2016): 623-631.
- “Data and statistics on venous thromboembolism,” US Centers for Disease Control and Prevention, last modified May 15, 2024.
- “Testing and diagnosis for venous thromboembolism,” US Centers for Disease Control and Prevention, last modified May 15, 2024.